Cancer screening rates among transgender adults: Cross-sectional analysis of primary care data
- PMID: 30674526
- PMCID: PMC6347308
Cancer screening rates among transgender adults: Cross-sectional analysis of primary care data
Abstract
Objective: To compare rates of cervical, breast, and colorectal cancer screening between patients who are transgender and those who are cisgender (ie, nontransgender).
Design: Cross-sectional study.
Setting: A multisite academic family health team in Toronto, Ont, serving more than 45 000 enrolled patients.
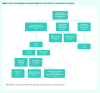
Participants: All patients enrolled in the family health team who were eligible for cervical, breast, or colorectal cancer screening. Patients were identified as transgender using an automated search of the practice electronic medical record followed by manual audit.
Main outcome measures: Screening rates for cervical, breast, and colorectal cancer calculated using data from the electronic medical record and provincial cancer screening registry. Screening rates among the transgender and cisgender populations were compared using 2 tests, and logistic regression modeling was used to understand differences in screening after adjustment for age, neighbourhood income quintile, and number of primary care visits.
Results: A total of 120 transgender patients were identified as eligible for cancer screening. More than 85% of transgender patients eligible for breast cancer screening were assigned male at birth. Transgender patients were less likely than cisgender patients (n = 20 514) were to be screened for cervical (56% vs 72%, P = .001; adjusted odds ratio [OR] of 0.39; 95% CI 0.25 to 0.62), breast (33% vs 65%, P < .001; adjusted OR = 0.27; 95% CI 0.12 to 0.59), and colorectal cancer (55% vs 70%, P = .046; adjusted OR = 0.50; 95% CI 0.26 to 0.99).
Conclusion: In this setting, transgender patients were less likely to receive recommended cancer screening compared with the cisgender population. Future research and quality improvement activities should aim to understand and address potential patient, provider, and system factors.
Objectif: Comparer les taux de dépistage des cancers colorectal, du col et du sein chez des patients transgenres par rapport à des patients cisgenres (c.-à-d. non transgenres).
Type d’étude: Une étude transversale.
Context: Une équipe universitaire multisite de santé familiale de Toronto, en Ontario, qui regroupe plus de 45 000 patients.
Participants: Tous les patients inscrits auprès de l’équipe de santé familiale qui étaient admissibles au dépistage des cancers colorectal, du col et du sein. Les patients ont été identifiés comme transgenres à l’aide d’une recherche automatisée dans les dossiers médicaux électroniques de la clinique, suivie d’une vérification manuelle.
Principaux paramètres à l’étude:
Les taux de dépistage des cancers colorectal, du col et du sein, calculés à partir des données des dossiers médicaux électroniques et du registre provincial sur le dépistage du cancer. Les taux de dépistage pour les transgenres et les patients cis ont été comparés à l’aide du test de  2, et la modélisation d’une régression logistique a permis de comprendre les différences de dépistage après ajustement pour l’âge, le niveau (quintile) de revenu du quartier et le nombre de visites à l’établissement de soins primaires.
2, et la modélisation d’une régression logistique a permis de comprendre les différences de dépistage après ajustement pour l’âge, le niveau (quintile) de revenu du quartier et le nombre de visites à l’établissement de soins primaires.
Résultats: Au total, 120 patients transgenres ont été considérés comme admissibles au dépistage du cancer. Parmi ces derniers, plus de 85 % avaient été déclarés de sexe mâle à la naissance. Par rapport aux patients cisgenres (n = 20 514), les transgenres étaient moins susceptibles de subir un dépistage pour le col utérin (56 % c. 72 %. P = .001; rapport de cotes [RC] ajusté de 0.39; IC à 95 % 0.25 à 0.62), pour le sein (33 % c. 65 %, P = .001; RC ajusté = 0.27; IC à 95 % 0.12 à 0.59) et pour le cancer colorectal (55 % c. 70 %, P = .046; RC ajusté = 0.50; IC à 95 % 0.26 à 0.99).
Conclusion: Dans ce contexte, les patients transgenres étaient moins susceptibles que les cisgenres de recevoir les différents dépistages du cancer recommandés. Les recherches et les efforts futurs pour améliorer la situation devraient chercher à comprendre et à corriger les facteurs éventuels qui relèvent des patients, des soignants et du système.
Copyright© the College of Family Physicians of Canada.
Figures
References
-
- Gates GJ. How many people are lesbian, gay, bisexual and transgender? Los Angeles, CA: The Williams Institute; 2011.
-
- Winter S, Diamond M, Green J, Karasic D, Reed T, Whittle S, et al. Transgender people: health at the margins of society. Lancet. 2016;388(10042):390–400. Epub 2016 Jun 17. - PubMed
-
- Baker KE. The future of transgender coverage. N Engl J Med. 2017;376(19):1801–4. Epub 2017 Apr 5. - PubMed
-
- Barrett J. Doctors are failing to help people with gender dysphoria. BMJ. 2016;352:i1694. - PubMed