Prehospital transdermal glyceryl trinitrate in patients with ultra-acute presumed stroke (RIGHT-2): an ambulance-based, randomised, sham-controlled, blinded, phase 3 trial
- PMID: 30738649
- PMCID: PMC6497986
- DOI: 10.1016/S0140-6736(19)30194-1
Prehospital transdermal glyceryl trinitrate in patients with ultra-acute presumed stroke (RIGHT-2): an ambulance-based, randomised, sham-controlled, blinded, phase 3 trial
Abstract
Background: High blood pressure is common in acute stroke and is a predictor of poor outcome; however, large trials of lowering blood pressure have given variable results, and the management of high blood pressure in ultra-acute stroke remains unclear. We investigated whether transdermal glyceryl trinitrate (GTN; also known as nitroglycerin), a nitric oxide donor, might improve outcome when administered very early after stroke onset.
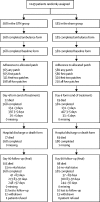
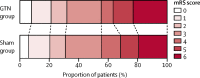
Methods: We did a multicentre, paramedic-delivered, ambulance-based, prospective, randomised, sham-controlled, blinded-endpoint, phase 3 trial in adults with presumed stroke within 4 h of onset, face-arm-speech-time score of 2 or 3, and systolic blood pressure 120 mm Hg or higher. Participants were randomly assigned (1:1) to receive transdermal GTN (5 mg once daily for 4 days; the GTN group) or a similar sham dressing (the sham group) in UK-based ambulances by paramedics, with treatment continued in hospital. Paramedics were unmasked to treatment, whereas participants were masked. The primary outcome was the 7-level modified Rankin Scale (mRS; a measure of functional outcome) at 90 days, assessed by central telephone follow-up with masking to treatment. Analysis was hierarchical, first in participants with a confirmed stroke or transient ischaemic attack (cohort 1), and then in all participants who were randomly assigned (intention to treat, cohort 2) according to the statistical analysis plan. This trial is registered with ISRCTN, number ISRCTN26986053.
Findings: Between Oct 22, 2015, and May 23, 2018, 516 paramedics from eight UK ambulance services recruited 1149 participants (n=568 in the GTN group, n=581 in the sham group). The median time to randomisation was 71 min (IQR 45-116). 597 (52%) patients had ischaemic stroke, 145 (13%) had intracerebral haemorrhage, 109 (9%) had transient ischaemic attack, and 297 (26%) had a non-stroke mimic at the final diagnosis of the index event. In the GTN group, participants' systolic blood pressure was lowered by 5·8 mm Hg compared with the sham group (p<0·0001), and diastolic blood pressure was lowered by 2·6 mm Hg (p=0·0026) at hospital admission. We found no difference in mRS between the groups in participants with a final diagnosis of stroke or transient ischaemic stroke (cohort 1): 3 (IQR 2-5; n=420) in the GTN group versus 3 (2-5; n=408) in the sham group, adjusted common odds ratio for poor outcome 1·25 (95% CI 0·97-1·60; p=0·083); we also found no difference in mRS between all patients (cohort 2: 3 [2-5]; n=544, in the GTN group vs 3 [2-5]; n=558, in the sham group; 1·04 [0·84-1·29]; p=0·69). We found no difference in secondary outcomes, death (treatment-related deaths: 36 in the GTN group vs 23 in the sham group [p=0·091]), or serious adverse events (188 in the GTN group vs 170 in the sham group [p=0·16]) between treatment groups.
Interpretation: Prehospital treatment with transdermal GTN does not seem to improve functional outcome in patients with presumed stroke. It is feasible for UK paramedics to obtain consent and treat patients with stroke in the ultra-acute prehospital setting.
Funding: British Heart Foundation.
Copyright © 2019 The Author(s). Published by Elsevier Ltd. This is an Open Access article under the CC BY 4.0 license. Published by Elsevier Ltd.. All rights reserved.
Figures

Comment in
-
Considering prehospital stroke trials: did RIGHT-2 get it right?Lancet. 2019 Mar 9;393(10175):963-965. doi: 10.1016/S0140-6736(19)30276-4. Epub 2019 Feb 6. Lancet. 2019. PMID: 30738650 No abstract available.
References
-
- Bath PM, Appleton JP, Krishnan K, Sprigg N. Blood pressure in acute stroke: to treat or not to treat: that is still the question. Stroke. 2018;49:1784–1790. - PubMed
-
- Intercollegiate Stroke Working Party . 5th edn. Royal College of Physicians; London: 2016. National clinical guideline for stroke.
-
- Willmot M, Gray L, Gibson C, Murphy S, Bath PMW. A systematic review of nitric oxide donors and L-arginine in experimental stroke; effects on infarct size and cerebral blood flow. Nitric Oxide. 2005;12:141–149. - PubMed
-
- Ferlito S, Gallina M, Pitari GM, Bianchi A. Nitric oxide plasma levels in patients with chronic and acute cerebrovascular disorders. Panminerva Med. 1998;40:51–54. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

