Pregnancy outcomes in women with kidney transplant: Metaanalysis and systematic review
- PMID: 30674290
- PMCID: PMC6345071
- DOI: 10.1186/s12882-019-1213-5
Pregnancy outcomes in women with kidney transplant: Metaanalysis and systematic review
Abstract
Background: Reproductive function in women with end stage renal disease generally improves after kidney transplant. However, pregnancy remains challenging due to the risk of adverse clinical outcomes.
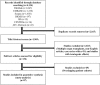
Methods: We searched PubMed/MEDLINE, Elsevier EMBASE, Scopus, BIOSIS Previews, ISI Science Citation Index Expanded, and the Cochrane Central Register of Controlled Trials from date of inception through August 2017 for studies reporting pregnancy with kidney transplant.
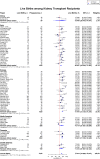
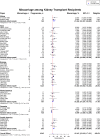
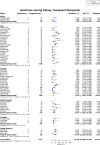
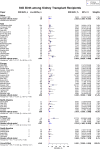
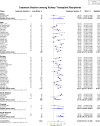
Results: Of 1343 unique studies, 87 met inclusion criteria, representing 6712 pregnancies in 4174 kidney transplant recipients. Mean maternal age was 29.6 ± 2.4 years. The live-birth rate was 72.9% (95% CI, 70.0-75.6). The rate of other pregnancy outcomes was as follows: induced abortions (12.4%; 95% CI, 10.4-14.7), miscarriages (15.4%; 95% CI, 13.8-17.2), stillbirths (5.1%; 95% CI, 4.0-6.5), ectopic pregnancies (2.4%; 95% CI, 1.5-3.7), preeclampsia (21.5%; 95% CI, 18.5-24.9), gestational diabetes (5.7%; 95% CI, 3.7-8.9), pregnancy induced hypertension (24.1%; 95% CI, 18.1-31.5), cesarean section (62.6, 95% CI 57.6-67.3), and preterm delivery was 43.1% (95% CI, 38.7-47.6). Mean gestational age was 34.9 weeks, and mean birth weight was 2470 g. The 2-3-year interval following kidney transplant had higher neonatal mortality, and lower rates of live births as compared to > 3 year, and < 2-year interval. The rate of spontaneous abortion was higher in women with mean maternal age < 25 years and > 35 years as compared to women aged 25-34 years.
Conclusion: Although the outcome of live births is favorable, the risks of maternal and fetal complications are high in kidney transplant recipients and should be considered in patient counseling and clinical decision making.
Keywords: Fetal; Kidney transplant; Maternal; Outcomes; Pregnancy.
Conflict of interest statement
Ethics approval and consent to participate
Not applicable.
Consent for publication
Not applicable.
Competing interests
All the authors have no disclosures and competing interests. The results presented in this paper have not been published previously in whole or part, except in abstract format.
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Figures







References
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

