Migration of an intrauterine device causing severe hydronephrosis progressing to renal failure: A case report
- PMID: 30653092
- PMCID: PMC6370023
- DOI: 10.1097/MD.0000000000013872
Migration of an intrauterine device causing severe hydronephrosis progressing to renal failure: A case report
Abstract
Rationale: Intrauterine device (IUD) is commonly used in China. Its complications include uterine perforation, IUD ectopic migration, etc. However, a migrated IUD rarely leads to renal failure.
Patient concerns: IUD insertion in the patient was followed by unexplained pain in the left renal area, without bladder irritation or dysuresia.
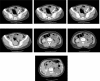
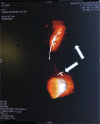
Diagnoses: Hydronephrosis, renal failure, migrated IUD.
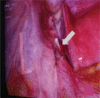
Interventions: The patient underwent laparoscopic and retroperitoneoscopic left nephrectomy, partial ureterectomy, and migrated IUD extraction.
Outcomes: No complications were found after 1 year of follow-up.
Lesson: An IUD should be placed by an experienced doctor. If conditions permit, it is best to perform the procedure under the guidance of ultrasound. The patients should be advised to undergo regular check-ups after the procedure. If necessary, abdominal color Doppler examination should be performed. Importantly, patients with IUD pregnancy must be reviewed.
Conflict of interest statement
The authors have no funding and conflicts of interest to disclose.
Figures



References
-
- Harrison-Woolrych M, Ashton J, Coulter D. Uterine perforation on intrauterine device insertion: is the incidence higher than previously reported? Contraception 2003;67:53–6. - PubMed
-
- Zakin D, Stern WZ, Rosenblatt R. Complete and partial uterine perforation and embedding following insertion of intrauterine devices. II. Diagnostic methods, prevention, and management. Obstet Gynecol Surv 1981;36:401–17. - PubMed
-
- Shen Suqi, Li Ying Analysis of adverse events of ectopic iud in 90 cases. Chinese J Family Planning 2010;2:111–3.
-
- Tuncay YA, Tuncay E, Guzin K, et al. Transuterine migration as a complication of intrauterine contraceptive devices: six case reports. Eur J Contracept Reprod Health Care 2004;9:194–200. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources

