Lost but not forgotten: A population-based study of mortality and care trajectories among people living with HIV who are lost to follow-up in Ontario, Canada
- PMID: 30474908
- PMCID: PMC9292000
- DOI: 10.1111/hiv.12682
Lost but not forgotten: A population-based study of mortality and care trajectories among people living with HIV who are lost to follow-up in Ontario, Canada
Abstract
Objectives: Selection as a consequence of volunteer participation in, and loss to follow-up from, cohort studies may bias estimates of mortality and other health outcomes. To quantify this potential, we estimated mortality and health service use among people living with HIV (PLWH) who were lost to cohort follow-up (LTCFU) from a volunteer clinical HIV-infected cohort, and compared these to mortality and health service use in active cohort participants and non-cohort-participants living with HIV in Ontario, Canada.
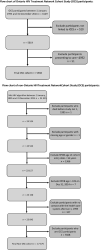
Methods: We analysed population-based provincial health databases from 1995 to 2014, identifying PLWH ≥ 18 years old; these included data from participants in the Ontario HIV Treatment Network Cohort Study (OCS), a volunteer, multi-site clinical HIV-infected cohort. We calculated all-cause mortality, hospitalization and emergency department (ED) visit rates per 100 person-years (PY) and estimated hazard ratios (HRs) of mortality, adjusting for age, sex, income, rurality, and immigration status.
Results: Among 23 043 PLWH, 5568 were OCS participants. Compared with nonparticipants, participants were younger and less likely to be female, to be an immigrant and to reside in a major urban centre, and had lower comorbidity. Mortality among active participants, participants LTCFU and nonparticipants was 2.52, 3.30 and 2.20 per 100 PY, respectively. After adjustment for covariates, mortality risk was elevated among participants LTCFU compared with active participants (HR 2.26; 95% confidence interval 1.91, 2.68). Age-adjusted hospitalization rates and ED visit rates were highest among participants LTCFU.
Conclusions: Mortality risk and use of health care resources were lower among active cohort participants. Our findings may inform health outcome estimates based on volunteer cohorts, as well as quantitative bias adjustment to correct for such biases.
Keywords: HIV; cohort; health services; lost to follow-up; mortality.
© 2018 The Authors. HIV Medicine published by John Wiley & Sons Ltd on behalf of British HIV Association.
Figures
Similar articles
-
Association of Immigrant and Refugee Status With Risk Factors for Exposure to Violent Assault Among Youths and Young Adults in Canada.JAMA Netw Open. 2020 Mar 2;3(3):e200375. doi: 10.1001/jamanetworkopen.2020.0375. JAMA Netw Open. 2020. PMID: 32129867 Free PMC article.
-
Trends in mental health service utilisation in immigrant youth in Ontario, Canada, 1996-2012: a population-based longitudinal cohort study.BMJ Open. 2018 Sep 17;8(9):e022647. doi: 10.1136/bmjopen-2018-022647. BMJ Open. 2018. PMID: 30224392 Free PMC article.
-
Cohort profile: Development and profile of a population-based, retrospective cohort of diagnosed people living with HIV in Ontario, Canada (Ontario HIV Laboratory Cohort).BMJ Open. 2019 May 27;9(5):e027325. doi: 10.1136/bmjopen-2018-027325. BMJ Open. 2019. PMID: 31133591 Free PMC article.
-
Association Between Immigrant Status and End-of-Life Care in Ontario, Canada.JAMA. 2017 Oct 17;318(15):1479-1488. doi: 10.1001/jama.2017.14418. JAMA. 2017. PMID: 28973088 Free PMC article.
-
Impact of language barriers on complications and mortality among immigrants with diabetes: a population-based cohort study.Diabetes Care. 2015 Feb;38(2):189-96. doi: 10.2337/dc14-0801. Epub 2014 Jul 15. Diabetes Care. 2015. PMID: 25028526
Cited by
-
Public attitudes towards personal health data sharing in long-term epidemiological research: a Citizen Science approach in the KORA study.BMC Public Health. 2024 Aug 26;24(1):2317. doi: 10.1186/s12889-024-19730-0. BMC Public Health. 2024. PMID: 39187842 Free PMC article.
-
Determinants of loss to care and risk of clinical progression in PLWH who are re-engaged in care after a temporary loss.Sci Rep. 2021 May 5;11(1):9632. doi: 10.1038/s41598-021-88367-5. Sci Rep. 2021. PMID: 33953250 Free PMC article.
-
Implementation of Lost & Found, An Intervention to Reengage Patients Out of HIV Care: A Convergent Explanatory Sequential Mixed-Methods Analysis.AIDS Behav. 2023 May;27(5):1531-1547. doi: 10.1007/s10461-022-03888-y. Epub 2022 Oct 22. AIDS Behav. 2023. PMID: 36271984 Free PMC article.
-
A cross-sectional study of prolonged disengagement from clinic among people with HCV receiving care in a low-threshold, multidisciplinary clinic.Can Liver J. 2020 Jun 4;3(2):212-223. doi: 10.3138/canlivj.2019-0020. eCollection 2020 Spring. Can Liver J. 2020. PMID: 35991860 Free PMC article.
References
-
- Ndiaye B, Ould‐Kaci K, Salleron J et al. Characteristics of and outcomes in HIV‐infected patients who return to care after loss to follow‐up. AIDS 2009; 23: 1786–1789. - PubMed
-
- Mocroft A, Kirk O, Aldins P et al. Loss to follow‐up in an international, multicentre observational study. HIV Med 2008; 9: 261–269. - PubMed
-
- Torian LV, Wiewel EW. Continuity of HIV‐related medical care, New York City, 2005–2009: do patients who initiate care stay in care? AIDS Patient Care STDS 2011; 25: 79–88. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical