Trends in HIV care cascade engagement among diagnosed people living with HIV in Ontario, Canada: A retrospective, population-based cohort study
- PMID: 30608962
- PMCID: PMC6319701
- DOI: 10.1371/journal.pone.0210096
Trends in HIV care cascade engagement among diagnosed people living with HIV in Ontario, Canada: A retrospective, population-based cohort study
Abstract
Background: The HIV cascade is an important framework for assessing systems of care, but population-based assessment is lacking for most jurisdictions worldwide. We measured cascade indicators over time in a population-based cohort of diagnosed people living with HIV (PLWH) in Ontario, Canada.
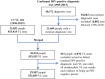
Methods: We created a retrospective cohort of diagnosed PLWH using a centralized laboratory database with HIV diagnostic and viral load (VL) test records linked at the individual-level. Individuals enter the cohort with record of a nominal HIV-positive diagnostic test or VL test, and remain unless administratively lost to follow-up (LTFU, >2 consecutive years with no VL test and no VL test in later years). We calculated the annual percent of diagnosed PLWH (cohort individuals not LTFU) between 2000 and 2015 who were in care (≥1 VL test), on ART (as documented on VL test requisition) or virally suppressed (<200 copies/ml). We also calculated time from diagnosis to linkage to care and viral suppression among individuals newly diagnosed with HIV. Analyses were stratified by sex and age. Upper/lower bounds were calculated using alternative indicator definitions.
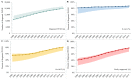
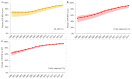
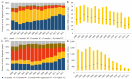
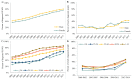
Results: The number of diagnosed PLWH increased from 8,859 (8,859-11,389) in 2000 to 16,110 (16,110-17,423) in 2015. Over this 16-year period, the percent of diagnosed PLWH who were: in care increased from 81% (63-81%) to 87% (81-87%), on ART increased from 55% (34-60%) to 81% (70-82%) and virally suppressed increased from 41% (23-46%) to 80% (67-81%). Between 2000 and 2014, the percent of newly diagnosed individuals who linked to care within three months of diagnosis or achieved viral suppression within six months of diagnosis increased from 67% to 82% and from 22% to 42%, respectively. Estimates were generally lower for females and younger individuals.
Discussion: HIV cascade indicators among diagnosed PLWH in Ontario improved between 2000 and 2015, but gaps still remain-particularly for younger individuals.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures
References
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

