Comorbid obstructive sleep apnoea and chronic obstructive pulmonary disease and the risk of cardiovascular disease
- PMID: 30687541
- PMCID: PMC6321895
- DOI: 10.21037/jtd.2018.10.117
Comorbid obstructive sleep apnoea and chronic obstructive pulmonary disease and the risk of cardiovascular disease
Abstract
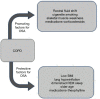
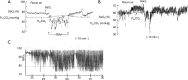
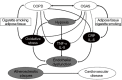
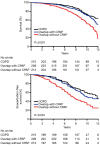
Chronic obstructive pulmonary disease (COPD) and obstructive sleep apnoea (OSA) syndrome are both highly prevalent, affecting at least 10% of the general adult population, and each has been independently associated with an increased risk of cardiovascular disease. The presence of both disorders together, commonly referred to as the overlap syndrome, is also highly prevalent, although various clinical and pathophysiological factors associated with COPD may increase or decrease the likelihood of OSA. Lung hyperinflation reduces the likelihood of obstructive apnoea, whereas right heart failure increases the likelihood as a result of rostral fluid shift causing upper airway narrowing in the supine position while asleep. Furthermore, upper airway inflammation associated with OSA may aggravate lower airway inflammation in COPD. The proposed mechanisms of cardiovascular disease in each disorder are similar and include systemic inflammation, oxidative stress, and sympathetic excitation. Thus, one could expect that the prevalence of co-morbid cardiovascular disease would be higher in the overlap syndrome but, with the exception of pulmonary hypertension, there are few published reports that have explored this aspect in depth. Hypoxia is more pronounced in patients with the overlap syndrome, especially during sleep, which is likely to be the principal factor accounting for the recognised higher prevalence of pulmonary hypertension in these patients. Cardiac sympathetic activity is increased in patients with the overlap syndrome when compared to each disorder alone, but echocardiographic evidence of left ventricular strain is no greater in overlap patients when compared to COPD alone. While survival might be expected to be worse in overlap patients, recent evidence surprisingly indicates that the incremental contribution of lung function to mortality diminishes with increasing severity of OSA. Identification of co-morbid OSA in patients with COPD has practical clinical significance as appropriate positive airway pressure therapy in COPD patients with co-existing OSA is associated with improved morbidity and mortality.
Keywords: Obstructive sleep apnoea (OSA); cardiovascular disease; chronic obstructive pulmonary disease (COPD); continuous positive airway pressure (CPAP); overlap syndrome.
Conflict of interest statement
Conflicts of Interest: The author has no conflicts of interest to declare.
Figures
Similar articles
-
Sleep disordered breathing: OSA-COPD overlap.Expert Rev Respir Med. 2024 Jun;18(6):369-379. doi: 10.1080/17476348.2024.2373790. Epub 2024 Jul 2. Expert Rev Respir Med. 2024. PMID: 38932721 Review.
-
Obstructive sleep apnea in chronic obstructive pulmonary disease patients.Curr Opin Pulm Med. 2011 Mar;17(2):79-83. doi: 10.1097/MCP.0b013e32834317bb. Curr Opin Pulm Med. 2011. PMID: 21169840 Review.
-
Chronic obstructive pulmonary disease and obstructive sleep apnoea-the overlap syndrome.J Thorac Dis. 2016 Feb;8(2):236-42. doi: 10.3978/j.issn.2072-1439.2016.01.52. J Thorac Dis. 2016. PMID: 26904264 Free PMC article. Review.
-
Integrating the overlap of obstructive lung disease and obstructive sleep apnoea: OLDOSA syndrome.Respirology. 2013 Apr;18(3):421-31. doi: 10.1111/resp.12062. Respirology. 2013. PMID: 23368952 Review.
-
Microalbuminuria in Patients with Obstructive Sleep Apnea-Chronic Obstructive Pulmonary Disease Overlap Syndrome.Ann Am Thorac Soc. 2016 Jun;13(6):917-25. doi: 10.1513/AnnalsATS.201510-655OC. Ann Am Thorac Soc. 2016. PMID: 26966922
Cited by
-
Symptomatic response to CPAP in obstructive sleep apnea versus COPD- obstructive sleep apnea overlap syndrome: Insights from a large national registry.PLoS One. 2021 Aug 12;16(8):e0256230. doi: 10.1371/journal.pone.0256230. eCollection 2021. PLoS One. 2021. PMID: 34383866 Free PMC article.
-
Lung structure and longitudinal change in cardiac structure and function: the MESA COPD Study.Eur Respir J. 2024 Dec 12;64(6):2400820. doi: 10.1183/13993003.00820-2024. Print 2024 Dec. Eur Respir J. 2024. PMID: 39362671 Free PMC article.
-
Effect of Nocturnal Oxygen on Blood Pressure Response to Altitude Exposure in COPD - Data from a Randomized Placebo-Controlled Cross-Over Trial.Int J Chron Obstruct Pulmon Dis. 2021 Dec 24;16:3503-3512. doi: 10.2147/COPD.S331658. eCollection 2021. Int J Chron Obstruct Pulmon Dis. 2021. PMID: 34992358 Free PMC article. Clinical Trial.
-
Heterogeneity of Melanoma Cell Responses to Sleep Apnea-Derived Plasma Exosomes and to Intermittent Hypoxia.Cancers (Basel). 2021 Sep 24;13(19):4781. doi: 10.3390/cancers13194781. Cancers (Basel). 2021. PMID: 34638272 Free PMC article.
-
Sympathetic and Vagal Nerve Activity in COPD: Pathophysiology, Presumed Determinants and Underappreciated Therapeutic Potential.Front Physiol. 2022 Jun 23;13:919422. doi: 10.3389/fphys.2022.919422. eCollection 2022. Front Physiol. 2022. PMID: 35845993 Free PMC article. Review.
References
Publication types
LinkOut - more resources
Full Text Sources
