Adoption of Health Information Technology Among US Nursing Facilities
- PMID: 30579920
- PMCID: PMC6591108
- DOI: 10.1016/j.jamda.2018.11.002
Adoption of Health Information Technology Among US Nursing Facilities
Abstract
Objectives: Nursing facilities have lagged behind in the adoption of interoperable health information technology (ie technologies that allow the sharing and use of electronic patient information between different information systems). The objective of this study was to estimate the nationwide prevalence of electronic health record (EHR) adoption among nursing facilities and to identify the factors associated with adoption.
Design: Cross-sectional survey.
Setting & participants: We surveyed members of the Society for Post-Acute & Long-Term Care Medicine (AMDA) about their organizations' health information technology usage and characteristics.
Measurements: Using questions adopted from existing instruments, the survey measured nursing home's EHR adoption, the ability to send, receive, search and integrate electronic information, as well as barriers to usage. Additionally, we linked survey responses to public use secondary data sources to construct measurements for 8 determinants known to be associated with organizational adoption: innovativeness, functional differentiation, role specialization, administrative intensity, professionalism, complexity, technical knowledge resources, and slack resources. A series of regression models estimated the association between potential determinants and technology adoption.
Results: 84% of nursing facilities reported using an EHR. After controlling for all other factors, respondents who characterized their organization as more innovative had more than 6 times the odds (adjusted odds ratio = 6.39, 95% confidence interval = 2.69, 15.21) of adopting an EHR. Organization innovativeness was also associated with an increased odds of being able to send, integrate, and search for electronic information. The most commonly identified barrier to sharing clinical information among nursing facilities with an EHR was a reported absence of interoperability (57%).
Conclusions/implications: An organizational culture that fosters innovation and awareness campaigns by professional societies may facilitate further adoption and effective use of technology. This will be increasingly important as policy makers continue to emphasize the use of EHRs and interoperability to improve the quality of care in nursing facilities.
Keywords: Long-term care; electronic health records; health information technology; nursing home.
Copyright © 2018 AMDA – The Society for Post-Acute and Long-Term Care Medicine. Published by Elsevier Inc. All rights reserved.
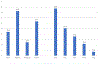
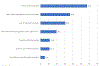
Figures
Similar articles
-
A statewide assessment of electronic health record adoption and health information exchange among nursing homes.Health Serv Res. 2014 Feb;49(1 Pt 2):361-72. doi: 10.1111/1475-6773.12137. Epub 2013 Dec 21. Health Serv Res. 2014. PMID: 24359612 Free PMC article.
-
Do service innovations influence the adoption of electronic health records in long-term care organizations? Results from the U.S. National Survey of Residential Care Facilities.Int J Med Inform. 2014 Dec;83(12):975-82. doi: 10.1016/j.ijmedinf.2014.09.007. Epub 2014 Oct 2. Int J Med Inform. 2014. PMID: 25453201
-
Adoption and utilization of electronic health record systems by long-term care facilities in Texas.Perspect Health Inf Manag. 2012;9(Spring):1g. Epub 2012 Apr 1. Perspect Health Inf Manag. 2012. PMID: 22737099 Free PMC article.
-
Factors associated with adoption of health information technology: a conceptual model based on a systematic review.JMIR Med Inform. 2014 May 23;2(1):e9. doi: 10.2196/medinform.3106. JMIR Med Inform. 2014. PMID: 25599673 Free PMC article. Review.
-
Wearable Health Technology and Electronic Health Record Integration: Scoping Review and Future Directions.JMIR Mhealth Uhealth. 2019 Sep 11;7(9):e12861. doi: 10.2196/12861. JMIR Mhealth Uhealth. 2019. PMID: 31512582 Free PMC article.
Cited by
-
Design, Development, and Evaluation of an Automated Solution for Electronic Information Exchange Between Acute and Long-term Postacute Care Facilities: Design Science Research.JMIR Form Res. 2023 Feb 17;7:e43758. doi: 10.2196/43758. JMIR Form Res. 2023. PMID: 36800213 Free PMC article.
-
Information sharing to support care transitions for patients with complex mental health and social needs.J Am Geriatr Soc. 2023 Jun;71(6):1963-1973. doi: 10.1111/jgs.18278. Epub 2023 Feb 10. J Am Geriatr Soc. 2023. PMID: 36762760 Free PMC article.
-
Written discharge communication of diagnostic and decision-making information for persons living with dementia during hospital to skilled nursing facility transitions.Geriatr Nurs. 2022 May-Jun;45:215-222. doi: 10.1016/j.gerinurse.2022.04.010. Epub 2022 May 13. Geriatr Nurs. 2022. PMID: 35569425 Free PMC article.
-
The Effect of Innovation Capabilities of Health Care Organizations on the Quality of Health Information Technology: Model Development With Cross-sectional Data.JMIR Med Inform. 2021 Mar 15;9(3):e23306. doi: 10.2196/23306. JMIR Med Inform. 2021. PMID: 33720029 Free PMC article.
-
Health Data Sharing in US Nursing Homes: A Mixed Methods Study.J Am Med Dir Assoc. 2021 May;22(5):1052-1059. doi: 10.1016/j.jamda.2020.02.009. Epub 2020 Mar 27. J Am Med Dir Assoc. 2021. PMID: 32224261 Free PMC article.
References
-
- AHIMA Longitudinal Coordination of Care Practice Council E-HIM Strategy Team. (2014). Electronic Health Record Adoption in Long Term Care ( 2014 update ). AHIMA Practice Brief, (November).
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

