Experimental and computational analyses reveal dynamics of tumor vessel cooption and optimal treatment strategies
- PMID: 30700544
- PMCID: PMC6377457
- DOI: 10.1073/pnas.1818322116
Experimental and computational analyses reveal dynamics of tumor vessel cooption and optimal treatment strategies
Abstract
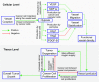
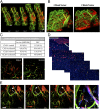
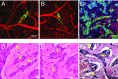
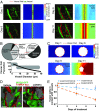
Cooption of the host vasculature is a strategy that some cancers use to sustain tumor progression without-or before-angiogenesis or in response to antiangiogenic therapy. Facilitated by certain growth factors, cooption can mediate tumor infiltration and confer resistance to antiangiogenic drugs. Unfortunately, this mode of tumor progression is difficult to target because the underlying mechanisms are not fully understood. Here, we analyzed the dynamics of vessel cooption during tumor progression and in response to antiangiogenic treatment in gliomas and brain metastases. We followed tumor evolution during escape from antiangiogenic treatment as cancer cells coopted, and apparently mechanically compressed, host vessels. To gain deeper understanding, we developed a mathematical model, which incorporated compression of coopted vessels, resulting in hypoxia and formation of new vessels by angiogenesis. Even if antiangiogenic therapy can block such secondary angiogenesis, the tumor can sustain itself by coopting existing vessels. Hence, tumor progression can only be stopped by combination therapies that judiciously block both angiogenesis and cooption. Furthermore, the model suggests that sequential blockade is likely to be more beneficial than simultaneous blockade.
Keywords: Ang2; VEGF; antiangiogenic treatment; glioblastoma; hypoxia.
Conflict of interest statement
Conflict of interest statement: R.K.J. received an honorarium from Amgen and consultant fees from Merck, Ophthotech, Pfizer, Sun Pharma Advanced Research Corporation (SPARC), SynDevRx, and XTuit; owns equity in Enlight, Ophthotech, and SynDevRx; and serves on the Boards of Trustees of Tekla Healthcare Investors, Tekla Life Sciences Investors, Tekla Healthcare Opportunities Fund, and Tekla World Healthcare Fund. No funding or reagents from these companies were used in these studies. N.D.K. completed the study more than 5 years ago and neither any reagent nor any funding from Novartis was used at the time.
Figures
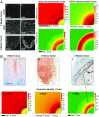

Similar articles
-
Tumor vessel biology in pediatric intracranial ependymoma.J Neurosurg Pediatr. 2010 Apr;5(4):335-41. doi: 10.3171/2009.11.PEDS09260. J Neurosurg Pediatr. 2010. PMID: 20367336
-
Role of collagen matrix in tumor angiogenesis and glioblastoma multiforme progression.Am J Pathol. 2013 Oct;183(4):1293-1305. doi: 10.1016/j.ajpath.2013.06.026. Epub 2013 Aug 5. Am J Pathol. 2013. PMID: 23928381 Free PMC article.
-
A tricistronic retroviral vector expressing natural antiangiogenic factors inhibits angiogenesis in vitro, but is not able to block tumor progression in vivo.Gene Ther. 2002 Feb;9(4):297-302. doi: 10.1038/sj.gt.3301652. Gene Ther. 2002. PMID: 11896469
-
Glioblastoma angiogenesis: VEGF resistance solutions and new strategies based on molecular mechanisms of tumor vessel formation.Brain Tumor Pathol. 2012 Apr;29(2):73-86. doi: 10.1007/s10014-011-0077-6. Epub 2012 Jan 6. Brain Tumor Pathol. 2012. PMID: 22218709 Review.
-
Angiogenesis in gliomas: biology and molecular pathophysiology.Brain Pathol. 2005 Oct;15(4):297-310. doi: 10.1111/j.1750-3639.2005.tb00115.x. Brain Pathol. 2005. PMID: 16389942 Free PMC article. Review.
Cited by
-
Inverting angiogenesis with interstitial flow and chemokine matrix-binding affinity.Sci Rep. 2022 Mar 10;12(1):4237. doi: 10.1038/s41598-022-08186-0. Sci Rep. 2022. PMID: 35273299 Free PMC article.
-
Real-Time Longitudinal Evaluation of Tumor Blood Vessels Using a Compact Preclinical Fluorescence Imaging System.Biosensors (Basel). 2021 Nov 23;11(12):471. doi: 10.3390/bios11120471. Biosensors (Basel). 2021. PMID: 34940228 Free PMC article.
-
TGF-β inhibition combined with cytotoxic nanomedicine normalizes triple negative breast cancer microenvironment towards anti-tumor immunity.Theranostics. 2020 Jan 12;10(4):1910-1922. doi: 10.7150/thno.36936. eCollection 2020. Theranostics. 2020. PMID: 32042344 Free PMC article.
-
Mesenchymal glioma stem cells trigger vasectasia-distinct neovascularization process stimulated by extracellular vesicles carrying EGFR.Nat Commun. 2024 Apr 3;15(1):2865. doi: 10.1038/s41467-024-46597-x. Nat Commun. 2024. PMID: 38570528 Free PMC article.
-
Differential stiffness between brain vasculature and parenchyma promotes metastatic infiltration through vessel co-option.Nat Cell Biol. 2024 Dec;26(12):2144-2153. doi: 10.1038/s41556-024-01532-6. Epub 2024 Oct 24. Nat Cell Biol. 2024. PMID: 39448802
References
-
- Wesseling P, van der Laak JA, de Leeuw H, Ruiter DJ, Burger PC. Quantitative immunohistological analysis of the microvasculature in untreated human glioblastoma multiforme. Computer-assisted image analysis of whole-tumor sections. J Neurosurg. 1994;81:902–909. - PubMed
-
- Pezzella F, Gatter K. Non-angiogenic tumours unveil a new chapter in cancer biology. J Pathol. 2015;235:381–383. - PubMed
-
- Donnem T, et al. Non-angiogenic tumours and their influence on cancer biology. Nat Rev Cancer. 2018;18:323–336. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

