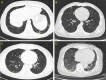
Pulmonary high-resolution computed tomography findings in patients with synovitis, acne, pustulosis, hyperostosis and osteitis syndrome
- PMID: 30517110
- PMCID: PMC6281176
- DOI: 10.1371/journal.pone.0206858
Pulmonary high-resolution computed tomography findings in patients with synovitis, acne, pustulosis, hyperostosis and osteitis syndrome
Abstract
Objective: To characterize the high-resolution computed tomography (HRCT) pulmonary abnormalities in patients with synovitis, acne, pustulosis, hyperostosis, and osteitis (SAPHO) syndrome.
Methods: Pulmonary HRCT images were reconstructed from whole-spine computed tomography (CT) images of 67 patients with SAPHO syndrome. HRCT images of 58 healthy controls were also obtained and reviewed. Patients with pneumonia and tuberculosis were excluded. Demographic and clinical data such as gender, age, onset age, disease duration, erythrocyte sedimentation rate (ESR), highly sensitive C-reactive protein (hs-CRP) and the Bath Ankylosing Spondylitis Disease Activity Index (BASDAI) were collected from the SAPHO syndrome patients. Demographic characteristics, ESR and hs-CRP data from the healthy controls were also recorded. Student's t test, Mann-Whitney U test, chi-squared test and logistic regression were employed to compare the HRCT findings of the two groups of patients.
Results: The median age of the SAPHO syndrome patients was 47.0 years, interquartile range [38.0-53.0]; that of the healthy controls was 37.0[30.8-53.8]. From the detailed HRCT evaluations, abnormalities were identified in 45 patients. We found irregular linear opacities in 29 (43.3%) patients, opacities in 22 (32.8%), ground-glass opacity in 11 (16.4%), pleural thickening in 9 (13.4%), solitary nodules in 6 (9%), bronchiectasis in 3 (4.5%), pulmonary bulla in 2 (3%), multiple nodules in 1 (1.5%), and reticular patterns in 1 (1.5%). Compared to the healthy controls, the SAPHO syndrome patients had a significantly higher rate of opacities but a significantly lower percentage of nodules (especially multiple nodules), although the overall rates of abnormal HRCT findings were similar in the two groups. According to the multivariate logistic regression analysis, increased age and BASDAI < 4 were significant predictors of abnormal HRCT findings.
Conclusion: Our study is the first to address HRCT pulmonary abnormalities in SAPHO syndrome patients. SAPHO syndrome patients have a significantly higher percentage of opacities and a significantly lower rate of pulmonary nodules than healthy controls. BASDAI and age are possible good predictors of abnormal HRCT pulmonary findings.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures
Similar articles
-
Fibromyalgia in patients with synovitis, acne, pustulosis, hyperostosis, and osteitis (SAPHO) syndrome: prevalence and screening.Clin Rheumatol. 2021 Apr;40(4):1559-1565. doi: 10.1007/s10067-020-05394-9. Epub 2020 Sep 19. Clin Rheumatol. 2021. PMID: 32949312
-
A retrospective study of bone scintigraphy in the follow-up of patients with synovitis, acne, pustulosis, hyperostosis, and osteitis syndrome: is it useful to repeat bone scintigraphy for disease assessment?Clin Rheumatol. 2020 Apr;39(4):1305-1314. doi: 10.1007/s10067-019-04864-z. Epub 2019 Dec 19. Clin Rheumatol. 2020. PMID: 31858336
-
Synovitis, acne, pustulosis, hyperostosis and osteitis syndrome: a single centre study of a cohort of 164 patients.Rheumatology (Oxford). 2016 Jun;55(6):1023-30. doi: 10.1093/rheumatology/kew015. Epub 2016 Feb 25. Rheumatology (Oxford). 2016. PMID: 26917545
-
Imaging for Synovitis, Acne, Pustulosis, Hyperostosis, and Osteitis (SAPHO) Syndrome.Rheum Dis Clin North Am. 2016 Nov;42(4):695-710. doi: 10.1016/j.rdc.2016.07.011. Rheum Dis Clin North Am. 2016. PMID: 27742022 Review.
-
The SAPHO syndrome in children: a rare cause of hyperostosis and osteitis.J Pediatr Orthop. 1999 May-Jun;19(3):297-300. J Pediatr Orthop. 1999. PMID: 10344310 Review.
Cited by
-
Synovitis, acne, pustulosis, hyperostosis, and osteitis syndrome: review and update.Ther Adv Musculoskelet Dis. 2020 May 12;12:1759720X20912865. doi: 10.1177/1759720X20912865. eCollection 2020. Ther Adv Musculoskelet Dis. 2020. PMID: 32523634 Free PMC article. Review.
-
What Is New and What Is Next for SAPHO Syndrome Management: A Narrative Review.J Clin Med. 2025 Feb 18;14(4):1366. doi: 10.3390/jcm14041366. J Clin Med. 2025. PMID: 40004896 Free PMC article. Review.
-
[SAPHO syndrome : An overview and nosological differentiation of 35 disease cases].Z Rheumatol. 2021 Jun;80(5):456-466. doi: 10.1007/s00393-021-00979-4. Epub 2021 Mar 16. Z Rheumatol. 2021. PMID: 33725179 Free PMC article. German.
References
-
- Chamot AM, Benhamou CL, Kahn MF, Beraneck L, Kaplan G, Prost A. Acne-pustulosis-hyperostosis-osteitis syndrome. Results of a national survey. 85 cases. Revue du rhumatisme et des maladies osteo-articulaires. 1987;54(3):187–96. Epub 1987/03/01. . - PubMed
-
- Earwaker JW, Cotten A. SAPHO: syndrome or concept? Imaging findings. Skeletal radiology. 2003;32(6):311–27. Epub 2003/04/30. 10.1007/s00256-003-0629-x . - DOI - PubMed
-
- Colina M, Govoni M, Orzincolo C, Trotta F. Clinical and radiologic evolution of synovitis, acne, pustulosis, hyperostosis, and osteitis syndrome: a single center study of a cohort of 71 subjects. Arthritis Rheum. 2009;61(6):813–21. Epub 2009/05/30. 10.1002/art.24540 . - DOI - PubMed
-
- Nguyen MT, Borchers A, Selmi C, Naguwa SM, Cheema G, Gershwin ME. The SAPHO syndrome. Seminars in arthritis and rheumatism. 2012;42(3):254–65. Epub 2012/11/17. 10.1016/j.semarthrit.2012.05.006 . - DOI - PubMed
-
- Li C, Cao Y, Zhang W. Clinical heterogeneity of SAPHO syndrome: Challenge of diagnosis. Mod Rheumatol. 2018:1–3. Epub 2017/12/19. 10.1080/14397595.2017.1416733 . - DOI - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous