Risk factors associated with prolonged hospital length-of-stay: 18-year retrospective study of hospitalizations in a tertiary healthcare center in Mexico
- PMID: 30408118
- PMCID: PMC6224124
- DOI: 10.1371/journal.pone.0207203
Risk factors associated with prolonged hospital length-of-stay: 18-year retrospective study of hospitalizations in a tertiary healthcare center in Mexico
Erratum in
-
Correction: Risk factors associated with prolonged hospital length-of-stay: 18-year retrospective study of hospitalizations in a tertiary healthcare center in Mexico.PLoS One. 2018 Dec 21;13(12):e0209944. doi: 10.1371/journal.pone.0209944. eCollection 2018. PLoS One. 2018. PMID: 30576394 Free PMC article.
Abstract
Background: Hospital length-of-Stay has been traditionally used as a surrogate to evaluate healthcare efficiency, as well as hospital resource utilization. Prolonged Length-of-stay (PLOS) is associated with increased mortality and other poor outcomes. Additionally, these patients represent a significant economic problem on public health systems and their families. We sought to describe and compare characteristics of patients with Normal hospital Length-of-Stay (NLOS) and PLOS to identify sociodemographic and disease-specific factors associated with PLOS in a tertiary care institution that attends adults with complicated diseases from all over Mexico.
Materials and methods: We conducted a retrospective analysis of hospital discharges from January 2000-December 2017 using institutional databases of medical records. We compared NLOS and PLOS using descriptive and inferential statistics. PLOS were defined as those above the 95th percentile of length of hospitalization.
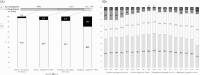
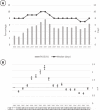
Results: We analyzed 85,904 hospitalizations (1,069,875 bed-days), of which 4,427 (5.1%) were PLOS (247,428 bed-days, 23.1% of total bed-days). Hematological neoplasms were the most common discharge diagnosis and surgery of the small bowel was the most common type of surgery. Younger age, male gender, a lower physician-to-patient ratio, emergency and weekend admissions, surgery, the number of comorbidities, residence outside Mexico City and lower socioeconomic status were associated with PLOS. Bone marrow transplant (OR 18.39 [95% CI 12.50-27.05, p<0.001), complex infectious diseases such as systemic mycoses and parasitoses (OR 4.65 [95% CI 3.40-6.63, p<0.001), and complex abdominal diseases such as intestinal fistula (OR 2.57 [95% CI 1.98-3.32) had the greatest risk for PLOS. Risk of mortality in patients with PLOS increased more than threefold (3.7% vs 13.3%, p<0.001).
Conclusions: We report some key sociodemographic and disease-specific differences in patients with PLOS. These could serve to develop a specific model of directed hospital healthcare for patients identified as in risk of PLOS.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures

References
-
- World Health Organization. Global Health Expenditure Database. Accesed on 07/19/2016. Available at http://apps.who.int/nha/database/Country_Profile/Index/en.
-
- Marshall A, Vasilakis C, El-Darzi E. Length of stay-based patient flow models: recent developments and future directions. Health Care Manag Sci. 2005;8(3):213–20. . - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources

