Functional Subunit Reconstruction of Giant Facial Congenital Melanocytic Nevi in Children With the Use of Matriderm and Skin Graft: Surgical Experience and Literature Review
- PMID: 30455780
- PMCID: PMC6232950
Functional Subunit Reconstruction of Giant Facial Congenital Melanocytic Nevi in Children With the Use of Matriderm and Skin Graft: Surgical Experience and Literature Review
Abstract
Introduction: Facial giant congenital melanocytic nevus represents a major cosmetic deformity for the child and parents and is a challenge for the plastic surgeons to achieve best cosmetic results. Herein, we present a case of single-stage surgical reconstruction using partial-thickness scalp skin graft aided with Matriderm dermal substitute for a facial giant congenital melanocytic nevus. Methods: An 8-year-old boy presented with a facial giant congenital melanocytic nevus without leptomeningeal involvement. A single-stage complete excision of the nevus was performed. A split-thickness skin graft, 12/1000-inch thick, was then harvested from the anterior scalp region for reconstruction. A 1-mm Matriderm dermal substitute was first applied, on which functional subunit skin graft was then secured to cover the defect. Eyelid reconstruction was reconstructed separately using full-thickness postauricular skin grafts. Results: Histopathology of the excised specimen confirmed the diagnosis of congenital melanocytic nevus, with no evidence of melanoma. The donor area healed with a favorable scar and no donor site morbidity or complications such as alopecia or hypertrophic scar. The postoperative result was satisfactory with minimal residual nevus around the eye, and the patient was fully satisfied with the cosmetic and functional results. Discussion and Conclusions: Resection of facial congenital melanocytic nevi, followed by single-stage reconstruction using Matriderm and skin graft from the scalp, is an excellent and fast reconstructive method with promising aesthetic outcomes and greater improvement in physiological outcome, especially in the pediatric population.
Keywords: dermal; face; graft; matrix; nevus.
Figures

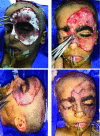

Similar articles
-
Reconstruction of Back Defect from Giant Congenital Melanocytic Nevus Using Dermal Substitute Matrix.Plast Reconstr Surg Glob Open. 2025 Jan 21;13(1):e6487. doi: 10.1097/GOX.0000000000006487. eCollection 2025 Jan. Plast Reconstr Surg Glob Open. 2025. PMID: 39839454 Free PMC article.
-
The Use of Matriderm® for Scalp Full-Thickness Defects Reconstruction: A Case Series.J Clin Med. 2022 Oct 13;11(20):6041. doi: 10.3390/jcm11206041. J Clin Med. 2022. PMID: 36294362 Free PMC article.
-
Radical resection of giant congenital melanocytic nevus and reconstruction with meek-graft covered integra dermal template.Dermatol Surg. 2003 Jun;29(6):653-7. doi: 10.1046/j.1524-4725.2003.29157.x. Dermatol Surg. 2003. PMID: 12786713
-
Giant Congenital Blue Nevus Presenting as Cutis Verticis Gyrata: A Case Report and Review of the Literature.Ann Otol Rhinol Laryngol. 2021 Dec;130(12):1407-1411. doi: 10.1177/00034894211007236. Epub 2021 Apr 3. Ann Otol Rhinol Laryngol. 2021. PMID: 33813872 Review.
-
Role of In Vivo Reflectance Confocal Microscopy in the Analysis of Melanocytic Lesions.Acta Dermatovenerol Croat. 2018 Apr;26(1):64-67. Acta Dermatovenerol Croat. 2018. PMID: 29782304 Review.
Cited by
-
Use of Preexpanded Forehead and Neck Skin in Case of Giant Facial Hairy Naevus: Planning and Technique.Indian J Plast Surg. 2021 Apr;54(2):221-224. doi: 10.1055/s-0040-1721537. Epub 2020 Nov 30. Indian J Plast Surg. 2021. PMID: 34239250 Free PMC article.
-
Serial Tissue Expansion and Skin Grafts in the Management of a Giant Congenital Nevus of the Face: Review of Literature and Case Report.Arch Plast Surg. 2024 Feb 29;51(3):290-294. doi: 10.1055/a-2201-8061. eCollection 2024 May. Arch Plast Surg. 2024. PMID: 38737851 Free PMC article.
References
-
- Bittencourt FV, Marghoob AA, Kopf AW, Koenig KL, Bart RS. Large congenital melanocytic nevi and the risk for development of malignant melanoma and neurocutaneous melanocytosis. Pediatrics. 2000;106:736–41. - PubMed
-
- Corcoran J, Bauer BS. Management of large melanocytic nevi in the extremities. J Craniofac Surg. 2005;16:877–85. - PubMed
-
- Berg P, Lindelof B. Congenital melanocytic naevi and cutaneous melanoma. Melanoma Res. 2003;13:441–5. - PubMed
-
- Castilla EE, da Graca Dutra M, Orioli-Parreiras IM. Epidemiology of congenital pigmented naevi, part I: incidence rates and relative frequencies. Br J Dermatol. 1981;104:307–15. - PubMed
-
- Kincannon J, Boutzale C. The physiology of pigmented nevi. Pediatrics. 1999;104:1042–5. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
