Amplification of endothelium-dependent vasodilatation in contracting human skeletal muscle: role of KIR channels
- PMID: 30506579
- PMCID: PMC6395423
- DOI: 10.1113/JP276998
Amplification of endothelium-dependent vasodilatation in contracting human skeletal muscle: role of KIR channels
Abstract
Key points: In humans, the vasodilatory response to skeletal muscle contraction is mediated in part by activation of inwardly rectifying potassium (KIR ) channels. Evidence from animal models suggest that KIR channels serve as electrical amplifiers of endothelium-dependent hyperpolarization (EDH). We found that skeletal muscle contraction amplifies vasodilatation to the endothelium-dependent agonist ACh, whereas there was no change in the vasodilatory response to sodium nitroprusside, an endothelium-independent nitric oxide donor. Blockade of KIR channels reduced the exercise-induced amplification of ACh-mediated vasodilatation. Conversely, pharmacological activation of KIR channels in quiescent muscle via intra-arterial infusion of KCl independently amplified the vasodilatory response to ACh. This study is the first in humans to demonstrate that specific endothelium-dependent vasodilatory signalling is amplified in the vasculature of contracting skeletal muscle and that KIR channels may serve as amplifiers of EDH-like vasodilatory signalling in humans.
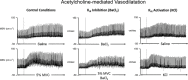
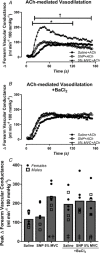
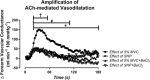
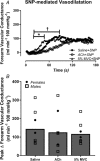
Abstract: The local vasodilatory response to muscle contraction is due in part to the activation of inwardly rectifying potassium (KIR ) channels. Evidence from animal models suggest that KIR channels function as 'amplifiers' of endothelium-dependent vasodilators. We tested the hypothesis that contracting muscle selectively amplifies endothelium-dependent vasodilatation via activation of KIR channels. We measured forearm blood flow (Doppler ultrasound) and calculated changes in vascular conductance (FVC) to local intra-arterial infusion of ACh (endothelium-dependent dilator) during resting conditions, handgrip exercise (5% maximum voluntary contraction) or sodium nitroprusside (SNP; endothelium-independent dilator) which served as a high-flow control condition (n = 7, young healthy men and women). Trials were performed before and after blockade of KIR channels via infusion of barium chloride. Exercise augmented peak ACh-mediated vasodilatation (ΔFVC saline: 117 ± 14; exercise: 236 ± 21 ml min-1 (100 mmHg)-1 ; P < 0.05), whereas SNP did not impact ACh-mediated vasodilatation. Blockade of KIR channels attenuated the exercise-induced augmentation of ACh. In eight additional subjects, SNP was administered as the experimental dilator. In contrast to ACh, exercise did not alter SNP-mediated vasodilatation (ΔFVC saline: 158 ± 35; exercise: 121 ± 22 ml min-1 (100 mmHg)-1 ; n.s.). Finally, in a subset of six subjects, direct pharmacological activation of KIR channels in quiescent muscle via infusion of KCl amplified peak ACh-mediated vasodilatation (ΔFVC saline: 97 ± 15, KCl: 142 ± 16 ml min-1 (100 mmHg)-1 ; respectively; P < 0.05). These findings indicate that skeletal muscle contractions selectively amplify endothelium-dependent vasodilatory signalling via activation of KIR channels, and this may be an important mechanism contributing to the normal vasodilatory response to exercise in humans.
Keywords: Inwardly rectifying potassium channels; endothelium-dependent hyperpolarization; exercise hyperaemia.
© 2018 The Authors. The Journal of Physiology © 2018 The Physiological Society.
Figures



Comment in
-
Electrical amplification: KIR channels taking centre stage in the hyperaemic debate.J Physiol. 2019 Mar;597(5):1223-1224. doi: 10.1113/JP277513. Epub 2019 Jan 28. J Physiol. 2019. PMID: 30615195 Free PMC article. No abstract available.
Similar articles
-
Endothelium-dependent vasodilatory signalling modulates α1 -adrenergic vasoconstriction in contracting skeletal muscle of humans.J Physiol. 2016 Dec 15;594(24):7435-7453. doi: 10.1113/JP272829. Epub 2016 Oct 13. J Physiol. 2016. PMID: 27561916 Free PMC article.
-
Contracting human skeletal muscle maintains the ability to blunt α1 -adrenergic vasoconstriction during KIR channel and Na(+) /K(+) -ATPase inhibition.J Physiol. 2015 Jun 15;593(12):2735-51. doi: 10.1113/JP270461. Epub 2015 May 20. J Physiol. 2015. PMID: 25893955 Free PMC article. Clinical Trial.
-
KIR channel activation links local vasodilatation with muscle fibre recruitment during exercise in humans.J Physiol. 2020 Jul;598(13):2621-2636. doi: 10.1113/JP279682. Epub 2020 May 17. J Physiol. 2020. PMID: 32329892 Free PMC article.
-
Endothelial-smooth muscle cell interactions in the regulation of vascular tone in skeletal muscle.Microcirculation. 2016 Nov;23(8):626-630. doi: 10.1111/micc.12322. Microcirculation. 2016. PMID: 27653241 Review.
-
Vascular inward rectifier K+ channels as external K+ sensors in the control of cerebral blood flow.Microcirculation. 2015 Apr;22(3):183-96. doi: 10.1111/micc.12190. Microcirculation. 2015. PMID: 25641345 Free PMC article. Review.
Cited by
-
Visceral adipose of obese mice inhibits endothelial inwardly rectifying K+ channels in a CD36-dependent fashion.Am J Physiol Cell Physiol. 2024 May 1;326(5):C1543-C1555. doi: 10.1152/ajpcell.00073.2024. Epub 2024 Apr 8. Am J Physiol Cell Physiol. 2024. PMID: 38586877 Free PMC article.
-
Integrating molecular and cellular components of endothelial shear stress mechanotransduction.Am J Physiol Heart Circ Physiol. 2024 Oct 1;327(4):H989-H1003. doi: 10.1152/ajpheart.00431.2024. Epub 2024 Aug 23. Am J Physiol Heart Circ Physiol. 2024. PMID: 39178024 Review.
-
In utero hypoxia attenuated acetylcholine-mediated vasodilatation via CHRM3/p-NOS3 in fetal sheep MCA: role of ROS/ERK1/2.Hypertens Res. 2022 Jul;45(7):1168-1182. doi: 10.1038/s41440-022-00935-y. Epub 2022 May 18. Hypertens Res. 2022. PMID: 35585170
-
Endogenous muscarinic acetylcholine receptor signaling blunts α1-adrenergic vasoconstriction during higher-intensity handgrip exercise in humans.Am J Physiol Regul Integr Comp Physiol. 2025 Jun 1;328(6):R619-R627. doi: 10.1152/ajpregu.00305.2024. Epub 2025 Apr 16. Am J Physiol Regul Integr Comp Physiol. 2025. PMID: 40235317 Free PMC article.
-
ATP and acetylcholine interact to modulate vascular tone and α1-adrenergic vasoconstriction in humans.J Appl Physiol (1985). 2021 Aug 1;131(2):566-574. doi: 10.1152/japplphysiol.00205.2021. Epub 2021 Jun 24. J Appl Physiol (1985). 2021. PMID: 34166116 Free PMC article.
References
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Miscellaneous

