Prognostic Impact of Tumor-Infiltrating Lymphocytes and Neutrophils on Survival of Patients with Upfront Resection of Pancreatic Cancer
- PMID: 30609853
- PMCID: PMC6356339
- DOI: 10.3390/cancers11010039
Prognostic Impact of Tumor-Infiltrating Lymphocytes and Neutrophils on Survival of Patients with Upfront Resection of Pancreatic Cancer
Abstract
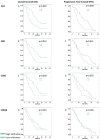
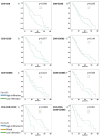
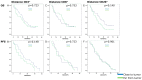
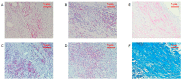
In patients with pancreatic ductal adenocarcinoma (PDAC), the tumor microenvironment consists of cellular and stromal components that influence prognosis. Hence, tumor-infiltrating lymphocytes (TILs) may predict prognosis more precisely than conventional staging systems. Studies on the impact of TILs are heterogeneous and further research is needed. Therefore, this study aims to point out the importance of peritumoral TILs, tumor-infiltrating neutrophils (TINs), and immune subtype classification in PDAC. Material from 57 patients was analyzed with immunohistochemistry performed for CD3, CD8, CD20, CD66b, α-sma, and collagen. Hot spots with peritumoral TILs and TINs were quantified according to the QTiS algorithm and the distance of TILs hot spots to the tumor front was measured. Results were correlated with overall (OS) and progression-free survival (PFS). High densities of peritumoral hot spots with CD3⁺, CD8⁺, and CD20⁺ TILs correlated significantly with improved OS and PFS. Combined immune cell subtypes predicted improved OS and PFS. High infiltration of CD3⁺ TILs predicted progression after 12 months. The location of TILs' hot spots and their distance to the tumor front did not correlate with patient survival. Peritumoral TILs and the composition of the stroma predict OS and PFS in PDAC.
Keywords: activated stroma index; immune cell infiltration; immune infiltrate; immunoscore; immunosuppression; pancreatic ductal adenocarcinoma; quantification of the tumor immune stroma (QTiS); tumor microenvironment; tumor-infiltrating lymphocytes.
Conflict of interest statement
The authors declare no conflict of interest.
Figures

References
Grants and funding
LinkOut - more resources
Full Text Sources
Research Materials

