Women receiving massive transfusion due to postpartum hemorrhage: A comparison over time between two nationwide cohort studies
- PMID: 30667050
- PMCID: PMC6593418
- DOI: 10.1111/aogs.13542
Women receiving massive transfusion due to postpartum hemorrhage: A comparison over time between two nationwide cohort studies
Abstract
Introduction: Incidence of massive transfusion after birth was high in the Netherlands between 2004 and 2006 compared with other high-income countries. This study investigated incidence, causes, management and outcome of women receiving massive transfusion due to postpartum hemorrhage in the Netherlands in more recent years.
Material and methods: Data for all pregnant women who received eight or more units of packed red blood cells from a gestational age of 20 weeks and within the first 24 hours after childbirth, during 2011 and 2012, were obtained from a nationwide retrospective cohort study, including 61 hospitals with a maternity unit in the Netherlands.
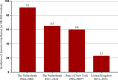
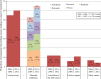
Results: Incidence of massive transfusion due to postpartum hemorrhage decreased to 65 per 100 000 births (95% CI 56-75) between 2011 and 2012, from 91 per 100 000 births (95% CI 81-101) between 2004 and 2006, while median blood loss increased from 4500 mL (interquartile range 3250-6000) to 6000 mL (interquartile range 4500-8000). Uterine atony remained the leading cause of hemorrhage. Thirty percent (53/176) underwent peripartum hysterectomy between 2011 and 2012, compared with 25% (83/327) between 2004 and 2006. Case fatality rate for women who received massive transfusion due to postpartum hemorrhage was 2.3% (4/176) between 2011 and 2012, compared with 0.9% (3/327) between 2004 and 2006.
Conclusions: The incidence of postpartum hemorrhage with massive transfusion decreased in the Netherlands between both time frames, but remained an important cause of maternal mortality and morbidity, including peripartum hysterectomy. National surveillance of maternal morbidity and mortality due to postpartum hemorrhage through an improved and continuous registration with confidential enquiries may lead to the identification of clear improvements of maternal care.
Keywords: blood transfusion; hysterectomy; morbidity; mortality; postpartum hemorrhage.
© 2019 The Authors. Acta Obstetricia et Gynecologica Scandinavica published by John Wiley & Sons Ltd on behalf of Nordic Federation of Societies of Obstetrics and Gynecology (NFOG).
Conflict of interest statement
No competing interests were reported by all authors.
Figures
References
-
- Ramler PI, van den Akker T, Henriquez D, Zwart JJ, van Roosmalen J. Incidence, management and outcome of women requiring massive transfusion after childbirth in the Netherlands: secondary analysis of a nationwide cohort study between 2004 and 2006. BMC Pregnancy Childbirth. 2017;17(1):197. - PMC - PubMed
-
- Green L, Knight M, Seeney FM, et al. The epidemiology and outcomes of women with postpartum haemorrhage requiring massive transfusion with eight or more units of red cells: a national cross‐sectional study. BJOG. 2016;123(13):2164‐2170. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

