The effects of a forced-air warming system plus electric blanket for elderly patients undergoing transurethral resection of the prostate: A randomized controlled trial
- PMID: 30407328
- PMCID: PMC6250554
- DOI: 10.1097/MD.0000000000013119
The effects of a forced-air warming system plus electric blanket for elderly patients undergoing transurethral resection of the prostate: A randomized controlled trial
Abstract
Background: Perioperative inadvertent hypothermia in elderly urology patients undergoing transurethral resection of the prostate (TURP) is a well-known serious complication, as it increases the risk of myocardial ischemia, blood loss, and surgical wound infection. We conducted this prospective randomized controlled trial to evaluate the combined effect of a forced-air warming system and electric blanket in elderly TURP patients.
Methods: Between January 2015 and October 2017, we recruited 443 elderly male patients undergoing elective TURP with subarachnoid blockade (SAB). These were randomly divided into 3 groups: group E (intraoperative warming using electric blankets set to 38°C; n = 128); group F (intraoperative warming using a forced-air warmer set to 38°C; n = 155) and group FE (intraoperative warming using a forced-air warmer plus electric blankets, both set to 38°C; n = 160). The primary outcome was shivering and their grades. Hemodynamic changes, esophageal temperature, recovery time, incidences of adverse effects, and patient and surgeon satisfaction were also recorded.
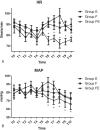
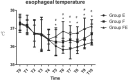
Results: Baseline characteristics showed no significant differences when compared across the 3 groups (P >.05). Compared with groups E and F, both HR and mean arterial pressure (MAP) in group FE were significantly decreased from T6 to T10 (P <.05). Compared with groups E and F, esophageal temperature in group FE increased significantly from T5 to T10 (P <.05). Compared with group E, esophageal temperature in group F was significantly increased from T5 to T10 (P <.05). Compared with groups F and FE, post-anesthesia care unit (PACU) recovery time was longer in group E, while compared with group F, PACU recovery time was shorter in group FE (P <.05). Compared to patients in groups E and F, those in group FE had a significantly lower incidence of arrhythmia and shivering (P <.05). The number of patients with shivering grades 0 to 3 was higher in group E than in other groups, while the number of patients with shivering grade 2 was significantly higher in group F than in group FE (P <.05). Patient and surgeon satisfaction scores were higher in group FE than in groups E and F (P <.05).
Conclusions: Use of a forced-air warming system combined with an electric blanket was an effective method with which to retain warmth among elderly TURP patients.
Conflict of interest statement
The authors declare that this research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
References
-
- John M, Crook D, Dasari K, et al. Comparison of resistive heating and forced-air warming to prevent inadvertentperioperative hypothermia. Br J Anaesth 2016;116:249–54. - PubMed
-
- Grigore AM, Murray CF, Ramakrishna H, et al. A core review of temperature regimens and neuro protection during cardiopulmonary bypass: does rewarming rate matter. Anesth Analg 2009;109:1741–51. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Research Materials

