Level of agreement of point-of-care and laboratory HbA1c measurements in the preoperative outpatient clinic in non-diabetic patients who are overweight or obese
- PMID: 30659411
- PMCID: PMC6823319
- DOI: 10.1007/s10877-019-00255-6
Level of agreement of point-of-care and laboratory HbA1c measurements in the preoperative outpatient clinic in non-diabetic patients who are overweight or obese
Abstract
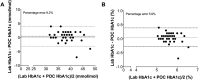
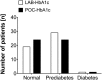
Implementation of point-of-care HbA1c devices in the preoperative outpatient clinic might facilitate the early diagnosis of glycemic disturbances in overweight or obese patients undergoing surgery, but validation studies in this setting do not exist. We determined the level of agreement between a point-of-care and laboratory HbA1c test in non-diabetic patients visiting the outpatient clinic for preoperative risk profiling. Point-of-care HbA1c levels were measured in whole blood obtained by a finger prick (Siemens DCA Vantage HbA1c analyzer) and in hemolysed EDTA blood in the central laboratory (LAB). Bland Altman and Clarke's error grid analysis were used to analyze the agreement between the point-of-care and laboratory measurements. Patients (n = 49) were 55 ± 11 years old, 47% were male with a body mass index (BMI) of 30.6 ± 3.4 kg/m2. The mean HbA1c was 38.1 ± 3.7 mmol/mol or 5.6 ± 0.3%. One patient was diagnosed with a HbA1c indicative for diabetes mellitus (6.7%). Bland Altman analysis revealed a bias of - 0.53 ± 1.81 mmol/mol with limits of agreement of - 4.09 to 3.03 mmol/mol and a bias of - 0.05 ± 0.17% with limits of agreement - 0.39 to 0.28%. The percentage error was 9.2% and 5.9% for HbA1c expressed in mmol/mol and %, respectively. Clarke's error grid analysis showed that 48 out of 49 measurements were located in area A (98%). Point-of-care HbA1c measurements showed a high level of agreement with the laboratory test in the outpatient setting, and may be used for preoperative risk profiling in patients prone to cardiometabolic complications.Trial registration: Netherlands Trial Register NTR3057.
Keywords: Anesthesia; Diabetes; Glucose; Obesity; Preoperative screening.
Conflict of interest statement
The authors declare that they have no conflict of interest.
Figures

Similar articles
-
[Diagnostic agreement between two glycosylated a1b hemoglobin methods in Primary Care].Semergen. 2014 Nov-Dec;40(8):431-5. doi: 10.1016/j.semerg.2014.01.012. Epub 2014 Apr 4. Semergen. 2014. PMID: 24708908 Spanish.
-
Measurement of HbA1c in multicentre diabetes trials - should blood samples be tested locally or sent to a central laboratory: an agreement analysis.Trials. 2016 Oct 24;17(1):517. doi: 10.1186/s13063-016-1640-6. Trials. 2016. PMID: 27776543 Free PMC article. Clinical Trial.
-
Assessment of Two Diabetes Point-of-care Analyzers Measuring Hemoglobin A1c in the Peruvian Amazon.Ann Glob Health. 2018 Nov 5;84(4):618-624. doi: 10.9204/aogh.2368. Ann Glob Health. 2018. PMID: 30779508 Free PMC article.
-
Accuracy of point-of-care HbA1c testing in pregnant women.Aust N Z J Obstet Gynaecol. 2018 Dec;58(6):643-647. doi: 10.1111/ajo.12786. Epub 2018 Feb 22. Aust N Z J Obstet Gynaecol. 2018. PMID: 29468638
-
Point-of-Care Hemoglobin A1c Testing: An Evidence-Based Analysis.Ont Health Technol Assess Ser. 2014 Jul 1;14(8):1-30. eCollection 2014. Ont Health Technol Assess Ser. 2014. PMID: 26316922 Free PMC article. Review.
Cited by
-
Level of Agreement and Correlation Between the Estimated Hemoglobin A1c Results Derived by Continuous or Conventional Glucose Monitoring Systems Compared with the Point-of-Care or Laboratory-Based Measurements: An Observational Study.Diabetes Ther. 2022 May;13(5):953-967. doi: 10.1007/s13300-022-01240-0. Epub 2022 Mar 20. Diabetes Ther. 2022. PMID: 35306640 Free PMC article.
-
Using point-of-care HbA1c to facilitate the identification of diabetes and abnormal glucose regulation in primary healthcare settings.Front Public Health. 2023 May 9;11:1078361. doi: 10.3389/fpubh.2023.1078361. eCollection 2023. Front Public Health. 2023. PMID: 37228727 Free PMC article.
-
Comparison of Point-of-Care and Laboratory Glycated Hemoglobin A1c and Its Relationship to Time-in-Range and Glucose Variability: A Real-World Study.Cureus. 2023 Jan 5;15(1):e33416. doi: 10.7759/cureus.33416. eCollection 2023 Jan. Cureus. 2023. PMID: 36643084 Free PMC article.
-
Protocol for a randomized controlled trial of sitting reduction to improve cardiometabolic health in older adults.Contemp Clin Trials. 2021 Dec;111:106593. doi: 10.1016/j.cct.2021.106593. Epub 2021 Oct 16. Contemp Clin Trials. 2021. PMID: 34666182 Free PMC article.
-
Derivation and validation of gray-box models to estimate noninvasive in-vivo percentage glycated hemoglobin using digital volume pulse waveform.Sci Rep. 2021 Jun 9;11(1):12169. doi: 10.1038/s41598-021-91527-2. Sci Rep. 2021. PMID: 34108531 Free PMC article.
References
-
- Obesity: preventing and managing the global epidemic. Report of a WHO consultation. World Health Organ Tech Rep Ser. 2000;894:1–253. - PubMed
-
- Yong PH, Weinberg L, Torkamani N, Churilov L, Robbins RJ, Ma R, Bellomo R, Lam QT, Burns JD, Hart GK, Lew JF, Mårtensson J, Story D, Motley AN, Johnson D, Zajac JD, Ekinci EI. The presence of diabetes and higher HbA1c are independently associated with adverse outcomes after surgery. Diabetes Care. 2018;41:1172–1179. doi: 10.2337/dc17-2304. - DOI - PubMed
Publication types
MeSH terms
Substances
Associated data
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

