Corneal re-innervation following refractive surgery treatments
- PMID: 30632489
- PMCID: PMC6352585
- DOI: 10.4103/1673-5374.247421
Corneal re-innervation following refractive surgery treatments
Abstract
Laser refractive surgery is one of the most performed surgical procedures in the world. Although regarded safe and efficient, it has side effects. All of the laser based refractive surgical procedures invoke corneal nerve injury to some degree. The impact of this denervation can range from mild discomfort to neurotrophic corneas. Currently, three techniques are widely used for laser vision correction: small incision lenticule extraction, laser-assisted keratomileusis in situ and photorefractive keratotomy. Each of these techniques affects corneal innervation differently and has a different pattern of nerve regeneration. The purpose of this review is to summarize the different underlying mechanisms for corneal nerve injury and compare the different patterns of corneal reinnervation.
Keywords: corneal nerve; corneal sensation; in vivo confocal microscopy; laser-assisted keratomileusis in situ; photorefractive keratotomy; refractive surgery; small incision manual lenticule extraction.
Conflict of interest statement
None
Figures
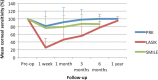
References
-
- Acosta MC, Peral A, Luna C, Pintor J, Belmonte C, Gallar J. Tear secretion induced by selective stimulation of corneal and conjunctival sensory nerve fibers. Invest Ophthalmol Vis Sci. 2004;45:2333–2336. - PubMed
-
- Agca A, Cankaya KI, Yilmaz I, Yildirim Y, Yasa D, Olcucu O, Demircan A, Demirok A, Yilmaz OF. Fellow eye comparison of nerve fiber regeneration after smile and femtosecond laser-assisted LASIK: a confocal microscopy study. J Refract Surg. 2015;31:594–598. - PubMed
-
- Al-Aqaba MA, Alomar T, Miri A, Fares U, Otri AM, Dua HS. Ex vivo confocal microscopy of human corneal nerves. Br J Ophthalmol. 2010;94:1251–1257. - PubMed
-
- Alcalde I, Inigo-Portugues A, Carreno N, Riestra AC, Merayo-Lloves JM. Effects of new biomimetic regenerating agents on corneal wound healing in an experimental model of post-surgical corneal ulcers. Arch Soc Esp Oftalmol. 2015;90:467–474. - PubMed
-
- Azar DT, Primack JD. Theoretical analysis of ablation depths and profiles in laser in situ keratomileusis for compound hyperopic and mixed astigmatism. J Cataract Refract Surg. 2000;26:1123–1136. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Medical

