Associations Between Breast Cancer Survivorship and Adverse Mental Health Outcomes: A Systematic Review
- PMID: 30403799
- PMCID: PMC6292797
- DOI: 10.1093/jnci/djy177
Associations Between Breast Cancer Survivorship and Adverse Mental Health Outcomes: A Systematic Review
Erratum in
-
Corrigendum.J Natl Cancer Inst. 2020 Jan 1;112(1):118. doi: 10.1093/jnci/djz059. J Natl Cancer Inst. 2020. PMID: 31329923 Free PMC article. No abstract available.
Abstract
Background: We aimed to systematically review the evidence on adverse mental health outcomes in breast cancer survivors (≥1 year) compared with women with no history of cancer.
Methods: Studies were identified by searching MEDLINE, PsycINFO, the Cumulative Index to Nursing and Allied Health Literature, and the Social Sciences Citation Index, and through backward citation tracking. Two researchers selected the studies, extracted data, and assessed the risk of bias.
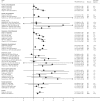
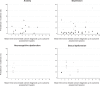
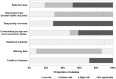
Results: Sixty studies were included. Of 38 studies of depression, 33 observed more depression in breast cancer survivors; this was statistically significant in 19 studies overall, including six of seven where depression was ascertained clinically, three of four studies of antidepressants, and 13 of 31 that quantified depressive symptoms. Of 21 studies of anxiety, 17 observed more anxiety in breast cancer survivors, statistically significant in 11 studies overall, including two of four with clinical/prescription-based outcomes, and in eight of 17 of anxiety symptoms. Breast cancer survivors also had statistically significantly increased symptoms/frequency of neurocognitive dysfunction (18 of 24 studies), sexual dysfunctions (5 of 6 studies), sleep disturbance (5 of 5 studies), stress-related disorders/PTSD (2 of 3 studies), suicide (2 of 2 studies), somatisation (2 of 2 studies), and bipolar and obsessive-compulsive disorders (1 of 1 study each). Studies were heterogeneous in terms of participants' characteristics, time since diagnosis, ascertainment of outcomes, and measures reported. Approximately one-half of the studies were at high risk of selection bias and confounding by socio-economic status.
Conclusions: There is compelling evidence of an increased risk of anxiety, depression and suicide, and neurocognitive and sexual dysfunctions in breast cancer survivors compared with women with no prior cancer. This information can be used to support evidence-based prevention and management strategies. Further population-based and longitudinal research would help to better characterize these associations.
Figures

Comment in
-
Response to Hulliard, Le Strat, Dubertre, et al.J Natl Cancer Inst. 2019 Mar 1;111(3):337. doi: 10.1093/jnci/djz004. J Natl Cancer Inst. 2019. PMID: 30629200 Free PMC article. No abstract available.
-
RE: Associations Between Breast Cancer Survivorship and Adverse Mental Health Outcomes: A Systematic Review.J Natl Cancer Inst. 2019 Mar 1;111(3):335-336. doi: 10.1093/jnci/djz003. J Natl Cancer Inst. 2019. PMID: 30629204 No abstract available.
-
Mental health care of patients with breast cancer in Bangladesh.Lancet Psychiatry. 2021 Jan;8(1):18-19. doi: 10.1016/S2215-0366(20)30494-6. Lancet Psychiatry. 2021. PMID: 33341163 No abstract available.
References
-
- Ervik M, Lam F, Ferlay J, et al. Population fact sheets: breast cancer prevalence (5 years) very high and high HDI. http://gco.iarc.fr/today/fact-sheets-cancers?cancer=15&type=0&sex=2. Accessed 1 May 2018.
-
- Payne DK, Sullivan MD, Massie MJ.. Women's psychological reactions to breast cancer. Semin Oncol. 1996;23(1 suppl 2):89–97. - PubMed
-
- Al-Azri M, Al-Awisi H, Al-Moundhri M.. Coping with a diagnosis of breast cancer-literature review and implications for developing countries. Breast J. 2009;156:615–622. - PubMed

