Hospital organizational context and delivery of evidence-based stroke care: a cross-sectional study
- PMID: 30658654
- PMCID: PMC6339367
- DOI: 10.1186/s13012-018-0849-z
Hospital organizational context and delivery of evidence-based stroke care: a cross-sectional study
Erratum in
-
Correction to: Hospital organizational context and delivery of evidence-based stroke care: a cross-sectional study.Implement Sci. 2019 Feb 8;14(1):13. doi: 10.1186/s13012-019-0862-x. Implement Sci. 2019. PMID: 30736790 Free PMC article.
Abstract
Background: Organizational context is one factor influencing the translation of evidence into practice, but data pertaining to patients with acute stroke are limited. We aimed to determine the associations of organizational context in relation to four important evidence-based stroke care processes.
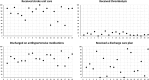
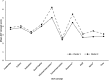
Methods: This was a mixed methods cross-sectional study. Among 19 hospitals in Queensland, Australia, a survey was conducted of the perceptions of stroke clinicians about their work using the Alberta Context Tool (ACT), a validated measure covering 10 concepts of organizational context, and with additional stroke-specific contextual questions. These data were linked to the Australian Stroke Clinical Registry (AuSCR) to determine the relationship with receipt of evidence-based acute stroke care (acute stroke unit admission, use of thrombolysis for those with acute ischemic stroke, receipt of a written care plan on discharge, and prescription of antihypertensive medications on discharge) using quantile regression. Exploratory cluster analysis was used to categorize hospitals into high and low context groups based on all of the 10 ACT concepts. Differences in adherence to care processes between the two groups were examined.
Results: A total of 215 clinicians completed the survey (50% nurses, 37% allied health staff, 10% medical practitioners), with 81% being in their current role for at least 1 year. There was good reliability (∞ 0.83) within the cohort to allow pooling of professional groups. Greater ACT scores, especially for social capital (μ 9.00, 95% confidence interval [CI] 4.86 to 13.14) and culture (μ 7.33, 95% CI 2.05 to 12.62), were associated with more patients receiving stroke unit care. There was no correlation between ACT concepts and other care processes. Working within higher compared to lower context environments was associated with greater proportions of patients receiving stroke unit care (88.5% vs. 69.0%) and being prescribed antihypertensive medication at discharge (62.5% vs. 52.0%). Staff from higher context hospitals were more likely to value medical and/or nursing leadership and stroke care protocols.
Conclusions: Overall organizational context, and in particular aspects of culture and social capital, are associated with the delivery of some components of evidence-based stroke care, offering insights into potential pathways for improving the implementation of proven therapies.
Keywords: Evidence-based care; Organizational context; Stroke; Stroke unit.
Conflict of interest statement
Ethics approval and consent to participate
The study was approved by the Metro South Human Research Ethics Committee (HREC/13/QPAH/31) and Monash University (CF13/1303-2013000641), and each participating hospital provided site governance authorization. Participating clinicians provided implied consent through the anonymous completion of the survey. The AuSCR has ethics approval to use an opt-out method of consent for collection of patient clinical data.
Consent for publication
Not applicable
Competing interests
SM is a member of the Research Committee of National Health and Medical Research Council (NHMRC) of Australia, but her appointment post-dated receipt of funding for this study. All other authors declare that they have no competing interests.
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Figures

References
-
- Feigin VL, Roth GA, Naghavi M, Parmar P, Krishnamurthi R, Chugh S, Mensah GA, Norrving B, Shiue I, Ng M, et al. Global burden of stroke and risk factors in 188 countries, during 1990–2013: a systematic analysis for the Global Burden of Disease Study 2013. Lancet Neurol. 2016;15(9):913–924. doi: 10.1016/S1474-4422(16)30073-4. - DOI - PubMed
-
- Stroke Foundation . Stroke audit – acute services report. Melbourne: Stroke Foundation; 2017. p. 78.
-
- Stroke Foundation . Clinical guidelines for stroke management 2017. Melbourne: Stroke Foundation; 2017. p. 168.
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Research Materials

