A Multidimensional Approach to Post-concussion Symptoms in Mild Traumatic Brain Injury
- PMID: 30619066
- PMCID: PMC6306025
- DOI: 10.3389/fneur.2018.01113
A Multidimensional Approach to Post-concussion Symptoms in Mild Traumatic Brain Injury
Abstract
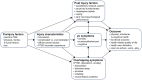
Mild traumatic brain injury (mTBI) presents a substantial burden to patients, families, and health care systems. Whereas, recovery can be expected in the majority of patients, a subset continues to report persisting somatic, cognitive, emotional, and/or behavioral problems, generally referred to as post-concussion syndrome (PCS). However, this term has been the subject of debate since the mechanisms underlying post-concussion symptoms and the role of pre- and post-injury-related factors are still poorly understood. We review current evidence and controversies concerning the use of the terms post-concussion symptoms vs. syndrome, its diagnosis, etiology, prevalence, assessment, and treatment in both adults and children. Prevalence rates of post-concussion symptoms vary between 11 and 82%, depending on diagnostic criteria, population and timing of assessment. Post-concussion symptoms are dependent on complex interactions between somatic, psychological, and social factors. Progress in understanding has been hampered by inconsistent classification and variable assessment procedures. There are substantial limitations in research to date, resulting in gaps in our understanding, leading to uncertainty regarding epidemiology, etiology, prognosis, and treatment. Future directions including the identification of potential mechanisms, new imaging techniques, comprehensive, multidisciplinary assessment and treatment options are discussed. Treatment of post-concussion symptoms is highly variable, and primarily directed at symptom relief, rather than at modifying the underlying pathology. Longitudinal studies applying standardized assessment strategies, diagnoses, and evidence-based interventions are required in adult and pediatric mTBI populations to optimize recovery and reduce the substantial socio-economic burden of post-concussion symptoms.
Keywords: diagnosis; etiology; mild traumatic brain injury; outcome; post-concussion symptoms; prevalence; treatment.
Figures

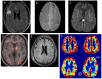
- Top row represents a single healthy control. Bottom row represents a single TBI patient.
- Left column: Cerebral Blood Flow (CBF), assessed by arterial spin labeling.
- Right column: Cerebrovascular reactivity (CVR) assessed using BOLD response to hypercapnia.
References
-
- US Department of Health and Human Services Centers CfDCaP, National Center for Health Statistics National Hospital Discharge Survey (2010-2012).
-
- American Congress of Rehabilitation Medicine (ACRM) . Definition of mild traumatic brain injury. J Head Trauma Rehabil (1993). 8:86–7. - PubMed
-
- World Health Organization The ICD-10 Classification of Mental and Behavioural Disorders: Diagnostic Criteria for Research. Geneva: WHO; (1993).
Publication types
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

