Negative pressure pulmonary edema postextubation following medial nerve repair with sural graft surgery in a young patient: A case report
- PMID: 30593150
- PMCID: PMC6314689
- DOI: 10.1097/MD.0000000000013743
Negative pressure pulmonary edema postextubation following medial nerve repair with sural graft surgery in a young patient: A case report
Abstract
Rationale: Negative pressure pulmonary edema (NPPE) is a serious well-described pulmonary complication. It occurs after an intense inspiratory effort against an obstructed or closed upper airway and generates a large negative airway pressure, leading to severe pulmonary edema (transvascular fluid filtration and interstitial/alveolar edema) and hypoxemia. We present a case of NPPE following general anesthesia in a patient who underwent median nerve neurorrhaphy with graft from lower left limb (sural nerve) due to sharp injury.
Patient concerns: A 39-year-old Hispanic male was admitted to the Hospital Universitario de San José and scheduled to undergo a median nerve neurorrhaphy under general anesthesia. Preoperative vital signs, physical examination, and laboratory assessments were unremarkable. At the end of surgery, anesthetic agents were ceased after patient responded to commands and maintained eye contact. However, immediately after extubation, anesthesia care providers observed marked respiratory distress and rapid development of hypoxia.
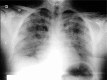
Diagnoses: After extubation, patient presented multiple episodes of hemoptysis, tachypnea (25 per minute), blood oxygen saturation (SpO2) of 82% and abundant bilateral pulmonary rales. A baseline chest x-ray revealed symmetric parenchymal opacities with ground-glass attenuation and bilateral multilobar consolidations patterns. The diagnosis of NPPE was established and supportive treatment was initiated.
Interventions: The patient received noninvasive mechanical ventilation with a PEEP at 10 cmH2O, intravenous furosemide (20 mg.) every 12 hours, and fluids restriction. Patient remained in PACU for continuing monitoring and laboratory/imaging follow-up testing until next morning.
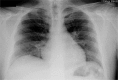
Outcomes: On postoperative day 1, patient responded satisfactorily to supportive treatment and transferred to the general care floor; oxygen supplementation was discontinued 12 hours after extubation time. On postoperative day 3, after the evaluation of a chest x-ray, patient was discharged to home in stable conditions LESSON:: The occurrence of NPPE in the perioperative setting could be successfully managed with supportive regimens, effective clinical team coordination, and awareness of the importance of its rapid diagnosis.
Conflict of interest statement
The authors have no conflicts of interest to disclose.
Figures
Similar articles
-
Negative-pressure pulmonary edema after mammoplasty: a case report.Pan Afr Med J. 2022 May 9;42:15. doi: 10.11604/pamj.2022.42.15.32010. eCollection 2022. Pan Afr Med J. 2022. PMID: 35812256 Free PMC article.
-
Recurrent negative pressure pulmonary edema.Clin Med Res. 2011 Jun;9(2):88-91. doi: 10.3121/cmr.2010.936. Epub 2010 Sep 17. Clin Med Res. 2011. PMID: 20852091 Free PMC article.
-
Negative pressure pulmonary edema after general anesthesia: A case report and literature review.Medicine (Baltimore). 2019 Apr;98(17):e15389. doi: 10.1097/MD.0000000000015389. Medicine (Baltimore). 2019. PMID: 31027133 Free PMC article. Review.
-
Negative pressure pulmonary edema after laparoscopic cholecystectomy: A case report and literature review.Medicine (Baltimore). 2024 Mar 15;103(11):e37443. doi: 10.1097/MD.0000000000037443. Medicine (Baltimore). 2024. PMID: 38489724 Free PMC article. Review.
-
Negative pressure pulmonary edema in a patient undergoing open rhinoplasty: A case report.Medicine (Baltimore). 2021 Jan 8;100(1):e24240. doi: 10.1097/MD.0000000000024240. Medicine (Baltimore). 2021. PMID: 33429827 Free PMC article.
Cited by
-
Negative pressure pulmonary edema (Review).Exp Ther Med. 2023 Aug 4;26(3):455. doi: 10.3892/etm.2023.12154. eCollection 2023 Sep. Exp Ther Med. 2023. PMID: 37614417 Free PMC article. Review.
-
Pulmonary edema: A complication of post-complete ingrown toenail excision. A case report.Saudi J Anaesth. 2024 Jan-Mar;18(1):131-133. doi: 10.4103/sja.sja_536_23. Epub 2024 Jan 2. Saudi J Anaesth. 2024. PMID: 38313710 Free PMC article.
-
Negative pressure plmonary oedema after adenotonsillectom: a case report and litrature review.Ann Med Surg (Lond). 2024 Feb 5;86(4):2236-2241. doi: 10.1097/MS9.0000000000001790. eCollection 2024 Apr. Ann Med Surg (Lond). 2024. PMID: 38576921 Free PMC article.
-
Safety, efficacy and airway complications of the flexible laryngeal mask airway in functional endoscopic sinus surgery: A retrospective study of 6661 patients.PLoS One. 2021 Feb 4;16(2):e0245521. doi: 10.1371/journal.pone.0245521. eCollection 2021. PLoS One. 2021. PMID: 33539365 Free PMC article.
References
-
- Lawrence VA, Cornell JE, Smetana GW. Strategies to reduce postoperative pulmonary complications after noncardiothoracic surgery: systematic review for the American College of Physicians. Ann Int Med 2006;144:596–608. - PubMed
-
- Canet J, Gallart L. Predicting postoperative pulmonary complications in the general population. Curr Opin Anaesthesiol 2013;26:107–15. - PubMed
-
- Abbott T, Fowler AJ, Pelosi P, et al. A systematic review and consensus definitions for standardised end-points in perioperative medicine: pulmonary complications. Br J Anaesth 2018;12:1006–79. - PubMed
-
- Belda J, Ferrando C, Garutti I. The effects of an open-lung approach during one-lung ventilation on postoperative pulmonary complications and driving pressure: a descriptive, multicenter national study. J Cardiothorac Vasc Anesth 2018;S1053-0770:30220–9. - PubMed
-
- Sabaté S, Mazo V, Canet J. Predicting postoperative pulmonary complications: implications for outcomes and costs. Curr Opin Anesthesiol 2014;27:201–9. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical