Percutaneous Fixation by Internal Cemented Screw for the Treatment of Unstable Osseous Disease in Cancer Patients
- PMID: 30402006
- PMCID: PMC6218255
- DOI: 10.1055/s-0038-1673359
Percutaneous Fixation by Internal Cemented Screw for the Treatment of Unstable Osseous Disease in Cancer Patients
Abstract
Interventional radiology expertise in image guidance has expanded the treatment options for cancer patients with unstable osseous disease. Percutaneous fixation by internal cemented screw (FICS) describes the technique by which the interventional radiologist stabilizes a fracture or impending fracture with the percutaneous placement of a cannulated screw that is locked in position by polymethyl methacrylate cement. The durable metallic screws provide added resistance to torque and tension stresses that complement the axial compression resistance of cement. Compared with cementoplasty alone, the procedure has been advanced as a more durable and precise technique for stabilization of osseous disease for certain disease presentations in cancer patients. The application of advanced image guidance techniques improves upon existing percutaneous surgical techniques to facilitate approaches that would otherwise prove quite challenging, particularly with stabilization of the pelvic flat bones. This article examines the applications of percutaneous FICS procedures for the treatment of unstable osseous disease in cancer patients. Indications, techniques, and follow-up care are reviewed. Case examples in which FICS can be performed in unstable pathology are detailed.
Keywords: bone fracture; cement consolidation; cementoplasty; interventional radiology; pain palliation; screw fixation.
Figures
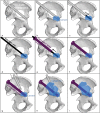
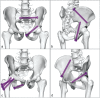
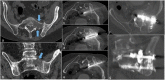
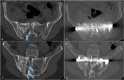
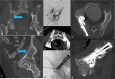
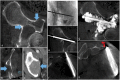
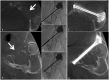
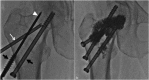
Similar articles
-
Prophylactic Percutaneous Consolidation of Large Osteolytic Tumors of the Pelvic Ring Using Fixation by Internal Cemented Screws.Radiol Imaging Cancer. 2021 May;3(3):e200137. doi: 10.1148/rycan.2021200137. Radiol Imaging Cancer. 2021. PMID: 33988476 Free PMC article.
-
CT guidance assisted by electromagnetic navigation system for percutaneous fixation by internal cemented screws (FICS).Eur Radiol. 2020 Feb;30(2):943-949. doi: 10.1007/s00330-019-06408-0. Epub 2019 Sep 2. Eur Radiol. 2020. PMID: 31478088
-
Image-guided Percutaneous Fixation with Internal Cemented Screws of Impending Femoral Neck Pathologic Fractures in Patients with Metastatic Cancer: Safety, Efficacy, and Durability.Radiology. 2020 Dec;297(3):721-729. doi: 10.1148/radiol.2020201341. Epub 2020 Oct 6. Radiology. 2020. PMID: 33021894
-
[Image-guided bone consolidation in oncology: Cementoplasty and percutaneous screw fixation].Bull Cancer. 2017 May;104(5):423-432. doi: 10.1016/j.bulcan.2016.12.009. Epub 2017 Mar 18. Bull Cancer. 2017. PMID: 28320522 Review. French.
-
Percutaneous Cement Injection for the Palliative Treatment of Osseous Metastases: A Technical Review.Semin Intervent Radiol. 2018 Oct;35(4):268-280. doi: 10.1055/s-0038-1673418. Epub 2018 Nov 5. Semin Intervent Radiol. 2018. PMID: 30402010 Free PMC article. Review.
Cited by
-
Different polymethylmethacrylate (PMMA) reinforcement strategies for long bone osteoplasty procedures: a controlled laboratory comparison using the 4-point bending test.BMC Musculoskelet Disord. 2024 Dec 21;25(1):1058. doi: 10.1186/s12891-024-08148-9. BMC Musculoskelet Disord. 2024. PMID: 39709357 Free PMC article.
-
Combined Angio-CT Systems: A Roadmap Tool for Precision Therapy in Interventional Oncology.Radiol Imaging Cancer. 2021 Sep;3(5):e210039. doi: 10.1148/rycan.2021210039. Radiol Imaging Cancer. 2021. PMID: 34559007 Free PMC article. Review.
-
Combined vertebroplasty and pedicle screw insertion for vertebral consolidation: feasibility and technical considerations.Neuroradiology. 2024 May;66(5):855-863. doi: 10.1007/s00234-024-03325-y. Epub 2024 Mar 8. Neuroradiology. 2024. PMID: 38453715
-
Prophylactic Percutaneous Consolidation of Large Osteolytic Tumors of the Pelvic Ring Using Fixation by Internal Cemented Screws.Radiol Imaging Cancer. 2021 May;3(3):e200137. doi: 10.1148/rycan.2021200137. Radiol Imaging Cancer. 2021. PMID: 33988476 Free PMC article.
-
Percutaneous Management of Cancer Pain.Curr Oncol Rep. 2020 Apr 16;22(5):43. doi: 10.1007/s11912-020-00906-x. Curr Oncol Rep. 2020. PMID: 32297006 Review.
References
-
- Hill T, D'Alessandro P, Murray K, Yates P. Prognostic factors following pathological fractures. ANZ J Surg. 2015;85(03):159–163. - PubMed
-
- Kaemmerlen P, Thiesse P, Bouvard H, Biron P, Mornex F, Jonas P. [Percutaneous vertebroplasty in the treatment of metastases. Technic and results] J Radiol. 1989;70(10):557–562. - PubMed
-
- Anselmetti G C, Marcia S, Saba L et al.Percutaneous vertebroplasty: multi-centric results from EVEREST experience in large cohort of patients. Eur J Radiol. 2012;81(12):4083–4086. - PubMed
-
- Wang Z, Zhen Y, Wu C et al.CT fluoroscopy-guided percutaneous osteoplasty for the treatment of osteolytic lung cancer bone metastases to the spine and pelvis. J Vasc Interv Radiol. 2012;23(09):1135–1142. - PubMed

