Timing of anticoagulation after recent ischaemic stroke in patients with atrial fibrillation
- PMID: 30415934
- PMCID: PMC6524642
- DOI: 10.1016/S1474-4422(18)30356-9
Timing of anticoagulation after recent ischaemic stroke in patients with atrial fibrillation
Abstract
Background: About 13-26% of all acute ischaemic strokes are related to non-valvular atrial fibrillation, the most common cardiac arrhythmia globally. Deciding when to initiate oral anticoagulation in patients with non-valvular atrial fibrillation is a longstanding, common, and unresolved clinical challenge. Although the risk of early recurrent ischaemic stroke is high in this population, early oral anticoagulation is suspected to increase the risk of potentially harmful intracranial haemorrhage, including haemorrhagic transformation of the infarct. This assumption, and current treatment guidelines, are based on historical, mostly observational data from patients with ischaemic stroke and atrial fibrillation treated with heparins, heparinoids, or vitamin K antagonists (VKAs) to prevent recurrent ischaemic stroke. Randomised controlled trials have subsequently shown that direct oral anticoagulants (DOACs; ie, apixaban, dabigatran, edoxaban, and rivaroxaban) are at least as effective as VKAs in primary and secondary prevention of atrial fibrillation-related ischaemic stroke, with around half the risk of intracranial haemorrhage. However, none of these DOAC trials included patients who had experienced ischaemic stroke recently (within the first few weeks). Clinicians therefore remain uncertain regarding when to commence DOAC administration after acute ischaemic stroke in patients with atrial fibrillation.
Recent developments: Prospective observational studies and two small randomised trials have investigated the risks and benefits of early DOAC-administration initiation (most with a median delay of 3-5 days) in mild-to-moderate atrial fibrillation-associated ischaemic stroke. These studies reported that early DOAC treatment was associated with a low frequency of clinically symptomatic intracranial haemorrhage or surrogate haemorrhagic lesions on MRI scans, whereas later DOAC-administration initiation (ie, >7 days or >14 days after index stroke) was associated with an increased frequency of recurrent ischaemic stroke. WHERE NEXT?: Adequately powered randomised controlled trials comparing early to later oral anticoagulation with DOACs in ischaemic stroke associated with atrial fibrillation are justified to confirm the acceptable safety and efficacy of this strategy. Four such randomised controlled trials (collectively planned to include around 9000 participants) are underway, either using single cutoff timepoints for early versus late DOAC-administration initiation, or selecting DOAC-administration timing according to the severity and imaging features of the ischaemic stroke. The results of these trials should help to establish the optimal timing to initiate DOAC administration after recent ischaemic stroke and whether the timing should differ according to stroke severity. Results of these trials are expected from 2021.
Copyright © 2019 Elsevier Ltd. All rights reserved.
Figures
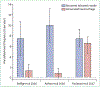

References
-
- Bejot Y, Ben Salem D, Osseby GV, et al. Epidemiology of ischemic stroke from atrial fibrillation in Dijon, France, from 1985 to 2006. Neurology 2009; 72: 346–53. - PubMed
-
- Grau AJ, Weimar C, Buggle F, et al. Risk factors, outcome, and treatment in subtypes of ischemic stroke: the German stroke data bank. Stroke 2001; 32: 2559–66. - PubMed
-
- Mozaffarian D, Benjamin EJ, Go AS, et al. Heart disease and stroke statistics—2015 update: a report from the American Heart Association. Circulation 2015; 131: e29–322. - PubMed
-
- Wolf PA, Abbott RD, Kannel WB. Atrial fibrillation as an independent risk factor for stroke: the Framingham Study. Stroke 1991; 22: 983–8. - PubMed
-
- Hart RG, Coull BM, Hart D. Early recurrent embolism associated with nonvalvular atrial fibrillation: a retrospective study. Stroke 1983; 14: 688–93. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

