Improving Handoffs Between Operating Room and Pediatric Intensive Care Teams: Before and After Study
- PMID: 30584628
- PMCID: PMC6221591
- DOI: 10.1097/pq9.0000000000000101
Improving Handoffs Between Operating Room and Pediatric Intensive Care Teams: Before and After Study
Abstract
Introduction: Patient transfer between teams and units is known to be a high-risk event for miscommunication and therefore error. We instituted a quality improvement initiative to formalize patient handoffs from the operating room (OR) to the Pediatric Intensive Care Unit (PICU). We hypothesized that measures of information transfer would improve.
Methods: In this before and after study, a multidisciplinary team developed a standardized handoff protocol (including a checklist) instituted in the Dartmouth PICU over the summer of 2016. We directly observed pediatric admissions from OR to PICU and collected data on information transfer and patient outcome metrics both before and after the institution of the handoff protocol at the time of transfer (intervention).
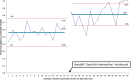
Results: We directly observed 52 handoffs (29 preintervention, 23 postintervention). The mean patient age was 9.3 years (SD, 6.5), with 55% male. Preintervention the average information transfer was 56% (upper control limit, 76%; lower control limit, 36%), whereas postintervention it was 81% (upper control limit, 97%, lower control limit, 65%). The improvement in information transfer postintervention was statistically significant (P < 0.001). There was no statistically significant change in maximum pain score in the first 6 hours after admission (preintervention, 4.5, SD 3.9; postintervention, 2.9, SD 1.3, P = 0.15). There was no difference in the time required for handoff pre- versus postintervention (8.7 minutes, SD 5.5 versus 10.1 minutes, SD 4.6, P = 0.34).
Conclusion: Standardization of OR to PICU patient transfers using a predetermined checklist at the time of handoff can improve the completeness of information transfer without increasing the length of the handoff.
Figures
Similar articles
-
Standardization of Pediatric Noncardiac Operating Room to Intensive Care Unit Handoffs Improves Communication and Patient Care.J Patient Saf. 2022 Sep 1;18(6):e1021-e1026. doi: 10.1097/PTS.0000000000000986. Epub 2022 Feb 3. J Patient Saf. 2022. PMID: 35985048
-
Handoffs and transitions in critical care (HATRICC): protocol for a mixed methods study of operating room to intensive care unit handoffs.BMC Surg. 2014 Nov 19;14:96. doi: 10.1186/1471-2482-14-96. BMC Surg. 2014. PMID: 25410548 Free PMC article. Clinical Trial.
-
A Partially Structured Postoperative Handoff Protocol Improves Communication in 2 Mixed Surgical Intensive Care Units: Findings From the Handoffs and Transitions in Critical Care (HATRICC) Prospective Cohort Study.Ann Surg. 2020 Mar;271(3):484-493. doi: 10.1097/SLA.0000000000003137. Ann Surg. 2020. PMID: 30499797
-
Improving resident handoffs for children transitioning from the intensive care unit.Hosp Pediatr. 2015 Mar;5(3):127-33. doi: 10.1542/hpeds.2014-0067. Hosp Pediatr. 2015. PMID: 25732985
-
Eastern association for the surgery of trauma - quality, patient safety, and outcomes committee - transitions of care: healthcare handoffs in trauma.Am J Surg. 2021 Sep;222(3):521-528. doi: 10.1016/j.amjsurg.2021.01.034. Epub 2021 Feb 1. Am J Surg. 2021. PMID: 33558061
Cited by
-
Qualitative Study on Safe and Effective Handover Information during a Rapid Response Team Encounter.Pediatr Qual Saf. 2023 May 22;8(3):e650. doi: 10.1097/pq9.0000000000000650. eCollection 2023 May-Jun. Pediatr Qual Saf. 2023. PMID: 38571734 Free PMC article.
-
Improved patient safety with a simplified operating room to pediatric intensive care unit handover tool (PATHQS).Front Pediatr. 2024 Jan 24;12:1327381. doi: 10.3389/fped.2024.1327381. eCollection 2024. Front Pediatr. 2024. PMID: 38328344 Free PMC article.
-
Handoff Tool Improves Transitions from the Operating Room to the Neonatal Intensive Care Unit.Pediatr Qual Saf. 2023 Oct 7;8(5):e695. doi: 10.1097/pq9.0000000000000695. eCollection 2023 Sep-Oct. Pediatr Qual Saf. 2023. PMID: 37818200 Free PMC article.
-
Handoff Mnemonics Used in Perioperative Handoff Intervention Studies: A Systematic Review.Anesth Analg. 2025 Sep 1;141(3):468-481. doi: 10.1213/ANE.0000000000007261. Epub 2024 Nov 26. Anesth Analg. 2025. PMID: 39590557 Free PMC article.
-
Screening for Social Determinants of Health in the Pediatric Intensive Care Unit: Recommendations for Clinicians.Crit Care Clin. 2023 Apr;39(2):341-355. doi: 10.1016/j.ccc.2022.09.009. Epub 2022 Nov 18. Crit Care Clin. 2023. PMID: 36898778 Free PMC article. Review.
References
-
- (IOM) IoM. To Err Is Human: Building a Safer Health System. 2000Washington, D.C.: National Academy Press. - PubMed
-
- Makary MA, Daniel M. Medical error-the third leading cause of death in the US. BMJ. 2016;353:i2139. - PubMed
-
- Donchin Y, Gopher D, Olin M, et al. A look into the nature and causes of human errors in the intensive care unit. Crit Care Med. 1995;23:294–300.. - PubMed
-
- Kemper PF, de Bruijne M, van Dyck C, et al. Crew resource management training in the intensive care unit. A multisite controlled before-after study. BMJ Qual Saf. 2016;25:577–587.. - PubMed
-
- Turkelson C, Aebersold M, Redman R, et al. Improving nursing communication skills in an intensive care unit using simulation and nursing crew resource management strategies: an implementation project. J Nurs Care Qual. 2017;32:331–339.. - PubMed
LinkOut - more resources
Full Text Sources