Association of Geriatric Syndromes with Urinary Incontinence according to Sex and Urinary-Incontinence-Related Quality of Life in Older Inpatients: A Cross-Sectional Study of an Acute Care Hospital
- PMID: 30400699
- PMCID: PMC6669396
- DOI: 10.4082/kjfm.18.0011
Association of Geriatric Syndromes with Urinary Incontinence according to Sex and Urinary-Incontinence-Related Quality of Life in Older Inpatients: A Cross-Sectional Study of an Acute Care Hospital
Abstract
Background: Geriatric syndromes are associated with morbidity and poor quality of life (QOL). Urinary incontinence (UI) is one of the most prevalent geriatric syndromes. However, there is little research on the association of UI and UI-related QOL with other geriatric syndromes. We investigated the relationship between geriatric syndromes and UI according to gender and UI-related QOL among older inpatients.
Methods: This study was conducted among 444 older inpatients (aged 65 years and older) between October 2016 and July 2017. We examined geriatric syndromes and related factors involving cognitive impairment, delirium, depression, mobility decline, polypharmacy, undernutrition, pain, and fecal incontinence. UI-related QOL was assessed using the International Consultation on Incontinence Questionnaire-Short Form. Multiple logistic regression analysis was used to evaluate these associations.
Results: Geriatric syndromes and related factors were associated with UI. Mobility decline (odds ratio [OR], 4.16; 95% confidence interval [CI], 2.29-7.56), polypharmacy (OR, 3.35; 95% CI, 1.89-5.92), and pain (OR, 6.80; 95% CI, 3.53-13.09) were related to UI in both genders. Especially, delirium (OR, 7.55; 95% CI, 1.61-35.44) and fecal incontinence (OR, 10.15; 95% CI, 2.50-41.17) were associated with UI in men, while cognitive impairment (OR, 4.19; 95% CI, 1.14-15.44) was significantly associated with UI in women. Patients with depression were more likely to have poor UI-related QOL (OR, 8.54; 95% CI, 1.43-51.15).
Conclusion: UI was associated with different geriatric syndromes and related factors according to gender. Care for patients with depression, related to poor UI-related QOL, should be considered in primary care to improve the UI-related QOL of these individuals.
Keywords: Geriatric Syndrome; Inpatients; Older Adults; Urinary Incontinence.
Conflict of interest statement
No potential conflict of interest relevant to this article was reported.
Figures
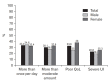
References
-
- Elsawy B, Higgins KE. The geriatric assessment. Am Fam Physician. 2011;83:48–56. - PubMed
-
- Hunskaar S, Burgio K, Diokno A, Herzog AR, Hjalmas K, Lapitan MC. Epidemiology and natural history of urinary incontinence in women. Urology. 2003;62(4 Suppl 1):16–23. - PubMed
-
- Coyne KS, Sexton CC, Irwin DE, Kopp ZS, Kelleher CJ, Milsom I. The impact of overactive bladder, incontinence and other lower urinary tract symptoms on quality of life, work productivity, sexuality and emotional well-being in men and women: results from the EPIC study. BJU Int. 2008;101:1388–95. - PubMed
-
- Milsom I, Coyne KS, Nicholson S, Kvasz M, Chen CI, Wein AJ. Global prevalence and economic burden of urgency urinary incontinence: a systematic review. Eur Urol. 2014;65:79–95. - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources

