Primary PCI versus pharmacoinvasive strategy for ST elevation myocardial infarction
- PMID: 30402534
- PMCID: PMC6205251
- DOI: 10.1016/j.ijcha.2018.10.006
Primary PCI versus pharmacoinvasive strategy for ST elevation myocardial infarction
Abstract
Background: The rationale for pharmacoinvasive strategy is that many patients have a persistent reduction in flow in the infarct-related artery. The aim of the present study is to assess safety and efficacy of pharmacoinvasive strategy using streptokinase compared to primary PCI and ischemia driven PCI on degree of myocardial salvage and outcomes.
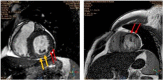
Methods and results: Sixty patients with 1st attack of acute STEMI within 12 h were randomized to 4 groups: primary PCI for patients presented to PPCI-capable centers (group I), transfer to PCI if presented to non-PCI capable center (group II), pharmacoinvasive strategy "Streptokinase followed by PCI within 3-24 h" (group III) and fibrinolytic followed by ischemia driven PCI (group IV). The primary endpoint is the infarction size and microvascular obstruction (MVO) measured by cardiac MRI (CMR) 3-5 days post-MI. Pharmacoinvasive strategy led to a significant reduction in infarction size, MVO and major adverse cardiac and cerebrovascular event (MACCE) compared to group IV but minor bleeding was significantly higher compared to other groups.
Conclusions: Pharmacoinvasive strategy resulted in effective reperfusion and smaller infarction size in patients with early STEMI who could not undergo primary PCI within 2 h after the first medical contact. This can provide a wide time window for PCI when the application of primary PCI within the optimal time limit is not possible. However, it was associated with a slightly increased risk of minor bleeding.
Keywords: Cardiac MRI (CMR); Infarction size; Microvascular obstruction (MVO); Pharmacoinvasive strategy; Primary PCI.
Figures

References
-
- Cantor W., Fitchett D., Borgundvaag B., Ducas J., Heffernan M., Cohen E., for the TRANSFER-AMI Trial Investigators Routine early angioplasty after fibrinolysis for acute myocardial infarction. NEJM. 2009;360:2705–2718. - PubMed
-
- Armstrong P., Gershlick A., Goldstein P., Wilcox R., Danays T., Bluhmki E. The Strategic Reperfusion Early after Myocardial Infarction (STREAM) study. Am. Heart J. 2010;160(1):30–35. - PubMed
-
- Aviles F., Alonso J., Beiras A., Vázquez N., Blanco J., Briales J. Routine invasive strategy within 24 hours of thrombolysis versus ischemia-guided conservative approach for acute myocardial infarction with ST-segment elevation (GRACIA-1) Lancet. 2004;364:1045–1053. - PubMed
-
- Borgia F., Goodman S., Halvorsen S., Cantor W., Piscione F., Le May M., Aviles F. Early routine percutaneous coronary intervention after fibrinolysis vs. standard therapy in ST-segment elevation myocardial infarction: a meta-analysis. Eur. Heart J. 2010;31:2156–2169. - PubMed
-
- Ibanez B., James S., Agewall S., Antunes M., Bucciarelli-Ducci C., Bueno H., Caforio A. 2017 ESC guidelines for the management of acute myocardial infarction in patients presenting with ST-segment elevation. Eur. Heart J. 2018;39:119–177. - PubMed
LinkOut - more resources
Full Text Sources
Miscellaneous

