Early reoperation following pancreaticoduodenectomy: impact on morbidity, mortality, and long-term survival
- PMID: 30704497
- PMCID: PMC6357503
- DOI: 10.1186/s12957-019-1569-9
Early reoperation following pancreaticoduodenectomy: impact on morbidity, mortality, and long-term survival
Abstract
Background: Reoperation following PD is a surrogate marker for a complex post-operative course and may lead to devastating consequences. We evaluate the indications for early reoperation following PD and analyze its effect on short- and long-term outcome.
Methods: Four hundred and thirty-three patients that underwent PD between August 2006 and June 2016 were retrospectively analyzed.
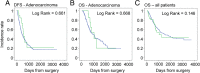
Results: Forty-eight patients (11%; ROp group) underwent 60 reoperations within 60 days from PD. Forty-two patients underwent 1 reoperation, and 6 had up to 6 reoperations. The average time to first reoperation was 10.1 ± 13.4 days. The most common indications were anastomotic leaks (22 operations in 18 patients; 37.5% of ROp), followed by post-pancreatectomy hemorrhage (PPH) (14 reoperations in 12 patients; 25%), and wound complications in 10 (20.8%). Patients with cholangiocarcinoma had the highest reoperation rate (25%) followed by ductal adenocarcinoma (12.3%). Reoperation was associated with increased length of hospital stay and a high post-operative mortality of 18.7%, compared to 2.6% for the non-reoperated group. For those who survived the post-operative period, the overall and disease-free survival were not affected by reoperation.
Conclusions: Early reoperations following PD carries a dramatically increased mortality rate, but has no impact on long-term survival.
Keywords: Complication; Pancreas; Surgery; Whipple.
Conflict of interest statement
Ethics approval and consent to participate
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. Informed consent was obtained from all individual participants included in the study.
Consent for publication
Not applicable
Competing interests
The authors declare that they have no competing interests.
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Figures
References
-
- Elberm H, Ravikumar R, Sabin C, Abu Hilal M, Al-Hilli A, Aroori S, et al. Outcome after pancreaticoduodenectomy for T3 adenocarcinoma: a multivariable analysis from the UK vascular resection for pancreatic Cancer study group. Eur J Surg Oncol. 2015;41(11):1500–1507. doi: 10.1016/j.ejso.2015.08.158. - DOI - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical