Prevalence of curable and pseudoarthrosis stages of adolescent lumbar spondylolysis
- PMID: 30546798
- PMCID: PMC6288723
- DOI: 10.2185/jrm.2967
Prevalence of curable and pseudoarthrosis stages of adolescent lumbar spondylolysis
Abstract
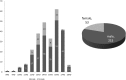
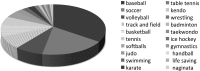
Objective: The aim of this study was to determine the prevalence of curable and pseudoarthrosis stages of adolescent lumbar spondylolysis under high school students complaining of and seeking medical consultation for low back pain. Patients and Methods: We analyzed age, sex, morbidity, presence of spina bifida occulta (SBO), and competitive sport discipline of patients with lumbar spondylolysis. We then stratified their pathological stage using a modified classification system via magnetic resonance imaging and computed tomography. Results: Of 507 patients, 451 lesions in 268 patients were diagnosed with lumbar spondylolysis (average age, 14.7 years; sex ratio, 215:53 male/female). Morbidity levels were as follows: L1, 1 lesion in 1 patient; L2, 9 lesions in 5 patients; L3, 38 lesions in 25 patients; L4, 106 lesions in 74 patients; L5, 297 lesions in 189 patients, and SBO verified in 111 patients. A total of 264 patients played a specific sport: baseball, 93; soccer, 49; volleyball, 21; track and field, 21; basketball, 20; others, 164. The prevalence of curable- and pseudoarthrosis-stage lumbar spondylolysis was 206 lesions in 142 patients, and 141 lesions in 87 patients, respectively. Conclusion: With 59.3% of patients having curable-stage lumbar spondylolysis, adolescent athletes with low back pain are urged to seek consultation. Furthermore, clinicians should perform magnetic resonance imaging to avoid misdiagnosis.
Keywords: adolescent; lumbar spondylolysis; pseudoarthrosis; stage.
Figures





Similar articles
-
Characteristics of adolescent lumbar spondylolysis with acute unilateral fatigue fracture and contralateral pseudoarthrosis.J Rural Med. 2020 Oct;15(4):170-177. doi: 10.2185/jrm.2020-026. Epub 2020 Oct 1. J Rural Med. 2020. PMID: 33033537 Free PMC article.
-
Epidemiological differences between the sexes in adolescent patients with lumbar spondylolysis: a single-institution experience in Japan.BMC Musculoskelet Disord. 2023 Jul 8;24(1):558. doi: 10.1186/s12891-023-06679-1. BMC Musculoskelet Disord. 2023. PMID: 37422627 Free PMC article.
-
Characteristics of lumbar spondylolysis in elementary school age children.Eur Spine J. 2016 Feb;25(2):602-6. doi: 10.1007/s00586-015-4029-4. Epub 2015 May 26. Eur Spine J. 2016. PMID: 26006706
-
Double-level lumbar spondylolysis and spondylolisthesis: A retrospective study.J Orthop Surg Res. 2018 Mar 16;13(1):55. doi: 10.1186/s13018-018-0723-3. J Orthop Surg Res. 2018. PMID: 29548343 Free PMC article. Review.
-
Clinical consequences of spina bifida occulta.J Manipulative Physiol Ther. 1997 Oct;20(8):546-50. J Manipulative Physiol Ther. 1997. PMID: 9345683 Review.
Cited by
-
Growth pattern of lumbar maturity stage at L1 to L5 during adolescent growth spurt.Eur Spine J. 2023 Jun;32(6):2164-2170. doi: 10.1007/s00586-023-07686-5. Epub 2023 Apr 4. Eur Spine J. 2023. PMID: 37014437
-
Pars Interarticularis Fractures Treated with Minimally Invasive Surgery: A Literature Review.J Clin Med. 2024 Jan 19;13(2):581. doi: 10.3390/jcm13020581. J Clin Med. 2024. PMID: 38276087 Free PMC article. Review.
-
Factors associated with failure of bony union after conservative treatment of acute cases of unilateral lumbar spondylolysis.BMC Musculoskelet Disord. 2021 Jan 13;22(1):75. doi: 10.1186/s12891-020-03940-9. BMC Musculoskelet Disord. 2021. PMID: 33441118 Free PMC article.
-
Characteristics of adolescent lumbar spondylolysis with acute unilateral fatigue fracture and contralateral pseudoarthrosis.J Rural Med. 2020 Oct;15(4):170-177. doi: 10.2185/jrm.2020-026. Epub 2020 Oct 1. J Rural Med. 2020. PMID: 33033537 Free PMC article.
-
Epidemiological differences between the sexes in adolescent patients with lumbar spondylolysis: a single-institution experience in Japan.BMC Musculoskelet Disord. 2023 Jul 8;24(1):558. doi: 10.1186/s12891-023-06679-1. BMC Musculoskelet Disord. 2023. PMID: 37422627 Free PMC article.
References
-
- Oba S. Prevention of lumbar spondylolysis – for early consultation and diagnosis. Nihon Rinsho Sport Igakukaishi 2008; 16: 339–348(J Jpn Soc Clin Sports Med).
-
- Gamada H, Tatsumura M, Shibao Y. Analysis of adolescent lumbar spondylolysis cases in pre-lysis stage. J Spine Res 2018; 9: 1436–1442(in Japanese, Abstract in English).
-
- Tatsumura M, Gamada H, Imoo Y. Fusion rate of fresh injured unilateral lumbar spondylolysis with pseudoarthrosis on contralateral side. Nihon Rinsho Sport Igakukaishi 2017; 25: 367–373(J Jpn Soc Clin Sports Med).
LinkOut - more resources
Full Text Sources
