Biological mesh is a safe and effective method of abdominal wall reconstruction in cytoreductive surgery for peritoneal malignancy
- PMID: 30511047
- PMCID: PMC6254008
- DOI: 10.1002/bjs5.93
Biological mesh is a safe and effective method of abdominal wall reconstruction in cytoreductive surgery for peritoneal malignancy
Abstract
Background: Patients with peritoneal malignancy often have multiple laparotomies before referral for cytoreductive surgery (CRS). Some have substantial abdominal wall herniation and tumour infiltration of abdominal incisions. CRS involves complete macroscopic tumour removal and hyperthermic intraperitoneal chemotherapy (HIPEC). Abdominal wall reconstruction is problematic in these patients. The aim of this study was to establish immediate and long-term outcomes of abdominal wall reconstruction with biological mesh in a single centre.
Methods: A dedicated peritoneal malignancy database was searched for all patients who had biological mesh abdominal wall reconstruction between 2004 and 2015. Short- and long-term outcomes were reviewed. All patients had annual abdominal CT as routine peritoneal malignancy follow-up.
Results: Some 33 patients (22 women) with a mean age of 53·4 (range 19-82) years underwent abdominal wall reconstruction with biological mesh. The majority (23) had CRS for pseudomyxoma (19 low grade), six for colorectal peritoneal metastasis and four for appendiceal adenocarcinoma; 18 had undergone CRS and HIPEC previously. Twenty-five of the 33 patients had abdominal wall tumour involvement and eight had concurrent hernias. The mean duration of surgery was 486 (range 120-795) min and the mean mesh size used was 345 (50-654) cm2. Ten patients developed wound infections and four had a seroma. Two developed early enterocutaneous fistulas. Mean follow-up was 48 months. Five patients developed an incisional hernia. Four died from progressive malignancy. A further 15 patients had disease recurrence, but only one had isolated abdominal wall recurrence.
Conclusion: Biological mesh was safe and effective for abdominal wall reconstruction in peritoneal malignancy. Postoperative wound infections were frequent but nevertheless incisional hernia rates were low with no instances of mesh-related bowel erosion or fistulation.
Figures

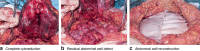

References
-
- Moran BJ, Cecil TD. Treatment of surgically resectable colorectal peritoneal metastases. Br J Surg 2014; 101: 5–7. - PubMed
-
- Elias D, Goéré D, Dumont F, Honoré C, Dartigues P, Stoclin A et al Role of hyperthermic intraoperative peritoneal chemotherapy in the management of peritoneal metastases. Eur J Cancer 2014; 50: 332–340. - PubMed
-
- Youssef H, Newman C, Chandrakumaran K, Mohamed F, Cecil TD, Moran BJ. Operative findings, early complications, and long‐term survival in 456 patients with pseudomyxoma peritonei syndrome of appendiceal origin. Dis Colon Rectum 2011; 54: 293–299. - PubMed
-
- Moran B, Baratti D, Yan TD, Kusamura S, Deraco M. Consensus statement on the loco‐regional treatment of appendiceal mucinous neoplasms with peritoneal dissemination (pseudomyxoma peritonei). J Surg Oncol 2008; 98: 277–282. - PubMed
LinkOut - more resources
Full Text Sources
Medical

