Psychiatric comorbidities in autism spectrum disorder: A comparative study between DSM-IV-TR and DSM-5 diagnosis
- PMID: 30487870
- PMCID: PMC6225088
- DOI: 10.1016/j.ijchp.2016.03.001
Psychiatric comorbidities in autism spectrum disorder: A comparative study between DSM-IV-TR and DSM-5 diagnosis
Abstract
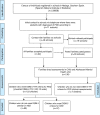
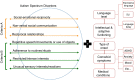
Background/Objective: The heterogeneous clinical presentations of individuals with Autism Spectrum Disorders (ASD) pose a significant challenge for sample characterization. Therefore the main goal of DSM-5 must be to identify subgroups of ASD, including comorbidity disorders and severity. The main goal of this study is to explore the psychiatric comorbidities and the severity of symptoms that could be relevant for the phenotype characterization in ASD and also to compare these results according to the different classification criteria between the DSM-IV-TR and the DSM-5. Method: A comparative study of severity and psychiatric comorbidities was carried out between a sample of participants that only met criteria for Pervasive Developmental Disorder (PDD) according to the DSM-IV-TR and a sample of participants that also met ASD criteria according to DSM-5 classification. The recruitment of children was via educational (N = 123). The psychiatric symptoms, comorbid disorders and severity of symptoms were assessed through The Nisonger Child Behavior Rating Form, clinical interview and The Inventory of Autism Spectrum Disorder, respectively. The psychiatric comorbidities considered were: anxiety, eating behavioural problems, self-aggressiveness, hetero-aggressiveness, self-harm, obsessive compulsive disorder and attention deficit and hyperactivity disorder. Results: Statistically significant differences between both groups were found regarding obsessive compulsive disorder, eating behavioural problems and severity. Conclusions: The results support the hypothesis that patients who meet the DSM-5 criteria have more severe symptoms, not only regarding the core autistic symptoms but also in relation with psychiatric comorbidities.
Antecedentes/Objetivo: Los Trastornos del Espectro Autista (TEA) incluyen un grupo heterogéneo en cuanto a su presentación clínica, que supone un desafío a nivel de caracterización diagnóstica. Por consiguiente, el objetivo principal de la clasificación DSM-5 debería de ser identificar subgrupos de TEA incluyendo severidad y comorbilidades psiquiátricas. El objetivo principal de este estudio es explorar las comorbilidades diagnósticas que pueden ser relevantes como descriptores de fenotipos autistas así como la severidad de los síntomas de autismo y comparar los resultados de las diferentes criterios de clasificación entre el DSM-IV-TR y el DSM-5. Método: Se realiza un estudio comparativo de severidad y comorbilidades psiquiátricas entre una muestra con diagnóstico de Trastorno Generalizado del Desarrollo, según criterios DSM-IV-TR, y una muestra que cumplía también criterios para TEA según la clasificación DSM-5. La muestra fue obtenida en centros educativos (N = 123). Las comorbilidades psiquiátricas y la severidad de los síntomas se evaluaron a través del The Nisonger Child Behavior Rating Form, entrevista clínica y el Inventario de Trastorno del Espectro Autista, respectivamente. Las comorbilidades estudiadas fueron ansiedad, alteraciones de la conducta alimentaria, auto-agresividad, hetero-agresividad, autolesiones, trastorno obsesivo-compulsivo y déficit de atención e hiperactividad. Resultados: Se encontraron diferencias estadísticamente significativas entre ambos grupos para trastorno obsesivo-compulsivo, alteraciones de la conducta alimentaria y severidad. Conclusiones: Se apoya la hipótesis de que los individuos que cumplen criterios diagnósticos según DSM-5 tienen mayor severidad sintomática, no sólo con respecto a los síntomas autistas centrales, sino también en relación con comorbilidades psiquiátricas.
Keywords: Autism spectrum disorder; DSM-5; DSM-IV-TR; Descriptive study; Psychiatric-comorbidities.
Figures
Similar articles
-
DSM-5 criteria for autism spectrum disorder maximizes diagnostic sensitivity and specificity in preschool children.Soc Psychiatry Psychiatr Epidemiol. 2019 Jun;54(6):693-701. doi: 10.1007/s00127-019-01674-1. Epub 2019 Mar 8. Soc Psychiatry Psychiatr Epidemiol. 2019. PMID: 30850887 Free PMC article.
-
A Comparison of DSM-IV-TR and DSM-5 Diagnostic Classifications in the Clinical Diagnosis of Autistic Spectrum Disorder.J Autism Dev Disord. 2017 Jan;47(1):101-109. doi: 10.1007/s10803-016-2937-8. J Autism Dev Disord. 2017. PMID: 27747464
-
A comparison of DSM-IV pervasive developmental disorder and DSM-5 autism spectrum disorder prevalence in an epidemiologic sample.J Am Acad Child Adolesc Psychiatry. 2014 May;53(5):500-8. doi: 10.1016/j.jaac.2013.12.021. Epub 2014 Jan 21. J Am Acad Child Adolesc Psychiatry. 2014. PMID: 24745950 Free PMC article.
-
[Treatment-refractory OCD from the viewpoint of obsessive-compulsive spectrum disorders: impact of comorbid child and adolescent psychiatric disorders].Seishin Shinkeigaku Zasshi. 2013;115(9):990-6. Seishin Shinkeigaku Zasshi. 2013. PMID: 24228477 Review. Japanese.
-
[Attention-deficit / hyperactivity disorder in autism spectrum disorders].Invest Clin. 2011 Jun;52(2):195-204. Invest Clin. 2011. PMID: 21866791 Review. Spanish.
Cited by
-
Prevalence of Autism Spectrum Disorder and Co-morbidities in Children and Adolescents: A Systematic Literature Review.Front Psychiatry. 2021 Oct 27;12:744709. doi: 10.3389/fpsyt.2021.744709. eCollection 2021. Front Psychiatry. 2021. PMID: 34777048 Free PMC article.
-
Sex-specific relationships of the infant microbiome and early-childhood behavioral outcomes.Pediatr Res. 2022 Aug;92(2):580-591. doi: 10.1038/s41390-021-01785-z. Epub 2021 Nov 4. Pediatr Res. 2022. PMID: 34732816 Free PMC article.
-
Diet-induced dysbiosis of the maternal gut microbiome in early life programming of neurodevelopmental disorders.Neurosci Res. 2021 Jul;168:3-19. doi: 10.1016/j.neures.2021.05.003. Epub 2021 May 13. Neurosci Res. 2021. PMID: 33992660 Free PMC article. Review.
-
Functional Neurological Disorder and Autism Spectrum Disorder: A Complex and Potentially Significant Relationship.Brain Behav. 2024 Dec;14(12):e70168. doi: 10.1002/brb3.70168. Brain Behav. 2024. PMID: 39705515 Free PMC article. Review.
-
Where do neurodevelopmental conditions fit in transdiagnostic psychiatric frameworks? Incorporating a new neurodevelopmental spectrum.World Psychiatry. 2024 Oct;23(3):333-357. doi: 10.1002/wps.21225. World Psychiatry. 2024. PMID: 39279404 Free PMC article.
References
-
- Aman M.G., Burrow W.H., Wolford P.L. The Aberrant Behavior Checklist-Community: Factor validity and effect of subject variables for adults in group homes. American Journal of Mental Retardation. 1995;100:283–292. - PubMed
-
- American Psychiatric Association, APA . American Psychiatric Association; Washington. DC: 2013. Diagnostic and Statistical Manual of Mental Disorders, 5th edition (DSM-5)
-
- Beighley J.S., Matson J.L., Rieske R.D., Jang J., Cervantes P.E., Goldin R.L. Comparing challenging behavior in children diagnosed with autism spectrum disorders according to the DSM-IV-TR and the proposed DSM-5. Developmental Neurorehabilitation. 2013;16:375–381. - PubMed
-
- Bejerot S. An autistic dimension: a proposed subtype of obsessive-compulsive disorder. Autism. 2007;11:101–110. - PubMed
LinkOut - more resources
Full Text Sources
Miscellaneous