Lipid Myopathies
- PMID: 30477112
- PMCID: PMC6306737
- DOI: 10.3390/jcm7120472
Lipid Myopathies
Abstract
Disorders of lipid metabolism affect several tissues, including skeletal and cardiac muscle tissues. Lipid myopathies (LM) are rare multi-systemic diseases, which most often are due to genetic defects. Clinically, LM can have acute or chronic clinical presentation. Disease onset can occur in all ages, from early stages of life to late-adult onset, showing with a wide spectrum of clinical symptoms. Muscular involvement can be fluctuant or stable and can manifest as fatigue, exercise intolerance and muscular weakness. Muscular atrophy is rarely present. Acute muscular exacerbations, resulting in rhabdomyolysis crisis are triggered by several factors. Several classifications of lipid myopathies have been proposed, based on clinical involvement, biochemical defect or histopathological findings. Herein, we propose a full revision of all the main clinical entities of lipid metabolism disorders with a muscle involvement, also including some those disorders of fatty acid oxidation (FAO) with muscular symptoms not included among previous lipid myopathies classifications.
Keywords: FAO defect; beta-oxidation defects; lipid metabolism disorders; lipid myopathies; lipid storage disease; metabolic myopathies; muscle lipidosis.
Conflict of interest statement
The authors declare no conflict of interest.
Figures
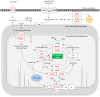

Similar articles
-
Approach to the diagnosis of metabolic myopathies.Indian J Pathol Microbiol. 2022 May;65(Supplement):S277-S290. doi: 10.4103/ijpm.ijpm_1088_21. Indian J Pathol Microbiol. 2022. PMID: 35562160 Review.
-
Metabolic Myopathies.Continuum (Minneap Minn). 2022 Dec 1;28(6):1752-1777. doi: 10.1212/CON.0000000000001182. Continuum (Minneap Minn). 2022. PMID: 36537979 Review.
-
Metabolic and mitochondrial myopathies.Neurol Clin. 2014 Aug;32(3):777-99, ix. doi: 10.1016/j.ncl.2014.05.001. Neurol Clin. 2014. PMID: 25037090 Review.
-
Metabolic myopathies: update 2009.J Clin Neuromuscul Dis. 2009 Mar;10(3):97-121. doi: 10.1097/CND.0b013e3181903126. J Clin Neuromuscul Dis. 2009. PMID: 19258857 Review.
-
Diagnosis and management of metabolic myopathies.Muscle Nerve. 2023 Sep;68(3):250-256. doi: 10.1002/mus.27840. Epub 2023 May 25. Muscle Nerve. 2023. PMID: 37226557
Cited by
-
Unmasking fibromyalgia as a mitochondrial disorder requires search for more than a single variant or single mtDNA deletions.Indian J Med Res. 2020 Oct;152(4):429-430. doi: 10.4103/ijmr.IJMR_1039_19. Indian J Med Res. 2020. PMID: 33380711 Free PMC article. No abstract available.
-
Statins Induce Locomotion and Muscular Phenotypes in Drosophila melanogaster That Are Reminiscent of Human Myopathy: Evidence for the Role of the Chloride Channel Inhibition in the Muscular Phenotypes.Cells. 2022 Nov 8;11(22):3528. doi: 10.3390/cells11223528. Cells. 2022. PMID: 36428957 Free PMC article.
-
The Association Between Acylcarnitine Metabolites and Cardiovascular Disease in Chinese Patients With Type 2 Diabetes Mellitus.Front Endocrinol (Lausanne). 2020 May 5;11:212. doi: 10.3389/fendo.2020.00212. eCollection 2020. Front Endocrinol (Lausanne). 2020. PMID: 32431666 Free PMC article.
-
Targeted Therapies for Metabolic Myopathies Related to Glycogen Storage and Lipid Metabolism: a Systematic Review and Steps Towards a 'Treatabolome'.J Neuromuscul Dis. 2021;8(3):401-417. doi: 10.3233/JND-200621. J Neuromuscul Dis. 2021. PMID: 33720849 Free PMC article.
-
ETF-QO Mutants Uncoupled Fatty Acid β-Oxidation and Mitochondrial Bioenergetics Leading to Lipid Pathology.Cells. 2019 Jan 31;8(2):106. doi: 10.3390/cells8020106. Cells. 2019. PMID: 30709034 Free PMC article.
References
Publication types
Grants and funding
LinkOut - more resources
Full Text Sources

