Cardiovascular Supportive Therapies for Neonates With Asphyxia - A Literature Review of Pre-clinical and Clinical Studies
- PMID: 30619782
- PMCID: PMC6295641
- DOI: 10.3389/fped.2018.00363
Cardiovascular Supportive Therapies for Neonates With Asphyxia - A Literature Review of Pre-clinical and Clinical Studies
Abstract
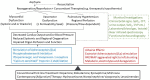
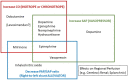
Asphyxiated neonates often have hypotension, shock, and poor tissue perfusion. Various "inotropic" medications are used to provide cardiovascular support to improve the blood pressure and to treat shock. However, there is incomplete literature on the examination of hemodynamic effects of these medications in asphyxiated neonates, especially in the realm of clinical studies (mostly in late preterm or term populations). Although the extrapolation of findings from animal studies and other clinical populations such as children and adults require caution, it seems appropriate that findings from carefully conducted pre-clinical studies are important in answering some of the fundamental knowledge gaps. Based on a literature search, this review discusses the current available information, from both clinical studies and animal models of neonatal asphyxia, on common medications used to provide hemodynamic support including dopamine, dobutamine, epinephrine, milrinone, norepinephrine, vasopressin, levosimendan, and hydrocortisone.
Keywords: asphyxia; catecholamines; hemodynamics; inotropes; newborn.
Figures
Similar articles
-
Treating Hypotension in Preterm Neonates With Vasoactive Medications.Front Pediatr. 2018 Apr 13;6:86. doi: 10.3389/fped.2018.00086. eCollection 2018. Front Pediatr. 2018. PMID: 29707527 Free PMC article. Review.
-
An Update on Pharmacologic Management of Neonatal Hypotension: When, Why, and Which Medication.Children (Basel). 2024 Apr 19;11(4):490. doi: 10.3390/children11040490. Children (Basel). 2024. PMID: 38671707 Free PMC article. Review.
-
Milrinone, dobutamine or epinephrine use in asphyxiated newborn pigs resuscitated with 100% oxygen.Intensive Care Med. 2010 Jun;36(6):1058-66. doi: 10.1007/s00134-010-1820-x. Epub 2010 Mar 11. Intensive Care Med. 2010. PMID: 20221750
-
Cardiovascular support in preterm infants.Clin Ther. 2006 Sep;28(9):1366-84. doi: 10.1016/j.clinthera.2006.09.006. Clin Ther. 2006. PMID: 17062310 Review.
-
Pharmacotherapy update on the use of vasopressors and inotropes in the intensive care unit.J Cardiovasc Pharmacol Ther. 2015 May;20(3):249-60. doi: 10.1177/1074248414559838. Epub 2014 Nov 28. J Cardiovasc Pharmacol Ther. 2015. PMID: 25432872 Review.
Cited by
-
Low Apgar score and asphyxia complications at birth and risk of longer-term cardiovascular disease: a nationwide population-based study of term infants.Lancet Reg Health Eur. 2022 Nov 3;24:100532. doi: 10.1016/j.lanepe.2022.100532. eCollection 2023 Jan. Lancet Reg Health Eur. 2022. PMID: 36643664 Free PMC article.
-
Dose-related systemic and cerebral hemodynamic effects of norepinephrine in newborn piglets with hypoxia-reoxygenation.Pediatr Res. 2025 Apr 3. doi: 10.1038/s41390-025-04010-3. Online ahead of print. Pediatr Res. 2025. PMID: 40181145
-
Management of cardiovascular dysfunction in neonates with hypoxic ischaemic encephalopathy; a national survey of current practice in the UK.J Perinatol. 2022 Dec;42(12):1695-1696. doi: 10.1038/s41372-022-01526-y. Epub 2022 Oct 6. J Perinatol. 2022. PMID: 36203082 No abstract available.
-
Getting an Early Start in Understanding Perinatal Asphyxia Impact on the Cardiovascular System.Front Pediatr. 2020 Feb 26;8:68. doi: 10.3389/fped.2020.00068. eCollection 2020. Front Pediatr. 2020. PMID: 32175294 Free PMC article. Review.
-
Comparing qualitative and quantitative echocardiographic markers to assess cardiac contractility in newborn infants: protocol for a prospective cohort study.BMJ Paediatr Open. 2024 Oct 14;8(1):e002606. doi: 10.1136/bmjpo-2024-002606. BMJ Paediatr Open. 2024. PMID: 39401972 Free PMC article.
References
-
- Perinatal morbidity. Report of the Health Care Committee Expert panel on Perinatal Morbidity. National Health and Medical Research Council. Australian Government Publishing Service; (1995)
-
- Martin-Ancel A, Garcia-Alix A, Gaya F, Cabañas F, Burgueros M, Quero J. Multiple organ involvement in perinatal asphyxia. J Pediatr. (1995) 127:786–93. - PubMed
Publication types
LinkOut - more resources
Full Text Sources

