Associations between Lifetime Adversity and Obesity Treatment in Patients with Morbid Obesity
- PMID: 30654360
- PMCID: PMC6465708
- DOI: 10.1159/000494333
Associations between Lifetime Adversity and Obesity Treatment in Patients with Morbid Obesity
Abstract
Background: Bariatric surgery is associated with greater and more sustainable weight loss compared with lifestyle intervention programs. On the other hand, bariatric surgery may also be associated with physical and psychosocial complications. The influence of psychological evaluation on treatment choice, however, is not known. We aimed to examine variables associated with treatment choice and, specifically, if self-reported lifetime adversity influenced obesity treatment, i.e. bariatric surgery, high-intensive lifestyle treatment or low-intensive lifestyle treatment in primary care.
Methods: We consecutively included 924 patients from the registry study of patients with morbid obesity at Akershus University Hospital, Lørenskog, Norway. Treatment selection was made through a shared decision-making process. Self-reported lifetime adversity was registered by trained personnel. Logistic regression models were used to assess the associations between obesity treatment and possible predictors.
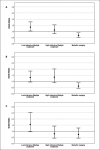
Results: Patients who chose bariatric surgery were more likely to have type 2 diabetes (DM2) compared with patients who chose lifestyle treatment (bariatric surgery: 35%, high-intensive lifestyle treatment: 26%, and low-intensive lifestyle treatment: 26%; p = 0.035). Patients who chose bariatric surgery were less likely than patients who chose lifestyle intervention to report lifetime adversity (bariatric surgery: 39%, high-intensive lifestyle treatment: 47%, and low-intensive lifestyle treatment: 51%; p = 0.004). After multivariable adjustments, increasing BMI, having DM2, and joint pain were associated with choosing bariatric surgery over non-surgical obesity treatment (odds ratio [95% CI]: BMI 1.03 [1.01-1.06], DM2 1.47 [1.09-1.99], and joint pain 1.46 [1.08-1.96]). Self-reported lifetime adversity was furthermore associated with lower odds of choosing bariatric surgery in patients with morbid obesity (0.67 [0.51-0.89]).
Conclusion: This study shows that increasing BMI, DM2, and joint pain were all associated with treatment choice for obesity. In addition, self-reported lifetime adversity was associated with the patients' treatment choice for morbid obesity. Consequently, we suggest that decisions concerning obesity treatment should include dialogue-based assessments of the patients' lifetime adversity.
Keywords: Bariatric surgery; Eating behavior; Obesity; Psychological aspects; Stress overnutrition.
© 2019 The Author(s) Published by S. Karger AG, Basel.
Figures
References
-
- Pischon T, Boeing H, Hoffmann K, Bergmann M, Schulze MB, Overvad K, et al. General and abdominal adiposity and risk of death in Europe. N Engl J Med. 2008 Nov;359((20)):2105–20. - PubMed
-
- Aftab H, Risstad H, Søvik TT, Bernklev T, Hewitt S, Kristinsson JA, et al. Five-year outcome after gastric bypass for morbid obesity in a Norwegian cohort. Surg Obes Relat Dis. 2014 Jan-Feb;10((1)):71–8. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources