Has the risk of dislocation after total hip arthroplasty performed for displaced femoral neck fracture improved with modern implants?
- PMID: 30449970
- PMCID: PMC6224700
- DOI: 10.1016/j.jcot.2017.09.002
Has the risk of dislocation after total hip arthroplasty performed for displaced femoral neck fracture improved with modern implants?
Abstract
Background: Displaced femoral neck fractures (DFNF) in the elderly can be treated with hemiarthroplasty or total hip arthroplasty (THA). One concern with utilizing THA in this setting is post-operative dislocation. The purposes of this study were to determine the incidence of hip dislocation following THA for DFNF and to identify risk factors for dislocation.
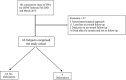
Methods: The charts of 66 posterior-approach THA cases performed for DFNF with mean post-operative follow-up of 4.4 years were retrospectively reviewed. Pre-operative patient demographic data and intra-operative clinical data were recorded including age, race, gender, height, weight, body mass index (BMI), femoral head diameter, acetabular cup diameter, use of an elevated liner, and cementing of femoral component. For patients with available post-operative pelvis radiographs, acetabular cup inclination and version angles were also calculated.
Results: Four dislocation (4/66, 6%) events occurred at an average of 51 days after surgery. No specific risk factors for dislocation were identified but the use of a cemented femoral stem did approach significance (p = 0.06). 47% of the acetabular cups were located outside of the Lewinnek safe zone. Although the dislocation rate of THAs with acetabular cups outside of the safe zone was higher than the dislocation rate for THAs with cups in the safe zone (12.5% vs 0%), placement of acetabular cups outside of the safe zone was not a risk factor for dislocation.
Conclusions: Posterior THA with proper cup positioning and meticulous soft tissue repair is an effective treatment option for DFNF with low dislocation risk.
Keywords: Acetabular cup positioning; Dislocation; Femoral neck fracture; Total hip arthroplasty.
Figures
References
-
- Cummings S.R., Rubin S.M., Black D. The future of hip fractures in the United States. Numbers, costs, and potential effects of postmenopausal estrogen. Clin Orthop Relat Res. 1990;252:163–166. - PubMed
-
- Parker M.J., Pryor G.A. Internal fixation or arthroplasty for displaced cervical hip fractures in the elderly: a randomised controlled trial of 208 patients. Acta Orthop Scand. 2000;71(5):440–446. - PubMed
-
- Tidermark J. Internal fixation compared with total hip replacement for displaced femoral neck fractures in the elderly. A randomised, controlled trial. J Bone Joint Surg Br. 2003;85(3):380–388. - PubMed
-
- Iorio R. Surgical treatment of displaced femoral neck fractures in the elderly: a survey of the American Association of Hip and Knee Surgeons. J Arthroplasty. 2006;21(8):1124–1133. - PubMed
-
- Low A.K., Gursel A.C. Mid-term outcome of total hip replacement using the posterior approach for displaced femoral neck fractures. Hip Int. 2012;22(2):203–208. - PubMed
LinkOut - more resources
Full Text Sources