Preventing Peritoneal Dialysis-Associated Fibrosis by Therapeutic Blunting of Peritoneal Toll-Like Receptor Activity
- PMID: 30538643
- PMCID: PMC6277495
- DOI: 10.3389/fphys.2018.01692
Preventing Peritoneal Dialysis-Associated Fibrosis by Therapeutic Blunting of Peritoneal Toll-Like Receptor Activity
Abstract
Peritoneal dialysis (PD) is an essential daily life-saving treatment for end-stage renal failure. PD therapy is limited by peritoneal inflammation, which leads to peritoneal membrane failure as a result of progressive fibrosis. Peritoneal infections, with the concomitant acute inflammatory response and membrane fibrosis development, worsen PD patient outcomes. Patients who remain infection-free, however, also show evidence of inflammation-induced membrane damage and fibrosis, leading to PD cessation. In this case, uraemia, prolonged exposure to bio-incompatible PD solutions and surgical catheter insertion have been reported to induce sterile peritoneal inflammation and fibrosis as a result of cellular stress or tissue injury. Attempts to reduce inflammation (either infection-induced or sterile) and, thus, minimize fibrosis development in PD have been hampered because the immunological mechanisms underlying this PD-associated pathology remain to be fully defined. Toll-like receptors (TLRs) are central to mediating inflammatory responses by recognizing a wide variety of microorganisms and endogenous components released following cellular stress or generated as a consequence of extracellular matrix degradation during tissue injury. Given the close link between inflammation and fibrosis, recent investigations have evaluated the role that TLRs play in infection-induced and sterile peritoneal fibrosis development during PD. Here, we review the findings and discuss the potential of reducing peritoneal TLR activity by using a TLR inhibitor, soluble TLR2, as a therapeutic strategy to prevent PD-associated peritoneal fibrosis.
Keywords: inflammation; peritoneal dialysis; peritoneal fibrosis; soluble toll-like receptor 2; toll-like receptors.
Figures
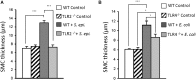

References
-
- Catalan M. P., Esteban J., Subira D., Egido J., Ortiz A. Grupo De Estudios Peritoneales De Madrid Friat/Irsin (2003). Inhibition of caspases improves bacterial clearance in experimental peritonitis. Perit. Dial. Int. 23 123–126. - PubMed
Publication types
LinkOut - more resources
Full Text Sources

