Factors predicting long-term comorbidities in patients with Cushing's syndrome in remission
- PMID: 30467627
- PMCID: PMC6453862
- DOI: 10.1007/s12020-018-1819-6
Factors predicting long-term comorbidities in patients with Cushing's syndrome in remission
Erratum in
-
Correction to: Factors predicting long-term comorbidities in patients with Cushing's syndrome in remission.Endocrine. 2019 Apr;64(1):202. doi: 10.1007/s12020-019-01839-7. Endocrine. 2019. PMID: 30680542 Free PMC article.
Abstract
Purpose: In Cushing's syndrome, comorbidities often persist after remission of glucocorticoid excess. Here, we aim to identify factors predicting long-term comorbidities in patients with Cushing's syndrome in remission.
Methods: In a retrospective cross-sectional study, 118 patients with Cushing's syndrome in remission (52 pituitary, 58 adrenal, 8 ectopic) were followed for a median of 7.9 years (range 2-38) after the last surgery. Associations between baseline anthropometric, metabolic, hormonal parameters at diagnosis, and comorbidities (obesity, diabetes, hyperlipidemia, hypertension, osteoporosis, depression) at last follow-up, were tested by uni- and multivariate regression analysis.
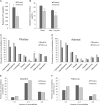
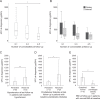
Results: In patients with manifest comorbidities at diagnosis, remission of Cushing's syndrome resolved diabetes in 56% of cases, hypertension in 36% of cases, hyperlipidaemia in 23%, and depression in 52% of cases. In a multivariate regression analysis, age, fasting glucose, BMI, and the number of comorbidities at diagnosis were positive predictors of the number of long-term comorbidities, while baseline 24-h urinary free cortisol (UFC) negatively correlated with the persistence of long-term comorbidities. The negative relationship between baseline UFC and long-term comorbidities was also found when pituitary and adrenal Cushing's cases were analyzed separately. Baseline UFC was negatively related to the time of exposure to excess glucocorticoids.
Conclusions: Long-term comorbidities after remission of Cushing's syndrome depend not only on the presence of classic cardiovascular risk factors (age, hyperglycemia, BMI), but also on the extent of glucocorticoid excess. Lower baseline UFC is associated with a higher number of long-term comorbidities, possibly due to the longer exposure to excess glucocorticoids in milder Cushing's syndrome.
Keywords: Cushing’s disease; Diabetes; Hypercortisolism; Hypertension; Obesity; Remission.
Conflict of interest statement
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human subjects were in accordance with the ethical approval standards of the institutional research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. For this type of study format, consent is not required.
Figures

References
-
- Clayton RN, Jones PW, Reulen RC, Stewart PM, Hassan-Smith ZK, Ntali G, Karavitaki N, Dekkers OM, Pereira AM, Bolland M, Holdaway I, Lindholm J. Mortality in patients with Cushing’s disease more than 10 years after remission: a multicentre, multinational, retrospective cohort study. Lancet Diabetes Endocrinol. 2016;4:569–576. doi: 10.1016/S2213-8587(16)30005-5. - DOI - PubMed
-
- E. Valassi, A. Santos, M. Yaneva, M. Toth, C.J. Strasburger, P. Chanson, J.A. Wass, O. Chabre, M. Pfeifer, R.A. Feelders, S. Tsagarakis, P.J. Trainer, H. Franz, K. Zopf, S. Zacharieva, S.W. Lamberts, A. Tabarin, S.M. Webb, ERCUSYN Study Group, The European Registry on Cushing's syndrome: 2-year experience. Baseline demographic and clinical characteristics. Eur. J. Endocrinol 165, 383–392 (2011) - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

