Association between Early Neuroretinal Dysfunction and Peripheral Motor Unit Loss in Patients with Type 1 Diabetes Mellitus
- PMID: 30402503
- PMCID: PMC6193343
- DOI: 10.1155/2018/9763507
Association between Early Neuroretinal Dysfunction and Peripheral Motor Unit Loss in Patients with Type 1 Diabetes Mellitus
Abstract
Objectives: It has been already confirmed that retinal neurodegeneration has a predictive value in the development of microvascular alterations in diabetic retinopathy. However, no data are available on the association between neuroretinal dysfunction and peripheral motor unit loss. Our study, therefore, was aimed at investigating the hypothesis that retinal neurodegeneration could be considered an early marker of diabetic peripheral neuropathy (DPN).
Methods: 20 T1DM patients with no symptoms/signs of peripheral polyneuropathy, without DR or with very mild nonproliferative DR, and 14 healthy controls (C) age- and gender-matched were enrolled. The following electrophysiological tests were performed: standard nerve conduction studies (NCS) and incremental motor unit number estimation (MUNE) from the abductor hallux (AH) and abductor digiti minimi (ADM). Neuroretinal function was studied by multifocal electroretinogram (MfERG) recordings, measuring response amplitude density (RAD) and implicit time (IT) from rings and sectors of superior (S)/inferior (I)/temporal (T)/nasal (N) macular sectors up to 10 degrees of foveal eccentricity.
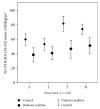
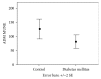
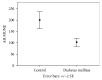
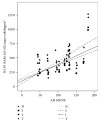
Results: MfERG RADs from rings and sectors were significantly reduced in T1DM (p < 0.05) vs. C. ADM MUNE and AH MUNE were significantly decreased in T1DM (p = 0.039 and p < 0.0001, respectively) vs. C. A positive correlation between mean MfERG RADs from the central 5 degrees of the four (S, I, T, and N) macular sectors and lower limb motor unit number (r = 0.50, p = 0.041; r = 0.64, p = 0.005; r = 0.64, p = 0.006; and r = 0.61, p = 0.010, respectively) was observed in T1DM patients. No abnormalities of NCS were found in any subject.
Conclusions: The motor unit loss on the one hand and neuroretinal dysfunction on the other hand are already present in T1DM patients without DPN. The relationship between neuroretinal dysfunction and motor unit decline supports the hypothesis that neuroretina may represent a potential "window" to track the early neurogenic damage in diabetes.
Figures
Similar articles
-
Early and localized retinal dysfunction in patients with type 1 diabetes mellitus studied by multifocal electroretinogram.Acta Diabetol. 2018 Nov;55(11):1191-1200. doi: 10.1007/s00592-018-1209-9. Epub 2018 Aug 28. Acta Diabetol. 2018. PMID: 30159747
-
Early detection of retinal dysfunction in type 1 diabetes without retinopathy using multifocal electroretinography.Sci Rep. 2025 Feb 21;15(1):6379. doi: 10.1038/s41598-025-89734-2. Sci Rep. 2025. PMID: 39984539 Free PMC article.
-
MScanFit motor unit number estimation and muscle velocity recovery cycle recordings in diabetic polyneuropathy.Clin Neurophysiol. 2020 Nov;131(11):2591-2599. doi: 10.1016/j.clinph.2020.07.017. Epub 2020 Aug 15. Clin Neurophysiol. 2020. PMID: 32927215
-
Multifocal electroretinogram responses in Nepalese diabetic patients without retinopathy.Doc Ophthalmol. 2014 Aug;129(1):39-46. doi: 10.1007/s10633-014-9447-9. Epub 2014 Jun 5. Doc Ophthalmol. 2014. PMID: 24898184
-
A multifocal electroretinogram model predicting the development of diabetic retinopathy.Prog Retin Eye Res. 2006 Sep;25(5):425-48. doi: 10.1016/j.preteyeres.2006.07.001. Epub 2006 Sep 1. Prog Retin Eye Res. 2006. PMID: 16949855 Free PMC article. Review.
Cited by
-
Diabetes Mellitus-Related Dysfunction of the Motor System.Int J Mol Sci. 2020 Oct 11;21(20):7485. doi: 10.3390/ijms21207485. Int J Mol Sci. 2020. PMID: 33050583 Free PMC article. Review.
-
Aberrant Neurovascular Coupling in Diabetic Retinopathy Using Arterial Spin Labeling (ASL) and Functional Magnetic Resonance Imaging (fMRI) methods.Diabetes Metab Syndr Obes. 2024 Jul 26;17:2809-2822. doi: 10.2147/DMSO.S465103. eCollection 2024. Diabetes Metab Syndr Obes. 2024. PMID: 39081370 Free PMC article.
-
Gynura divaricata Water Extract Presented the Possibility to Enhance Neuronal Regeneration.Evid Based Complement Alternat Med. 2021 Feb 17;2021:8818618. doi: 10.1155/2021/8818618. eCollection 2021. Evid Based Complement Alternat Med. 2021. PMID: 33680064 Free PMC article.
-
The proteasome as a druggable target with multiple therapeutic potentialities: Cutting and non-cutting edges.Pharmacol Ther. 2020 Sep;213:107579. doi: 10.1016/j.pharmthera.2020.107579. Epub 2020 May 19. Pharmacol Ther. 2020. PMID: 32442437 Free PMC article.
-
Redefining distal symmetrical polyneuropathy features in type 1 diabetes: a systematic review.Acta Diabetol. 2022 Jan;59(1):1-19. doi: 10.1007/s00592-021-01767-x. Epub 2021 Jul 2. Acta Diabetol. 2022. PMID: 34213655 Free PMC article.
References
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

