Association of Primary Care Providers' Beliefs of Statins for Primary Prevention and Statin Prescription
- PMID: 30681391
- PMCID: PMC6405576
- DOI: 10.1161/JAHA.118.010241
Association of Primary Care Providers' Beliefs of Statins for Primary Prevention and Statin Prescription
Abstract
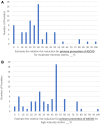
Background The 2013 American College of Cardiology/American Heart Association Cholesterol Treatment Guideline increased the number of primary prevention patients eligible for statin therapy, yet uptake of these guidelines has been modest. Little is known of how primary care provider ( PCP ) beliefs influence statin prescription. Methods and Results We surveyed 164 PCP s from a community-based North Carolina network in 2017 about statin therapy. We evaluated statin initiation among the PCP s' statin-eligible patients between 2014 and 2015 without a previous prescription. Seventy-two PCP s (43.9%) completed the survey. The median estimate of the relative risk reduction for high-intensity statins was 45% (interquartile range, 25%-50%). A minority of providers (27.8%) believed statins caused diabetes mellitus, and only 16.7% reported always/very often discussing this with patients. Most PCPs (97.2%) believed that statins cause myopathy, and 72.3% reported always/very often discussing this with patients. Most (77.7%) reported always/very often using the 10-year atherosclerotic cardiovascular disease risk calculator, although many reported that in most cases other risk factors or patient preferences influenced prescribing (59.8% and 43.1%, respectively). Of 6172 statin-eligible patients, 22.3% received a prescription for a moderate- or high-intensity statin at follow-up. Providers reporting greater reliance on risk factors beyond atherosclerotic cardiovascular disease risk were less likely to prescribe statins. Conclusions Although beliefs and approaches to statin discussions vary among community PCP s, new prescription rates are low and minimally associated with those beliefs. These results highlight the complexity of increasing statin prescriptions for primary prevention and suggest that strategies to facilitate standardized discussions and to address external influences on patient beliefs warrant future study.
Keywords: guideline adherence; prevention; shared decision making; statin.
Figures
References
-
- Stone NJ, Robinson JG, Lichtenstein AH, Bairey Merz CN, Blum CB, Eckel RH, Goldberg AC, Gordon D, Levy D, Lloyd‐Jones DM, McBride P, Schwartz JS, Shero ST, Smith SC Jr, Watson K, Wilson PW, Eddleman KM, Jarrett NM, LaBresh K, Nevo L, Wnek J, Anderson JL, Halperin JL, Albert NM, Bozkurt B, Brindis RG, Curtis LH, DeMets D, Hochman JS, Kovacs RJ, Ohman EM, Pressler SJ, Sellke FW, Shen WK, Smith SC Jr, Tomaselli GF; American College of Cardiology/American Heart Association Task Force on Practice Guidelines . ACC/AHA guideline on the treatment of blood cholesterol to reduce atherosclerotic cardiovascular risk in adults: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. Circulation. 2013;2013:S1–S45. - PubMed
-
- Pencina MJ, Navar‐Boggan AM, D'Agostino RB Sr, Williams K, Neely B, Sniderman AD, Peterson ED. Application of new cholesterol guidelines to a population‐based sample. N Engl J Med. 2014;370:1422–1431. - PubMed
-
- Rosenson RS, Kent ST, Brown TM, Farkouh ME, Levitan EB, Yun H, Sharma P, Safford MM, Kilgore M, Muntner P, Bittner V. Underutilization of high‐intensity statin therapy after hospitalization for coronary heart disease. J Am Coll Cardiol. 2015;65:270–277. - PubMed
-
- Olufade T, Zhou S, Anzalone D, Kern DM, Tunceli O, Cziraky MJ, Willey VJ. Initiation patterns of statins in the 2 years after release of the 2013 American College of Cardiology/American Heart Association (ACC/AHA) Cholesterol Management Guideline in a large US health plan. J Am Heart Assoc. 2017;6:e005205 DOI: 10.1161/JAHA.116.005205. - DOI - PMC - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical