Prospective Validation of a Checklist to Predict Short-term Death in Older Patients After Emergency Department Admission in Australia and Ireland
- PMID: 30428145
- PMCID: PMC6619350
- DOI: 10.1111/acem.13664
Prospective Validation of a Checklist to Predict Short-term Death in Older Patients After Emergency Department Admission in Australia and Ireland
Abstract
Background: Emergency departments (EDs) are pressured environment where patients with supportive and palliative care needs may not be identified. We aimed to test the predictive ability of the CriSTAL (Criteria for Screening and Triaging to Appropriate aLternative care) checklist to flag patients at risk of death within 3 months who may benefit from timely end-of-life discussions.
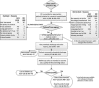
Methods: Prospective cohorts of >65-year-old patients admitted for at least one night via EDs in five Australian hospitals and one Irish hospital. Purpose-trained nurses and medical students screened for frailty using two instruments concurrently and completed the other risk factors on the CriSTAL tool at admission. Postdischarge telephone follow-up was used to determine survival status. Logistic regression and bootstrapping techniques were used to test the predictive accuracy of CriSTAL for death within 90 days of admission as primary outcome. Predictability of in-hospital death was the secondary outcome.
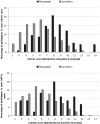
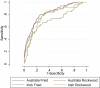
Results: A total of 1,182 patients, with median age 76 to 80 years (IRE-AUS), were included. The deceased had significantly higher mean CriSTAL with Australian mean of 8.1 (95% confidence interval [CI] = 7.7-8.6) versus 5.7 (95% CI = 5.1-6.2) and Irish mean of 7.7 (95% CI = 6.9-8.5) versus 5.7 (95% CI = 5.1-6.2). The model with Fried frailty score was optimal for the derivation (Australian) cohort but prediction with the Clinical Frailty Scale (CFS) was also good (areas under the receiver-operating characteristic [AUROC] = 0.825 and 0.81, respectively). Values for the validation (Irish) cohort were AUROC = 0.70 with Fried and 0.77 using CFS. A minimum of five of 29 variables were sufficient for accurate prediction, and a cut point of 7+ or 6+ depending on the cohort was strongly indicative of risk of death. The most significant independent predictor of short-term death in both cohorts was frailty, carrying a twofold risk of death. CriSTAL's accuracy for in-hospital death prediction was also good (AUROC = 0.795 and 0.81 in Australia and Ireland, respectively), with high specificity and negative predictive values.
Conclusions: The modified CriSTAL tool (with CFS instead of Fried's frailty instrument) had good discriminant power to improve certainty of short-term mortality prediction in both health systems. The predictive ability of models is anticipated to help clinicians gain confidence in initiating earlier end-of-life discussions. The practicalities of embedding screening for risk of death in routine practice warrant further investigation.
© 2018 The Authors. Academic Emergency Medicine published by Wiley Periodicals, Inc. on behalf of Society for Academic Emergency Medicine (SAEM).
Figures
Comment in
-
Hot Off the Press: Prospective Validation of a Checklist to Predict Short-term Death in Older Patients After ED Admission in Australia and Ireland.Acad Emerg Med. 2019 Nov;26(11):1289-1291. doi: 10.1111/acem.13845. Epub 2019 Sep 9. Acad Emerg Med. 2019. PMID: 31392777 No abstract available.
References
-
- Lamba S, Nagurka R, Murano T, Zalenski RJ, Compton S. Early identification of dying trajectories in emergency department patients: potential impact on hospital care. J Palliat Med 2012;15:392–5. - PubMed
-
- Galvin R, Gilleit Y, Wallace E, et al. Adverse outcomes in older adults attending emergency departments: a systematic review and meta‐analysis of the Identification of Seniors At Risk (ISAR) screening tool. Age Ageing 2017;46:179–86. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources