Radiomics in Kidney Cancer: MR Imaging
- PMID: 30466904
- PMCID: PMC6554741
- DOI: 10.1016/j.mric.2018.08.005
Radiomics in Kidney Cancer: MR Imaging
Abstract
Renal tumors encompass a heterogeneous disease spectrum, which confounds patient management and treatment. Percutaneous biopsy is limited by an inability to sample every part of the tumor. Radiomics may provide detail beyond what can be achieved from human interpretation. Understanding what new technologies offer will allow radiologists to play a greater role in caring for patients with renal cell carcinoma. In this article, we review the use of radiomics in renal cell carcinoma, in both the pretreatment assessment of renal masses and posttreatment evaluation of renal cell carcinoma, with special emphasis on the use of multiparametric MR imaging datasets.
Keywords: Kidney cancer; MR imaging; Quantitative imaging; Radiomics.
Copyright © 2018 Elsevier Inc. All rights reserved.
Figures





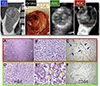



Similar articles
-
Radiomics and Artificial Intelligence for Renal Mass Characterization.Radiol Clin North Am. 2020 Sep;58(5):995-1008. doi: 10.1016/j.rcl.2020.06.001. Epub 2020 Jul 16. Radiol Clin North Am. 2020. PMID: 32792129 Review.
-
Cross-Sectional Imaging of Renal Masses: Image Interpretation-Related Potential Pitfalls and Possible Solutions.Semin Roentgenol. 2016 Jan;51(1):40-8. doi: 10.1053/j.ro.2016.01.002. Epub 2016 Jan 23. Semin Roentgenol. 2016. PMID: 27020235 Review. No abstract available.
-
Multiparametric Magnetic Resonance Imaging of Solid Renal Tumors: A Practical Algorithm.Semin Ultrasound CT MR. 2017 Feb;38(1):47-58. doi: 10.1053/j.sult.2016.08.009. Epub 2016 Sep 1. Semin Ultrasound CT MR. 2017. PMID: 28237280 Review.
-
Differentiation of Solid Renal Tumors with Multiparametric MR Imaging.Radiographics. 2017 Nov-Dec;37(7):2026-2042. doi: 10.1148/rg.2017170039. Radiographics. 2017. PMID: 29131770 Review.
-
Imaging and Screening of Kidney Cancer.Radiol Clin North Am. 2017 Nov;55(6):1235-1250. doi: 10.1016/j.rcl.2017.06.007. Radiol Clin North Am. 2017. PMID: 28991563 Free PMC article. Review.
Cited by
-
Preoperative Differentiation of Uterine Sarcoma from Leiomyoma: Comparison of Three Models Based on Different Segmentation Volumes Using Radiomics.Mol Imaging Biol. 2019 Dec;21(6):1157-1164. doi: 10.1007/s11307-019-01332-7. Mol Imaging Biol. 2019. PMID: 30850967
-
The influence of manual segmentation strategies and different phases selection on machine learning-based computed tomography in renal tumors: a systematic review and meta-analysis.Radiol Med. 2024 Jul;129(7):1025-1037. doi: 10.1007/s11547-024-01825-8. Epub 2024 May 13. Radiol Med. 2024. PMID: 38740709
-
A Computed Tomography-Based Radiomics Nomogram to Preoperatively Predict Tumor Necrosis in Patients With Clear Cell Renal Cell Carcinoma.Front Oncol. 2020 May 29;10:592. doi: 10.3389/fonc.2020.00592. eCollection 2020. Front Oncol. 2020. PMID: 32547934 Free PMC article.
-
Development of the interpretable typing prediction model for osteosarcoma and chondrosarcoma based on machine learning and radiomics: a multicenter retrospective study.Front Med (Lausanne). 2024 Nov 20;11:1497309. doi: 10.3389/fmed.2024.1497309. eCollection 2024. Front Med (Lausanne). 2024. PMID: 39635595 Free PMC article.
-
Contemporary Perspectives on Chronic Renal Disorders.Chronic Dis Transl Med. 2025 Apr 17;11(2):89-104. doi: 10.1002/cdt3.70004. eCollection 2025 Jun. Chronic Dis Transl Med. 2025. PMID: 40486956 Free PMC article. Review.
References
-
- Weikert S, Ljungberg B. Contemporary epidemiology of renal cell carcinoma: perspectives of primary prevention. World journal of urology. 2010;28(3):247–252. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

