Mechanistic Basis for Decreased Antimicrobial Susceptibility in a Clinical Isolate of Neisseria gonorrhoeae Possessing a Mosaic-Like mtr Efflux Pump Locus
- PMID: 30482834
- PMCID: PMC6282211
- DOI: 10.1128/mBio.02281-18
Mechanistic Basis for Decreased Antimicrobial Susceptibility in a Clinical Isolate of Neisseria gonorrhoeae Possessing a Mosaic-Like mtr Efflux Pump Locus
Abstract
Recent reports suggest that mosaic-like sequences within the mtr (multiple transferable resistance) efflux pump locus of Neisseria gonorrhoeae, likely originating from commensal Neisseria sp. by transformation, can increase the ability of gonococci to resist structurally diverse antimicrobials. Thus, acquisition of numerous nucleotide changes within the mtrR gene encoding the transcriptional repressor (MtrR) of the mtrCDE efflux pump-encoding operon or overlapping promoter region for both along with those that cause amino acid changes in the MtrD transporter protein were recently reported to decrease gonococcal susceptibility to numerous antimicrobials, including azithromycin (Azi) (C. B. Wadsworth, B. J. Arnold, M. R. A. Satar, and Y. H. Grad, mBio 9:e01419-18, 2018, https://doi.org/10.1128/mBio.01419-18). We performed detailed genetic and molecular studies to define the mechanistic basis for why such strains can exhibit decreased susceptibility to MtrCDE antimicrobial substrates, including Azi. We report that a strong cis-acting transcriptional impact of a single nucleotide change within the -35 hexamer of the mtrCDE promoter as well gain-of-function amino acid changes at the C-terminal region of MtrD can mechanistically account for the decreased antimicrobial susceptibility of gonococci with a mosaic-like mtr locus.IMPORTANCE Historically, after introduction of an antibiotic for treatment of gonorrhea, strains of N. gonorrhoeae emerge that display clinical resistance due to spontaneous mutation or acquisition of resistance genes. Genetic exchange between members of the Neisseria genus occurring by transformation can cause significant changes in gonococci that impact the structure of an antibiotic target or expression of genes involved in resistance. The results presented here provide a framework for understanding how mosaic-like DNA sequences from commensal Neisseria that recombine within the gonococcal mtr efflux pump locus function to decrease bacterial susceptibility to antimicrobials, including antibiotics used in therapy of gonorrhea.
Keywords: antibiotic resistance; efflux; gonorrhea; molecular genetics; transformation.
Figures
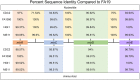





Comment in
-
Commensal Bacteria: Not Just Innocent Bystanders.mBio. 2019 Jan 15;10(1):e02723-18. doi: 10.1128/mBio.02723-18. mBio. 2019. PMID: 30647161 Free PMC article.
References
-
- CDC. 2017. Sexually transmitted disease surveillance 2016. CDC, Atlanta, GA. https://www.cdc.gov/std/stats. Accessed 31 July 2018.
-
- Newman L, Rowley J, Vander Hoorn S, Saman Wijesooriya N, Unemo M, Low N, Stevens G, Gottlieb S, Kiarie J, Temmerman M. 2015. Global estimates of the prevalence and incidence of four curable sexually transmitted infections in 2012 based on systematic review and global reporting. PLoS One 10:e0143304. doi: 10.1371/journal.pone.0143304. - DOI - PMC - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

