PET imaging of glucose and fatty acid metabolism for NAFLD patients
- PMID: 30547298
- PMCID: PMC8356561
- DOI: 10.1007/s12350-018-01532-8
PET imaging of glucose and fatty acid metabolism for NAFLD patients
Conflict of interest statement
The other authors have no conflict of interest.
Figures
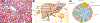


Comment on
-
Association between non-alcoholic fatty liver disease and myocardial glucose uptake measured by 18F-fluorodeoxyglucose positron emission tomography.J Nucl Cardiol. 2020 Oct;27(5):1679-1688. doi: 10.1007/s12350-018-1446-x. Epub 2018 Sep 20. J Nucl Cardiol. 2020. PMID: 30238301
References
-
- Correale M, Tarantino N, Petrucci R, Tricarico L, Laonigro I, Di Biase M, Brunetti ND. Liver disease and heart failure: Back and forth. Eur J Intern Med 2018;48:25–34. - PubMed
-
- Lee HJ, Lee CH, Kim S, Hwang SY, Hong HC, Choi HY, Chung HS, Yoo HJ, Seo JA, Kim SG, Kim NH, Baik SH, Choi DS, Choi KM. Association between vascular inflammation and non-alcoholic fatty liver disease: Analysis by 18F-fluorodeoxyglucose positron emission tomography. Metabolism 2017;67:72–79. - PubMed
-
- Mahfood Haddad T, Hamdeh S, Kanmanthareddy A, Alla VM. Nonalcoholic fatty liver disease and the risk of clinical cardiovascular events: A systematic review and meta-analysis. Diabetes Metab Syndr 2017;11Suppl 1:S209–16. - PubMed
-
- Ong JP, Pitts A, Younossi ZM. Increased overall mortality and liver-related mortality in non-alcoholic fatty liver disease. J Hepatol 2008;49:608–12. - PubMed
-
- Eslam M, Valenti L, Romeo S. Genetics and epigenetics of NAFLD and NASH: Clinical impact. J Hepatol 2018;68:268–79. - PubMed

