Prevalence and determinants of anti-tuberculosis treatment non-adherence in Ethiopia: A systematic review and meta-analysis
- PMID: 30629684
- PMCID: PMC6328265
- DOI: 10.1371/journal.pone.0210422
Prevalence and determinants of anti-tuberculosis treatment non-adherence in Ethiopia: A systematic review and meta-analysis
Abstract
Background: Tuberculosis is a global public health problem. One of the overarching dilemmas and challenges facing most tuberculosis program is non-adherence to treatment. However, in Ethiopia there are few studies with variable and inconsistent findings regarding non-adherence to treatment for tuberculosis.
Methods: This systematic review and meta-analysis was conducted to determine the prevalence of non-adherence to tuberculosis treatment and its determinants in Ethiopia. Biomedical databases including PubMed, Google Scholar, Science Direct, HINARI, EMBASE and Cochrane Library were systematically and comprehensively searched. To estimate the pooled prevalence, studies reporting the prevalence of adherence or non-adherence to tuberculosis treatment and its determinants were included. Data were extracted using a standardized data extraction tool prepared in Microsoft Excel and transferred to STATA/se version-14 statistical software for further analyses. To assess heterogeneity, the Cochrane Q test statistics and I2 test were performed. Since the included studies exhibited high heterogeneity, a random effects model meta- analysis was used to estimate the pooled prevalence of non-adherence to tuberculosis treatment. Finally, the association between determinant factors and non-adherence to tuberculosis treatment was assessed.
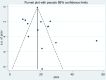
Results: The result of 13 studies revealed that the pooled prevalence of non-adherence to tuberculosis treatment in Ethiopia was found to be 21.29% (95% CI: 15.75, 26.68). In the subgroup analysis, the highest prevalence was observed in Southern Nations and Nationalities of Ethiopia, 23.61% (95% CI: 21.05, 26.17) whereas the lowest prevalence was observed in Amhara region, 10.0% (95% CI: 6.48, 13.17.0;). Forgetfulness (OR = 3.22, 95% CI = 2.28, 4.53), fear side effect of the drugs (OR = 1.93, 95% CI = 1.37, 2.74), waiting time ≥ 1 hour during service (OR = 4.88, 95% CI = 3.44, 6.91) and feeling distance to health institution is long (OR = 5.35, 95% CI = 4.00, 7.16) were found to be determinants of non-adherence to tuberculosis treatment.
Conclusion: In this meta-analysis, the pooled prevalence of non-adherence to tuberculosis treatment in Ethiopia was high. Forgetfulness, fear of side effect of the drugs, long waiting time (≥1 hour) during service and feeling distance to health institution is long were the main risk factors for non-adherence to tuberculosis treatment in Ethiopia. Early monitoring of the side effects and other reasons which account for missing medication may increase medication adherence in patients with tuberculosis in Ethiopia.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures



References
-
- Organization WH. Global tuberculosis report 2016. 2016.
-
- Dye C, Scheele S, Dolin P, Pathania V, Raviglione MC. Global burden of tuberculosis: estimated incidence, prevalence, and mortality by country. Jama. 1999;282(7):677–86. - PubMed
-
- Ahlburg DA, Initiative ST. The economic impacts of tuberculosis. 2000.
-
- Organization WH. Global tuberculosis control: epidemiology, strategy, financing: WHO report 2009: World Health Organization; 2009.
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

