Local regression and control of T1-2 nasopharyngeal carcinoma treated with intensity-modulated radiotherapy
- PMID: 30406969
- PMCID: PMC6308044
- DOI: 10.1002/cam4.1866
Local regression and control of T1-2 nasopharyngeal carcinoma treated with intensity-modulated radiotherapy
Abstract
Objective: To observe the local regression and control in T1-2 nasopharyngeal carcinoma (NPC) patients treated with intensity-modulated radiotherapy (IMRT) and to analyze the related influencing factors.
Methods: Between January 2006 and June 2014, 247 consecutive T1-2 NPC patients treated with IMRT were retrospectively analyzed, with 126 (51.0%) N0-1 disease and 121 (49.0%) N2-3 disease. Among them, 72.9% received platinum-based chemotherapy. The prescribed dose to gross tumor volume was 66 Gy/30 fractions.
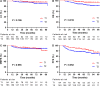
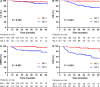
Results: By the end of IMRT, the chemoradiotherapy (CRT) group had higher local complete response (CR) rate compared with IMRT alone group (92.2% vs 74.6%, P < 0.001), but no significant difference was discovered in 5-year local control (LC) rate (95.1% vs 94.9%, P = 0.968). Of the rest 31 patients with residual nasopharyngeal lesions after IMRT, those received boost irradiation (67.7%) also showed no improvement in 5-year LC rate compared with the observational group (95.0% vs 100.0%, P = 0.307). With a median follow-up of 63 months, the estimated 5-year LC rate for the whole group was 95.1% (T1 vs T2: 95.9% vs 94.7%, P = 0.186). Prognostic factors for LC were found neither in univariate nor in multivariate analysis. Advanced N stage was found to be the only adverse prognostic factor for all the other survivals.
Conclusions: Excellent LC could be achieved in T1-2 NPC treated with IMRT. The addition of chemotherapy may offer short-term response benefit, but no significant LC benefit, so did boost irradiation. Attention should be attached to advanced N stage, the exploration of the recurrence-related factors, and the necessities of the additional treatment.
Keywords: T1-2 nasopharyngeal carcinoma; boost irradiation; chemotherapy; local control.
© 2018 The Authors. Cancer Medicine published by John Wiley & Sons Ltd.
Figures
References
-
- Lee AW, Ma BB, Ng WT, Chan AT. Management of Nasopharyngeal Carcinoma: Current Practice and Future Perspective. J Clin Oncol. 2015;33:3356‐3364. - PubMed
-
- Blanchard P, Lee A, Marguet S, et al. Chemotherapy and radiotherapy in nasopharyngeal carcinoma: an update of the MAC‐NPC meta‐analysis. Lancet Oncol. 2015;16:645‐655. - PubMed
-
- Al‐Sarraf M, LeBlanc M, Giri PG, et al. Chemoradiotherapy versus radiotherapy in patients with advanced nasopharyngeal cancer: phase III randomized Intergroup study 0099. J Clin Oncol. 1998;16:1310‐1317. - PubMed
-
- Lu H, Yao M. The current status of intensity‐modulated radiation therapy in the treatment of nasopharyngeal carcinoma. Cancer Treat Rev. 2008;34:27‐36. - PubMed
-
- Kam MK, Chau RM, Suen J, Choi PH, Teo PM. Intensity‐modulated radiotherapy in nasopharyngeal carcinoma: dosimetric advantage over conventional plans and feasibility of dose escalation. Int J Radiat Oncol Biol Phys. 2003;56:145‐157. - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Research Materials

