Association of Mild to Moderate Aortic Valve Stenosis Progression With Higher Lipoprotein(a) and Oxidized Phospholipid Levels: Secondary Analysis of a Randomized Clinical Trial
- PMID: 30476957
- PMCID: PMC6583098
- DOI: 10.1001/jamacardio.2018.3798
Association of Mild to Moderate Aortic Valve Stenosis Progression With Higher Lipoprotein(a) and Oxidized Phospholipid Levels: Secondary Analysis of a Randomized Clinical Trial
Abstract
Importance: Several studies have reported an association of levels of lipoprotein(a) (Lp[a]) and the content of oxidized phospholipids on apolipoprotein B (OxPL-apoB) and apolipoprotein(a) (OxPL-apo[a]) with faster calcific aortic valve stenosis (CAVS) progression. However, whether this association is threshold or linear remains unclear.
Objective: To determine whether the plasma levels of Lp(a), OxPL-apoB, and OxPL-apo(a) have a linear association with a faster rate of CAVS progression.
Design, setting, and participants: This secondary analysis of a randomized clinical trial tested the association of baseline plasma levels of Lp(a), OxPL-apoB, and OxPL-apo(a) with the rate of CAVS progression. Participants were included from the ASTRONOMER (Effects of Rosuvastatin on Aortic Stenosis Progression) trial, a multicenter study conducted in 23 Canadian sites designed to test the effect of statin therapy (median follow-up, 3.5 years [interquartile range, 2.9-4.5 years]). Patients with mild to moderate CAVS defined by peak aortic jet velocity ranging from 2.5 to 4.0 m/s were recruited; those with peak aortic jet velocity of less than 2.5 m/s or with an indication for statin therapy were excluded. Data were collected from January 1, 2002, through December 31, 2005, and underwent ad hoc analysis from April 1 through September 1, 2018.
Interventions: After the randomization process, patients were followed up by means of echocardiography for 3 to 5 years.
Main outcomes and measures: Progression rate of CAVS as assessed by annualized progression of peak aortic jet velocity.
Results: In this cohort of 220 patients (60.0% male; mean [SD] age, 58 [13] years), a linear association was found between plasma levels of Lp(a) (odds ratio [OR] per 10-mg/dL increase, 1.10; 95% CI, 1.03-1.19; P = .006), OxPL-apoB (OR per 1-nM increase, 1.06; 95% CI, 1.01-1.12; P = .02), and OxPL-apo(a) (OR per 10-nM increase, 1.16; 95% CI, 1.05-1.27; P = .002) and faster CAVS progression, which is marked in younger patients (OR for Lp[a] level per 10-mg/dL increase, 1.19 [95% CI, 1.07-1.33; P = .002]; OR for OxPL-apoB level per 1-nM increase, 1.06 [95% CI, 1.02-1.17; P = .01]; and OR for OxPL-apo[a] level per 10-nM increase, 1.26 [95% CI, 1.10-1.45; P = .001]) and remained statistically significant after comprehensive multivariable adjustment (β coefficient, ≥ 0.25; SE, ≤ 0.004 [P ≤ .005]; OR, ≥1.10 [P ≤ .007]).
Conclusions and relevance: This study demonstrates that the association of Lp(a) levels and its content in OxPL with faster CAVS progression is linear, reinforcing the concept that Lp(a) levels should be measured in patients with mild to moderate CAVS to enhance management and risk stratification.
Trial registration: ClinicalTrials.gov Identifier: NCT00800800.
Conflict of interest statement
Figures
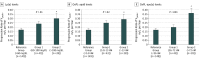
References
-
- Nishimura RA, Otto CM, Bonow RO, et al. . 2017 AHA/ACC focused update of the 2014 AHA/ACC guideline for the management of patients with valvular heart disease: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. J Am Coll Cardiol. 2017;70(2):252-289. doi:10.1016/j.jacc.2017.03.011 - DOI - PubMed
Publication types
MeSH terms
Substances
Associated data
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

