Comparison of intramedullary nailing and plate fixation in distal tibial fractures with metaphyseal damage: a meta-analysis of randomized controlled trials
- PMID: 30683118
- PMCID: PMC6347848
- DOI: 10.1186/s13018-018-1037-1
Comparison of intramedullary nailing and plate fixation in distal tibial fractures with metaphyseal damage: a meta-analysis of randomized controlled trials
Abstract
Background: Distal metadiaphyseal tibial fractures are commonly seen lower limb fractures. Intramedullary nail fixation (IMN) and plate internal fixation (PL) are the two mainstay treatments for tibial fractures, but agreement on the best internal fixation for distal tibial fractures is still controversial. This meta-analysis was designed to compare the success of IMN and PL fixations in the treatment of distal metadiaphyseal tibial fractures, in terms of complications and functional recovery.
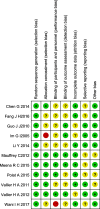
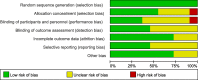
Methods: A systematic research of the literature was conducted to identify relevant articles that were published in PubMed, MEDLINE, Embase, the Cochrane Library, SpringerLink, Clinical Trials.gov, and OVID from the database inception to August 2018. All studies comparing the complication rate and functional improvement of I2MN and PL were included. Data on the 12 main outcomes were collected and analyzed using the Review Manager 5.3.
Results: Eleven studies were included in the current meta-analysis. A significant difference in malunion (RR = 1.76, 95%CI 1.21-2.57, P = 0.003), superficial infection (RR = 0.29, 95%CI 0.13-0.63, P = 0.002), FFI (MD = 0.09, 95%CI 0.01-0.17, P = 0.02), and knee pain (RR = 3.85, 95%CI 2.07-7.16, P < 0.0001) was noted between the IMN group and PL group. No significant difference was seen in the operation time (MD = - 10.46, 95%CI - 21.69-0.77, P = 0.07), radiation time (MD = 7.95, 95%CI - 6.65-22.55, P = 0.29), union time (MD = - 0.21, 95%Cl - 0.82-0.40, P = 0.49.), nonunion (RR = 2.17,95%CI 0.79-5.99, P = 0.15), deep infection (RR = 0.85, 95%CI 0.35-2.06, P = 0.72), delay union (RR = 0.92, 95%CI 0.45-1.87, P = 0.82), AOFAS (MD 1.26, 95%Cl - 1.19-3.70, P = 0.31), and Disability Rating Index in 6 or 12 months (MD = - 3.75, 95%CI - 9.32-1.81, P = 0.19, MD = - 17.11, 95%CI - 59.37-25.16, P = 0.43, respectively).
Conclusions: Although no significant difference was seen between IMN and PL fixation with regards to the operation time, radiation time, nonunion, deep infection delay union, union time, AOFAS, and Disability Rating Index, significant differences were seen in occurrence of malunion, superficial infection, FFI, and knee pain. Based on this evidence, IMN appears to be a superior choice for functional improvement of the ankle and reduction of postoperative wound superficial infection. PL internal fixation seems to be more advantageous in achieving anatomical reduction and decreasing knee pain.
Keywords: Distal metaphyseal fractures; Distal tibial fracture; Intramedullary nail; Plate.
Conflict of interest statement
Ethics approval and consent to participate
Not applicable.
Consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing interests.
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Figures

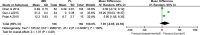




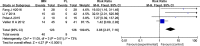


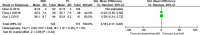
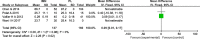

Similar articles
-
Comparing intramedullary nailing and plate fixation for treating distal tibail fractures: A meta-analysis of randomized controlled trials.Int J Surg. 2018 May;53:5-11. doi: 10.1016/j.ijsu.2018.03.026. Epub 2018 Mar 16. Int J Surg. 2018. PMID: 29555519 Review.
-
Efficacy comparison between intramedullary nail fixation and plate fixation in distal tibia fractures: a meta-analysis of randomized controlled trials.J Orthop Surg Res. 2024 Jul 12;19(1):403. doi: 10.1186/s13018-024-04900-y. J Orthop Surg Res. 2024. PMID: 38997735 Free PMC article.
-
Intramedullary Nailing Versus Minimally Invasive Plate Osteosynthesis for Distal Tibial Fractures: A Systematic Review and Meta-Analysis.Orthop Surg. 2019 Dec;11(6):954-965. doi: 10.1111/os.12575. Orthop Surg. 2019. PMID: 31823496 Free PMC article.
-
Locked intramedullary nailing provides superior functional outcomes and lower complication rates than plate fixation of distal fibula fractures. A systematic review and meta-analysis of comparative studies.Foot Ankle Surg. 2022 Oct;28(7):986-994. doi: 10.1016/j.fas.2022.02.005. Epub 2022 Feb 12. Foot Ankle Surg. 2022. PMID: 35184992
-
Intramedullary nail versus plate treatments for distal tibial fractures: a meta-analysis.Int J Surg. 2015 Apr;16(Pt A):60-68. doi: 10.1016/j.ijsu.2015.02.004. Epub 2015 Feb 18. Int J Surg. 2015. PMID: 25701618
Cited by
-
Limb salvage and functional recovery in infected nonunion of the distal tibia treated with the Ilizarov techniques.J Clin Orthop Trauma. 2023 Sep 22;44:102255. doi: 10.1016/j.jcot.2023.102255. eCollection 2023 Sep. J Clin Orthop Trauma. 2023. PMID: 37817763 Free PMC article.
-
Clinical Efficacy of Minimally Invasive Elastic Stable Intramedullary Nailing for Limb Long Bone Fractures in Children.Orthop Surg. 2021 Jun;13(4):1336-1342. doi: 10.1111/os.12977. Epub 2021 May 7. Orthop Surg. 2021. PMID: 33961343 Free PMC article. Clinical Trial.
-
Optimal Design and Biomechanical Analysis of a Biomimetic Lightweight Design Plate for Distal Tibial Fractures: A Finite Element Analysis.Front Bioeng Biotechnol. 2022 Feb 21;10:820921. doi: 10.3389/fbioe.2022.820921. eCollection 2022. Front Bioeng Biotechnol. 2022. PMID: 35265599 Free PMC article.
-
Comparative Study of Minimally Invasive Plate Osteosynthesis (MIPO) and Intramedullary Nailing (IMN) for Treating Extraarticular Distal Tibial Fractures: Clinical and Radiological Outcomes.Med Sci Monit. 2023 Oct 16;29:e942154. doi: 10.12659/MSM.942154. Med Sci Monit. 2023. PMID: 37885268 Free PMC article.
-
Evaluation of femoral malrotation after intramedullary nailing.Int J Burns Trauma. 2021 Oct 15;11(5):418-423. eCollection 2021. Int J Burns Trauma. 2021. PMID: 34858723 Free PMC article.
References
-
- Wennergren D, Bergdahl C, Ekelund J. Epidemiology and incidence of tibia fractures in the Swedish fracture register [J] Injury. 2018;11:S0020138318304893. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

