Multimorbidity patterns in high-need, high-cost elderly patients
- PMID: 30557384
- PMCID: PMC6296662
- DOI: 10.1371/journal.pone.0208875
Multimorbidity patterns in high-need, high-cost elderly patients
Abstract
Introduction: Patients with complex health care needs (PCHCN) are individuals who require numerous, costly care services and have been shown to place a heavy burden on health care resources. It has been argued that an important issue in providing value-based primary care concerns how to identify groups of patients with similar needs (who pose similar challenges) so that care teams and care delivery processes can be tailored to each patient subgroup. Our study aims to describe the most common chronic conditions and their combinations in a cohort of elderly PCHCN.
Methods: We focused on a cohort of PCHCN residing in an area served by a local public health unit (the "Azienda ULSS4-Veneto") and belonging to Resource Utilization Bands 4 and 5 according to the ACG System. For each patient we extracted Expanded Diagnosis Clusters, and combined them with information available from Rx-MGs diagnoses. For the present work we focused on 15 diseases/disorders, analyzing their combinations as dyads and triads. Latent class analysis was used to elucidate the patterns of the morbidities considered in the PCHCN.
Results: Five disease clusters were identified: one concerned metabolic-ischemic heart diseases; one was labelled as neurological and mental disorders; one mainly comprised cardiac diseases such as congestive heart failure and atrial fibrillation; one was largely associated with respiratory conditions; and one involved neoplasms.
Conclusions: Our study showed specific common associations between certain chronic diseases, shedding light on the patterns of multimorbidity often seen in PCHCN. Studying these patterns in more depth may help to better organize the intervention needed to deal with these patients.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures
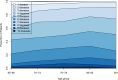
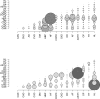
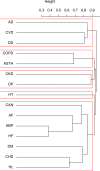
References
-
- Hayes S, Salzberg C, McCarthy D, Radley DC, Abrams MK, Shah T, et al. High-Need, High-Cost Patients: Who Are They and How Do They Use Health Care? New York, NY: The Commonwealth Fund; 3rd edPhilapelphia, PA: Wolters Kluwer 2016:3–16. - PubMed
-
- Valderas JM, Starfield B, Sibbald B, Salisbury C, Roland M. Defining comorbidity: implications for understanding health and health services. Ann Fam Med. 2009. Jul-Aug;7(4):357–63. 10.1370/afm.983 Review. - DOI - PMC - PubMed
-
- Schellevis FG. Chronic Disease in General Practice: Comorbidity and Quality of Care [dissertation] Utrecht: Drukkerij Pascal; 1993.
-
- Schäfer I, von Leitner E, Schön G, Koller D, Hansen H, Kolonko T, et al. Multimorbidity patterns in the elderly: a new approach of disease clustering identifies complex interrelations between chronic conditions. PLoS One 2010;5(12):e15941 10.1371/journal.pone.0015941 - DOI - PMC - PubMed
-
- Fortin M, Stewart M, Poitras M, Almirall J, Maddocks H. A systematic review of prevalence studies on multimorbidity: toward a more uniform methodology. Ann Fam Med 2012. Mar-Apr;10(2):142–151. 10.1370/afm.1337 - DOI - PMC - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

