Hyperkalemia constitutes a constraint for implementing renin-angiotensin-aldosterone inhibition: the widening gap between mandated treatment guidelines and the real-world clinical arena
- PMID: 30675416
- PMCID: PMC6340904
- DOI: 10.1016/j.kisu.2016.01.004
Hyperkalemia constitutes a constraint for implementing renin-angiotensin-aldosterone inhibition: the widening gap between mandated treatment guidelines and the real-world clinical arena
Abstract
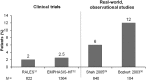
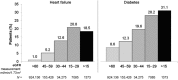
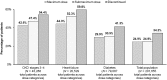
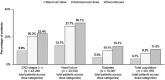
Recent studies have reported a large gap between the forceful and assertive recommendations in the guidelines and real-world practice in the use of renin-angiotensin-aldosterone inhibitors (RAASi) therapies. A comprehensive, retrospective analysis of a large database of electronic medical records (>7 million patients) was undertaken to evaluate 3 pivotal concerns: (i) whether RAASi are being prescribed according to treatment guidelines, (ii) what happens to RAASi prescriptions after hyperkalemia events, and (iii) what the clinical outcomes are in patients whose RAASi are discontinued or who are prescribed at doses lower than the guidelines recommend. The results indicate that a substantial gap exists between guideline recommendations and real-world prescribing patterns for RAASi. Among patients with cardiorenal comorbidities for which RAASi are recommended by the guidelines, more than one-half were prescribed lower-than-recommended doses, and approximately 14% to 16% discontinued RAASi therapy. RAASi prescribing patterns may be altered by the development of hyperkalemia. Moderate-to-severe hyperkalemia events were followed by down-titration or discontinuation of RAASi therapy in nearly one-half of all patients on maximal dose and by discontinuation in nearly one-third of patients on submaximal dose. This analysis highlights the challenge behind RAASi prescribing decisions, balancing the risk of provoking hyperkalemia with the benefits to reducing cardiorenal morbidity and mortality. Patients who are known to derive the greatest benefit from these drugs (chronic kidney disease patients with concomitant diabetes mellitus or heart failure) are the same patients who are at highest risk of developing hyperkalemia. These observations constitute a "call to action" to develop newer treatment modalities to lower serum potassium and to achieve and sustain normokalemia long-term.
Keywords: MR antagonism; cardiorenal comorbidities; chronic kidney disease; guideline recommendations for RAASi treatment; hyperkalemia; prescribing patterns for RAASi; renin-angiotensin inhibition; “big-data analytics”.
Figures

Similar articles
-
Real-World Associations of Renin-Angiotensin-Aldosterone System Inhibitor Dose, Hyperkalemia, and Adverse Clinical Outcomes in a Cohort of Patients With New-Onset Chronic Kidney Disease or Heart Failure in the United Kingdom.J Am Heart Assoc. 2019 Nov 19;8(22):e012655. doi: 10.1161/JAHA.119.012655. Epub 2019 Nov 12. J Am Heart Assoc. 2019. PMID: 31711387 Free PMC article.
-
Discontinuation of Renin-Angiotensin-Aldosterone System Inhibitors Secondary to Hyperkalemia Translates into Higher Cardiorenal Outcomes.Am J Nephrol. 2023;54(7-8):258-267. doi: 10.1159/000531102. Epub 2023 May 18. Am J Nephrol. 2023. PMID: 37231821 Free PMC article.
-
Management of RAASi-associated hyperkalemia in patients with cardiovascular disease.Heart Fail Rev. 2021 Jul;26(4):891-896. doi: 10.1007/s10741-020-10069-3. Epub 2021 Feb 18. Heart Fail Rev. 2021. PMID: 33599908 Free PMC article. Review.
-
Real-World Modifications of Renin-Angiotensin-Aldosterone System Inhibitors in Patients with Hyperkalemia Initiating Sodium Zirconium Cyclosilicate Therapy: The OPTIMIZE I Study.Adv Ther. 2023 Jun;40(6):2886-2901. doi: 10.1007/s12325-023-02518-w. Epub 2023 May 4. Adv Ther. 2023. PMID: 37140706 Free PMC article.
-
Optimally managing hyperkalemia in patients with cardiorenal syndrome.Nephrol Dial Transplant. 2019 Dec 1;34(Suppl 3):iii36-iii44. doi: 10.1093/ndt/gfz225. Nephrol Dial Transplant. 2019. PMID: 31800079 Review.
Cited by
-
The Cost Effectiveness of Patiromer for the Treatment of Hyperkalaemia in Patients with Chronic Kidney Disease with and without Heart Failure in Ireland.Pharmacoecon Open. 2022 Sep;6(5):757-771. doi: 10.1007/s41669-022-00357-z. Epub 2022 Aug 4. Pharmacoecon Open. 2022. PMID: 35925491 Free PMC article.
-
Hyperkalemia with Mineralocorticoid Receptor Antagonist Use in People with CKD: Understanding and Mitigating the Risks.Clin J Am Soc Nephrol. 2022 Mar;17(3):455-457. doi: 10.2215/CJN.13541021. Epub 2021 Dec 1. Clin J Am Soc Nephrol. 2022. PMID: 34853060 Free PMC article. No abstract available.
-
Endothelial dysfunction in the kidney transplant population: Current evidence and management strategies.World J Transplant. 2025 Mar 18;15(1):97458. doi: 10.5500/wjt.v15.i1.97458. World J Transplant. 2025. PMID: 40104196 Free PMC article. Review.
-
Risk-Benefit Balance of Renin-Angiotensin-Aldosterone Inhibitor Cessation in Heart Failure Patients with Hyperkalemia.J Clin Med. 2022 Sep 30;11(19):5828. doi: 10.3390/jcm11195828. J Clin Med. 2022. PMID: 36233692 Free PMC article.
-
Binding Potassium to Improve Treatment With Renin-Angiotensin-Aldosterone System Inhibitors: Results From Multiple One-Stage Pairwise and Network Meta-Analyses of Clinical Trials.Front Med (Lausanne). 2021 Aug 19;8:686729. doi: 10.3389/fmed.2021.686729. eCollection 2021. Front Med (Lausanne). 2021. PMID: 34490289 Free PMC article.
References
-
- Ferrario C.M., Strawn W.B. Role of the renin-angiotensin-aldosterone system and proinflammatory mediators in cardiovascular disease. Am J Cardiol. 2006;98:121–128. - PubMed
-
- Shearer F., Lang C.C., Struthers A.D. Renin-angiotensin-aldosterone system inhibitors in heart failure. Clin Pharmacol Ther. 2013;94:459–467. - PubMed
-
- Hsu T.W., Liu J.S., Hung S.C. Renoprotective effect of renin-angiotensin-aldosterone system blockade in patients with predialysis advanced chronic kidney disease, hypertension, and anemia. JAMA Intern Med. 2014;174:347–354. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Other Literature Sources
Miscellaneous

