Temporal Trends in the Use of Therapeutic Hypothermia for Out-of-Hospital Cardiac Arrest
- PMID: 30646357
- PMCID: PMC6324404
- DOI: 10.1001/jamanetworkopen.2018.4511
Temporal Trends in the Use of Therapeutic Hypothermia for Out-of-Hospital Cardiac Arrest
Abstract
Importance: Despite evidence that therapeutic hypothermia improves patient outcomes for out-of-hospital cardiac arrest, use of this therapy remains low.
Objective: To determine whether the use of therapeutic hypothermia and patient outcomes have changed after publication of the Targeted Temperature Management trial on December 5, 2013, which supported more lenient temperature management for out-of-hospital cardiac arrest.
Design, setting, and participants: A retrospective cohort was conducted between January 1, 2013, and December 31, 2016, of 45 935 US patients in the Cardiac Arrest Registry to Enhance Survival who experienced out-of-hospital cardiac arrest and survived to hospital admission.
Exposures: Calendar time by quarter year.
Main outcomes and measures: Use of therapeutic hypothermia and patient survival to hospital discharge.
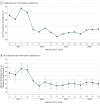
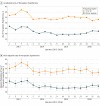
Results: Among 45 935 patients (17 515 women and 28 420 men; mean [SD] age, 59.3 [18.3] years) who experienced out-of-hospital cardiac arrest and survived to admission at 649 US hospitals, overall use of therapeutic hypothermia during the study period was 46.4%. In unadjusted analyses, the use of therapeutic hypothermia dropped from 52.5% in the last quarter of 2013 to 46.0% in the first quarter of 2014 after the December 2013 publication of the Targeted Temperature Management trial. Use of therapeutic hypothermia remained at or below 46.5% through 2016. In segmented hierarchical logistic regression analysis, the risk-adjusted odds of use of therapeutic hypothermia was 18% lower in the first quarter of 2014 compared with the last quarter of 2013 (odds ratio, 0.82; 95% CI, 0.71-0.94; P = .006). Similar point-estimate changes over time were observed in analyses stratified by presenting rhythm of ventricular tachycardia or ventricular fibrillation (odds ratio, 0.89; 95% CI, 0.71-1.13, P = .35) and pulseless electrical activity or asystole (odds ratio, 0.75; 95% CI, 0.63-0.89; P = .001). Overall risk-adjusted patient survival was 36.9% in 2013, 37.5% in 2014, 34.8% in 2015, and 34.3% in 2016 (P < .001 for trend). In mediation analysis, temporal trends in use of hypothermia did not consistently explain trends in patient survival.
Conclusions and relevance: In a US registry of patients who experienced out-of-hospital cardiac arrest, the use of guideline-recommended therapeutic hypothermia decreased after publication of the Targeted Temperature Management trial, which supported more lenient temperature thresholds. Concurrent with this change, survival among patients admitted to the hospital decreased, but was not mediated by use of hypothermia.
Conflict of interest statement
Figures